The program includes:
- Initial presentation in the clinic
- clinical history taking
- general physical examination
- laboratory tests:
- complete blood count
- biochemical analysis of blood
- urinalysis
- TSH-basal, fT3, fT4
- PSA blood level
- tests for urogenital infections
- indicators of inflammation
- indicators of blood coagulation
- ultrasound scan of the urogenital system
- renal scintigraphy
- PSMA PET-CT
- PSMA treatment with Actinium-225
- full body scintigraphy after 24 hours
- full body scintigraphy after 48 hours
- symptomatic treatment
- cost of essential medicines
- nursing services
- elaboration of further recommendations
- stay in the hospital with full board
- accommodation in 2-bedded room
How program is carried out
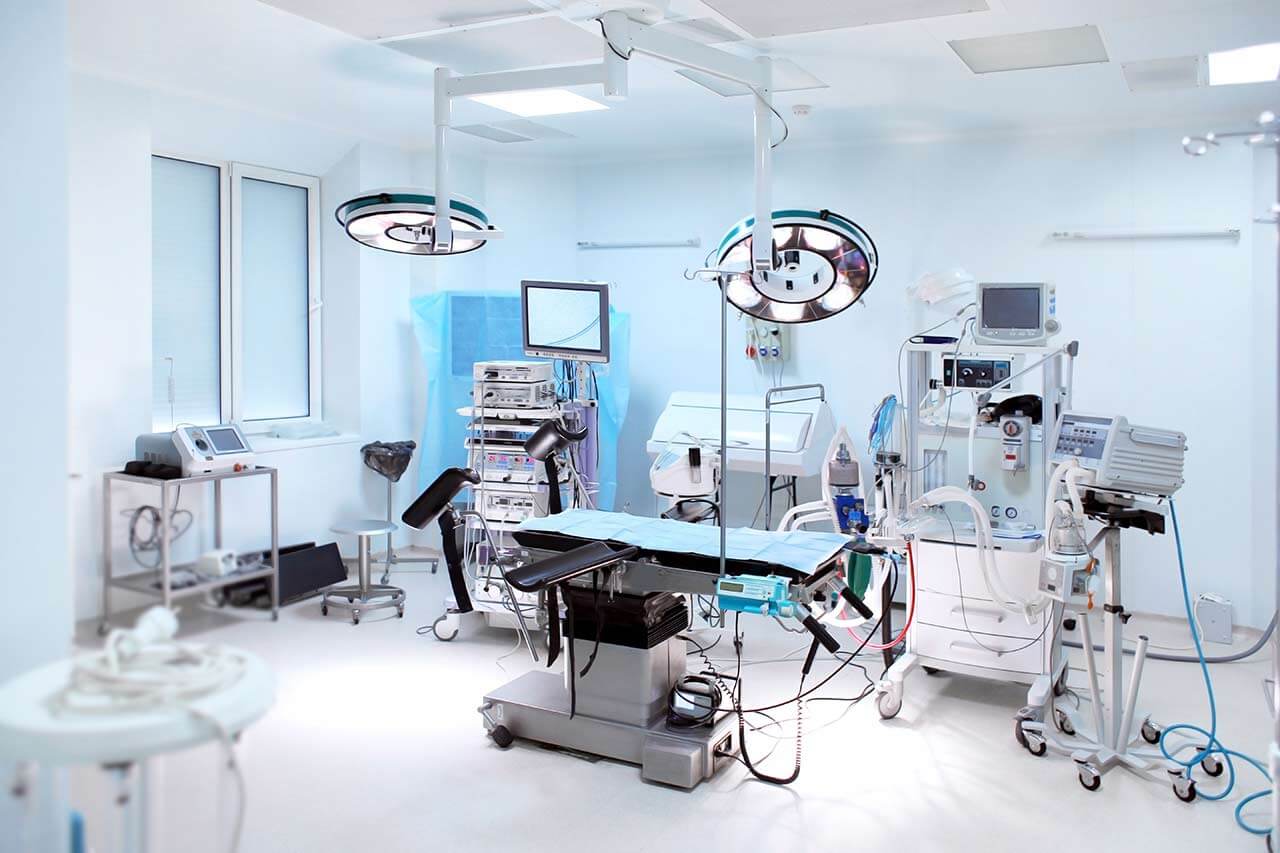
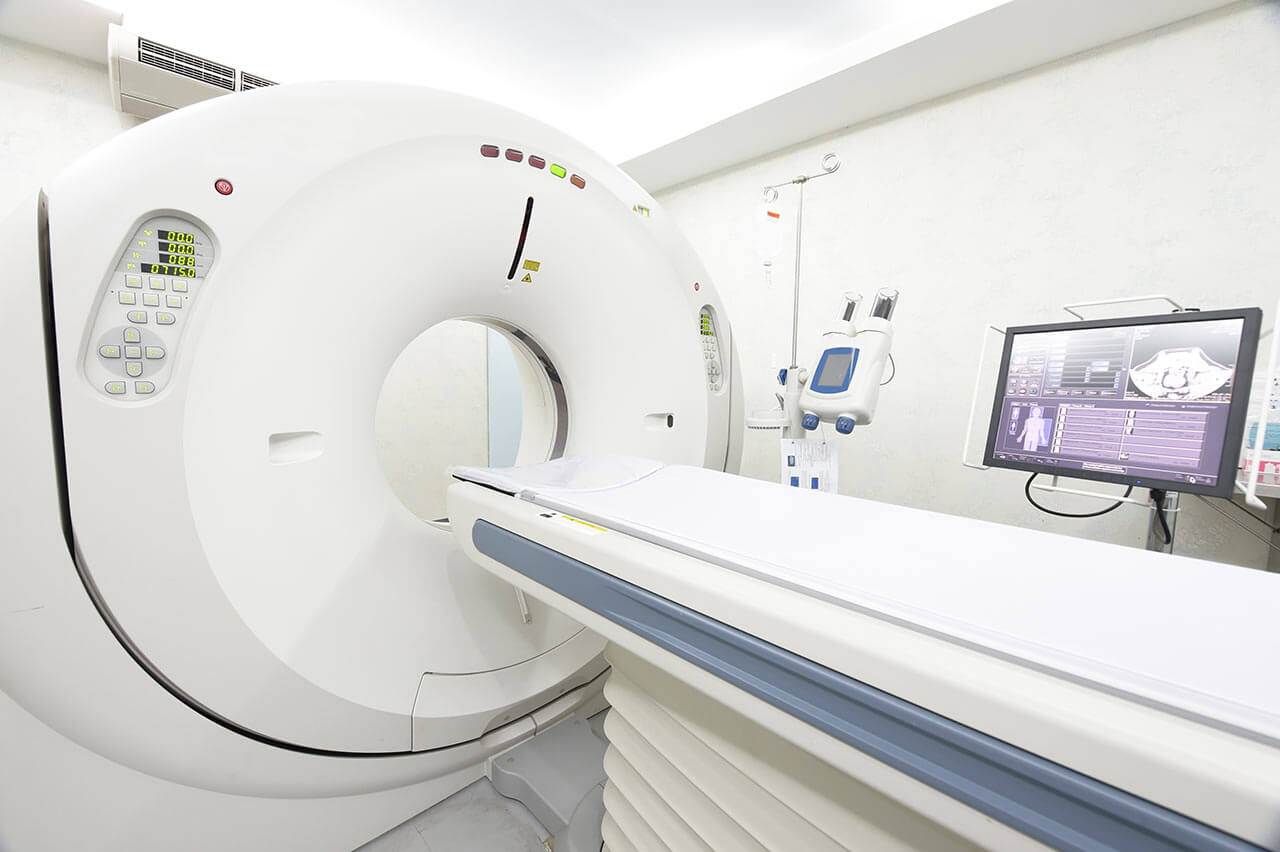
During the first visit, the doctor will carry out a general physical examination and go through the results of previous laboratory and instrumental tests. After that, you will undergo the necessary additional tests such as the assessment of liver and kidney function, scintigraphy of the skeleton and salivary glands, PSMA PET / CT. This will allow the doctor to assess how effective PSMA therapy with Actinium-225 will be and how well you will tolerate it. Also, the doctor will calculate your individual dosage of the radionuclide.
PSMA therapy with Actinium-225 is carried out via intravenous administration of a solution with the radioactive isotope Actinium-225. The solution is injected through a catheter. This is a short procedure, as the infusion usually takes no more than 20 minutes.
During the procedure, you will need to apply cooling bags to the salivary glands, as Actinium-225 partially accumulates in the salivary glands, affecting their function and causing dry mouth. You will also receive intravenous saline solutions to protect your kidneys.
After the infusion of Actinium-225, you will stay in a specially equipped (radiation-shielded) ward for 48 hours. The drug is quickly excreted by the kidneys, and after 48 hours you will no longer be dangerous to others. During these 48 hours, you can read, use a mobile phone, tablet or computer – all these devices will not be a source of radiation in the future.
Follow-up examinations include whole-body scintigraphy or computed tomography in 24 hours and 48 hours after the procedure. Based on the results of the examination, the doctor will determine whether one procedure is enough for you, or whether you will need to visit the hospital again. As a rule, 1-2 procedures are required for achieving a stable positive result. Procedures are carried out with an interval of 8 weeks.
Required documents
- Medical records
- PSA blood test
- MRI/CT scan (not older than 3 months)
- Bone scintigraphy (if available)
- Biopsy results (if available)
Service
You may also book:
 BookingHealth Price from:
BookingHealth Price from:
About the department
The Department of Nuclear Medicine at the University Hospital Carl Gustav Carus Dresden offers the full range of diagnostics and treatment with therapeutic radionuclides. The department has been carrying out successful clinical activities for over 60 years, and therefore it has vast experience and outstanding achievements. The department has state-of-the-art medical equipment, thereby providing each patient with optimal medical care that meets the highest international standards. A special focus is placed on the treatment of benign and malignant thyroid diseases. The department cooperates closely with the specialized centers for breast cancer, prostate cancer, lung cancer and skin cancer. The specialists in the field of nuclear medicine also actively cooperate with doctors from the Comprehensive Cancer Center Dresden. Most diagnostic examinations are carried out on an outpatient basis, and therapeutic interventions most often take place in an 18-bed inpatient medical facility – one of the largest of this kind in Germany.
The Head Physician of the department is Prof. Dr. med. Jörg Kotzerke, who is deservedly proud of his successful clinical practice in nuclear medicine. The doctor has been working with methods of radioisotope diagnostics and treatment for more than 30 years, tirelessly demonstrating excellent results. His clinical activity is closely intertwined with his research work, reflected in more than 350 scientific publications, including in the international medical literature. Since 2007, Prof. Jörg Kotzerke has been a Board Member of the German Society of Nuclear Medicine (DGN), and as a Member of the European Association of Nuclear Medicine (EANM), he shares his knowledge and achievements with colleagues from other European countries.
A special focus is on the treatment of benign and malignant thyroid diseases. In addition, over the past two decades, the department's range of treatment has been significantly expanded. As of today, the focus of the department's doctors is on interventional radionuclide therapy for neuroendocrine tumors. Radioimmunotherapy is used for malignant lymphoma treatment.
The department has all modern devices to perform accurate diagnostics, including a gamma camera, PET-CT and PET-MRI scanners. The most common diagnostic tests include scintigraphy of the thyroid and parathyroid glands, lungs, brain, heart, and kidneys.
Radiation therapy for such thyroid diseases as thyrotoxicosis (thyroid hyperfunction) accounts for a large number of the therapeutic procedures. In addition, radiation therapy is highly effective for thyroid cancer treatment. The essence of radiation therapy is to take radioactive iodine in the form of a capsule or a special liquid, after which it is actively absorbed by the thyroid gland. The amount of radioactive iodine required for therapy is determined using an outpatient radioiodine test. The therapy is carried out on an inpatient basis only. As a rule, the hospitalization period does not exceed 3-5 days. The therapeutic effect is achieved 6-8 weeks after the procedure, and therefore the patient must be monitored by an endocrinologist and oncologist, as well as undergo follow-up examinations.
A particularly demanded therapeutic procedure is Lutetium-177 PSMA therapy in patients with metastatic prostate cancer. The isotope Lutetium-177 is injected to the patient intravenously, in the form of an infusion. Due to its specific properties, the PSMA ligand marked with Lutetium-177 targetedly binds to cancer cells and destroys them. As a rule, three procedures performed at an interval of 8 weeks are required to achieve the result. In addition to its high efficiency, Lutetium-177 PSMA therapy is well tolerated.
The department's diagnostic and therapeutic range of services includes:
| Diagnostics |
|
| Therapy |
|
| Other diagnostic and therapeutic options |
Curriculum vitae
University Education and Medical Practice
- 1977 - 1983 Study of Medicine at the Hannover Medical School.
- 1984 - 1988 Assistant Physician, Department of Nuclear Medicine and Special Biophysics, Hannover Medical School.
- 1985 Doctor of Medicine, Hannover Medical School.
- 1988 Board certification in Nuclear Medicine.
- 1989 - 1995 Senior Physician, Department of Nuclear Medicine and Special Biophysics, Hannover Medical School.
- 1991 Habilitation and Venia Legendi in Nuclear Medicine, Hannover Medical School.
- 1995 - 2002 Assistant Professor in Cardiovascular Nuclear Medicine, Department of Nuclear Medicine, Ulm University.
- 2000 - 2002 Managing Senior Physician, Department of Nuclear Medicine, University Hospital Ulm.
- Since 2002 Professor for Nuclear Medicine, Carl Gustav Carus Faculty of Medicines of the Dresden University of Technology and Medical Director of the Positron Emission Tomography Center at the Research Center Dresden-Rossendorf.
- Since 2002 Head of the Department of Nuclear Medicine at the University Hospital Carl Gustav Carus Dresden.
Main Clinical Focuses
- Diagnostics of tumors using positron emission tomography.
- Radionuclide therapy.
Memberships in Scientific Societies
- German Society of Nuclear Medicine (DGN).
- German Radiological Society (DRG).
- European Association of Nuclear Medicine (EANM).
- Society of Nuclear Medicine (SNM).
- German Cancer Society (DKG).
Photo: (с) depositphotos
Sources:
About hospital
According to the reputable Focus magazine, the University Hospital Carl Gustav Carus Dresden ranks among the top five German hospitals!
The hospital is the benchmark for modern high-quality medicine. Positioning itself as a maximum care medical facility, the hospital represents all medical fields. There are 26 specialized departments, 6 institutes and 17 interdisciplinary centers, which cooperate closely with the clinical and scientific facilities of the Faculty of Medicine. The basis of successful practice is excellent equipment, which is regularly updated, as well as highly qualified, experienced medical personnel: world famous doctors and professors work here for the benefit of patients.
In addition to its main goal of caring for patients, the hospital is also active in training and professional development of medical personnel, as well as in the field of public health care. The priority focus of the work is research activity, which allows the doctors to introduce the innovative diagnostic and therapeutic techniques into clinical practice.
A special feature of the hospital is also the diagnostics and treatment of rare diseases. State-of-the-art equipment and well-coordinated work of doctors of various medical specialties make it possible to timely recognize pathologies rarely encountered in medical practice and select the most effective therapy. Specialization in rare diseases include neurology, endocrinology, hematology/oncology, and rare autoimmune diseases.
The hospital has 1,410 beds for patient hospitalization. About 55,900 inpatients and more than 233,975 outpatients undergo treatment here annually. A large medical team, consisting of about 1,000 highly qualified doctors, as well as over 2,000 nursing staff take care of the patients' health. Each patient is guaranteed an individual approach and the most effective treatment in accordance with current clinical protocols.
It should be noted that the university hospital enjoys an impeccable reputation not only in Germany, but also far beyond its borders, including Arab countries, post-Soviet states, Great Britain and the United States. Patients from different parts of the world come here for high-quality treatment for diseases of any severity. The highest credit of patient confidence is the main indicator of the fruitful work of doctors.
Photo: (с) depositphotos
Accommodation in hospital
Patients rooms
The patients of the University Hospital Carl Gustav Carus Dresden live in comfortable rooms made in bright colors and equipped with everything necessary. The standard patient room includes an automatically adjustable bed, a bedside table with a sliding table, a wardrobe, a telephone and a TV. There is also Wi-Fi (free) in the patient rooms.
If desired, patients may live in enhanced comfort patient rooms. These patient rooms have a more sophisticated design, upholstered furniture and a safe for storing valuables.
Meals and Menus
The patients of the hospital are offered a tasty, healthy and varied three meals a day. The menu is based on local cuisine and seasonal food. If you for some reason do not eat certain products, please inform the medical staff of the hospital in advance, and you will be offered an individual menu. The nutrition provided in the hospital is certified in accordance with the quality standards of the German Nutrition Society (DGE) for catering in German hospitals.
Further details
Standard rooms include:
Religion
The religious services are available upon request.
Accompanying person
Your accompanying person may stay with you in your patient room or at the hotel of your choice during the inpatient program.
Hotel
You may stay at the hotel of your choice during the outpatient program. Our managers will support you for selecting the best option.
The hospital offers a full range of laboratory diagnostic procedures (general, hormonal, tests for tumor markers, infections, antibodies, etc.), genetic tests, various modifications of ultrasound scans, CT scans, MRI and PET / CT, angiography, myelography, biopsy and other examinations. Treatment with medications, endoscopic and robotic operations, stereotaxic interventions is carried out here, modern types of radiation therapy are also used. The hospital offers patients all the necessary therapeutic techniques.
- Cochlear implantation
- Deep brain stimulation
- Treatment of benign prostatic hyperplasia with green laser
- Da Vinci prostatectomy
- Bone marrow transplantation
These are head and neck tumors, hearloss, amyotrophic lateral sclerosis, epilepsy, Parkinson disease, infertility, malignant tumors of the reproductive system, congenital anomalies of the genital organs and the urinary system, urinary incontinence, blood clotting disorders, leukemia and other pathologies.
- Otolaryngology (Center for Cochlear Implantation)
- Neurology and Epileptology
- Urology
- Oncology
- Gastroenterology and Hepatology
About 1,000 highly qualified doctors work at the hospital.