The program includes:
- Initial presentation in the clinic
- clinical history taking
- review of medical records
- physical examination
- laboratory tests:
- complete blood count
- biochemical analysis of blood
- mineral metabolism analysis (Na, K, Ca, Mg)
- lipid metabolism (HDL/LDL, cholesterol,
triglycerides Lip(a), homocysteine) - inflammation indicators (CRP, ESR)
- indicators blood coagulation
- blood gas analysis
- chest x-ray examination
- holter monitoring (24h)
- measurement of arterial blood pressure
- electrocardiogram (ECG)
- pulmonary function test
- echocardiography
- doppler echocardiography
- high-resolution computed tomography (HR-CT)/MRI (on indication 950/1200€)
- CT angiography (on indication 1350€)
- nursing services
- consultation of related specialists
- treatment by chief physician and all leading experts
- explanation of individual treatment plan
(the cost of medicines is not included)
Required documents
- Medical records
- ECG (if available)
Service
You may also book:
 BookingHealth Price from:
BookingHealth Price from:
About the department
The Department of Cardiology at the Schlosspark Hospital Berlin provides all the possibilities of modern medicine for the conservative and interventional treatment of cardiovascular diseases. The department's team of doctors is highly professional in providing medical care to patients with coronary heart disease, heart failure, cardiac arrhythmias, valvular defects, and arterial hypertension. The medical facility has excellent technical facilities for comprehensive diagnostics, including echocardiography, electrocardiography, CT and MRI scans, and electrophysiological studies. The department also offers the services of an advanced Cardiac Catheterization Laboratory, where cardiac catheter-based tests and interventional therapeutic procedures are performed. The department annually treats more than 2,500 patients. In addition, the Chest Pain Unit admits approximately 2,500 outpatients every year. Patients with acute coronary syndrome are admitted around the clock. The Head Physician of the department is Dr. med. Richard Stern.
One of the most common pathologies in the department's clinical practice is coronary heart disease (CHD). CHD causes the formation of atherosclerotic plaques (cholesterol deposits) on the walls of the coronary vessels, resulting in a depletion of blood flow. As coronary artery disease progresses, the influx of oxygen-rich blood less and less covers the needs of the heart muscle, as a result of which the patient develops angina pectoris. If left untreated, coronary artery disease may lead to myocardial infarction or sudden cardiac death. At the diagnostic stage, a patient with suspected coronary artery disease undergoes electrocardiography, echocardiography, 24-hour Holter ECG monitoring, bicycle ergometry, and a number of laboratory tests, including a complete blood count, a biochemical blood test, an electrolyte test, and a coagulogram. If diagnostic results reveal some signs of coronary heart disease, the patient additionally undergoes coronary angiography to clarify the diagnosis. As for the treatment, at the early stages of heart pathology, the department's specialists use only drug therapy aimed at preventing complications of coronary heart disease and relieving symptoms. The second-line therapy is percutaneous transluminal coronary angioplasty with stent implantation. The interventional procedure is performed in a specially equipped Cardiac Catheterization Laboratory under local anesthesia. The essence of percutaneous transluminal coronary angioplasty is that the narrowed section of the coronary artery is expanded using a balloon attached to the catheter, which is inserted into the femoral artery through a puncture in the inguinal region. The interventional procedure is performed under X-ray guidance, which ensures accurate delivery of the catheter with an attached balloon to the area of narrowing of the coronary vessel. The final stage of the procedure is stent implantation, which prevents recurrent narrowing of the lumen of the coronary vessel, thereby ensuring normal blood supply to the myocardium.
The department also successfully performs interventional treatment for valvular heart disease. Patients with aortic valve stenosis often seek help from the department's cardiologists. The specialists at the medical facility offer transcatheter aortic valve implantation (TAVI) to treat this pathology. Aortic valve stenosis most often develops in older people with severe comorbidities for whom open surgery is contraindicated. In such cases, the TAVI procedure is the optimal treatment option. Its essence lies in the fact that the department's cardiologists replace the patient's damaged aortic valve with a prosthesis using the endovascular technique without any chest incisions and a heart-lung machine. When performing transcatheter aortic valve implantation, the department's cardiologists use a specially designed prosthesis, which is delivered to the heart through the blood vessels in a compressed form. After positioning the prosthesis in the right place, the specialists expand it to a working size, as a result of which the artificial aortic valve begins to perform those functions that the patient's own heart valve can no longer perform.
The Cardiac Catheterization Laboratory also performs clipping for mitral regurgitation. Patients with this valvular disease have a backflow of blood from the left ventricle into the left atrium when the ventricle contracts. The reason for this is the incomplete closing of the heart valve leaflets. Pathology can be congenital or acquired. Until recently, patients required open surgery to repair this valvular disease, but now a sparing interventional procedure with the MitraClip device has been implemented into practice. The department's specialists perform mitral valve clipping procedures using catheter-based techniques with an endovascular approach through the femoral vein. The image-guided intervention is performed under general anesthesia. The duration of the clipping procedure is 2-5 hours, while the correction of uncomplicated cases of mitral regurgitation takes a minimum amount of time, and in complex clinical cases, the duration of the procedure increases.
The team of the department's cardiologists has rich experience in the treatment of heart arrhythmias. Of particular interest to doctors is the implantation of pacemakers and defibrillators to normalize the heart rhythm. A pacemaker helps control abnormal heart rhythms by using electrical impulses to make the heartbeat at a normal rate. It can speed up a slow heart rate, monitor a fast heart rate, and coordinate the work of the heart chambers. The work of the defibrillator is aimed at monitoring the heart rate, so if a dangerous situation arises, it generates an electric discharge. The interventions to implant pacemakers and defibrillators are usually performed in the department under local anesthesia using a percutaneous approach. Recovery after the interventional procedure does not take much time, and the patient can leave the hospital after 1-2 days.
The department's key areas of work include the following:
- Diagnostics
- Functional diagnostics
- Resting and stress ECG
- 24-hour ECG monitoring
- 24-hour blood pressure monitoring
- Spiroergometry
- Screening for obstructive sleep apnea
- Imaging diagnostics
- Echocardiography (classical, transesophageal, and stress echocardiography with dynamic physical and pharmacological stress)
- Cardiac CT and MRI scans
- Interventional diagnostic procedures
- Coronary angiography
- Fractional blood flow reserve measurement
- Intravascular ultrasound
- Implantation of an event recorder (for determining the causes of syncope of unknown origin and for the diagnosis of atrial fibrillation)
- Functional diagnostics
- Treatment
- Drug therapy
- Catheter-based interventional treatment
- Percutaneous transluminal coronary angioplasty with stent implantation
- Transcatheter aortic valve implantation (TAVI)
- Clipping (MitraClip) for mitral regurgitation
- Revision restoration of vascular patency in chronic occlusions using ante- and retrograde recanalization
- Pacemaker implantation
- Defibrillator implantation
- Cardiac resynchronization therapy for patients with advanced chronic heart failure
- Patent foramen ovale closure
- Emergency medical care for acute coronary syndrome (around the clock)
- Other medical services
Curriculum vitae
Higher Education
- 1977 - 1984 Medical studies at the Free University of Berlin.
- 1981 - 1984 Experimental thesis at the Institute of Toxicology and Embryonic Pharmacology.
Professional Career
- 1985 - 1989 Assistant Physician, Department of Internal Medicine, Department of Radiology and Nuclear Medicine, Jewish Hospital Berlin.
- 1989 - 1996 Assistant Physician, Department of Cardiology and Pulmonology, Charite University Hospital Berlin.
- 1993 Board certification in Internal Medicine.
- 1996 Board certification in Cardiology.
- 1996 - 1997 Senior Cardiologist, Department of Internal Medicine, Martin Luther King Hospital Berlin.
- 1997 - 2005 Deputy Head and Managing Senior Physician, Department of Cardiology and Intensive Care, Vivantes Am Urban Hospital and Vivantes Hospital Friedrichshain, Berlin.
- 2005 - 2012 Medical Director of the Heart Failure Center, Jewish Hospital Berlin.
- Since 01.2013 Head Physician of the Department of Cardiology at the Schlosspark Hospital Berlin.
Additional Qualifications
- Interventional treatment of cardiovascular diseases.
- Treatment of heart arrhythmias.
Memberships in Professional Societies
- German Society of Cardiology, Working Group on Heart Failure.
- Board of Trustees of the Men's Health Foundation.
- Berlin Society for the Prevention and Rehabilitation of Cardiovascular Diseases.
- European Society of Cardiology.
Photo of the doctor: (c) Schlosspark-Klinik GmbH
About hospital
The Schlosspark Hospital Berlin began its work in 1970 and, during this time, has gained an excellent reputation not only in Germany but also in the international medical arena. The Schlosspark Hospital Berlin is an academic hospital of the Charite University Hospital Berlin, which is one of the best medical centers in Europe and throughout the world. The successful clinical practice of the medical facility is based on an advanced medical and technical base, access to the very latest and most effective treatment methods, and the exceptional competence and experience of medical personnel. The hospital is located in the picturesque Charlottenburg Park, away from the hustle and bustle of the city, which contributes to the peace of mind of patients.
The hospital's bed fund includes 340 beds. Structurally, the hospital consists of 12 specialized departments with narrowly focused centers integrated into them, which are responsible for the treatment of a particular group of diseases. More than 14,000 patients are treated annually at the hospital. One of the priorities of the medical facility is emergency medical care. With an annual number of more than 10,000 surgical interventions, including operations of high complexity, the department is particularly interested in surgical treatment.
The hospital's medical team consists of more than 900 employees. The departments at the hospital are headed by professors who are well-known in the medical community and have impressive clinical experience and outstanding professional achievements. In the course of diagnostics and treatment, an individual approach is used for each patient, and his needs and wishes are also taken into account. The hospital pays due attention to patient care during the therapeutic process. Despite state-of-the-art medical equipment and the automation of many processes, a humane and respectful attitude towards the patient is the first priority for the doctors at the hospital. The specialists are always open to dialogue and do their best to achieve the best treatment outcomes.
Photo: (с) depositphotos
Accommodation in hospital
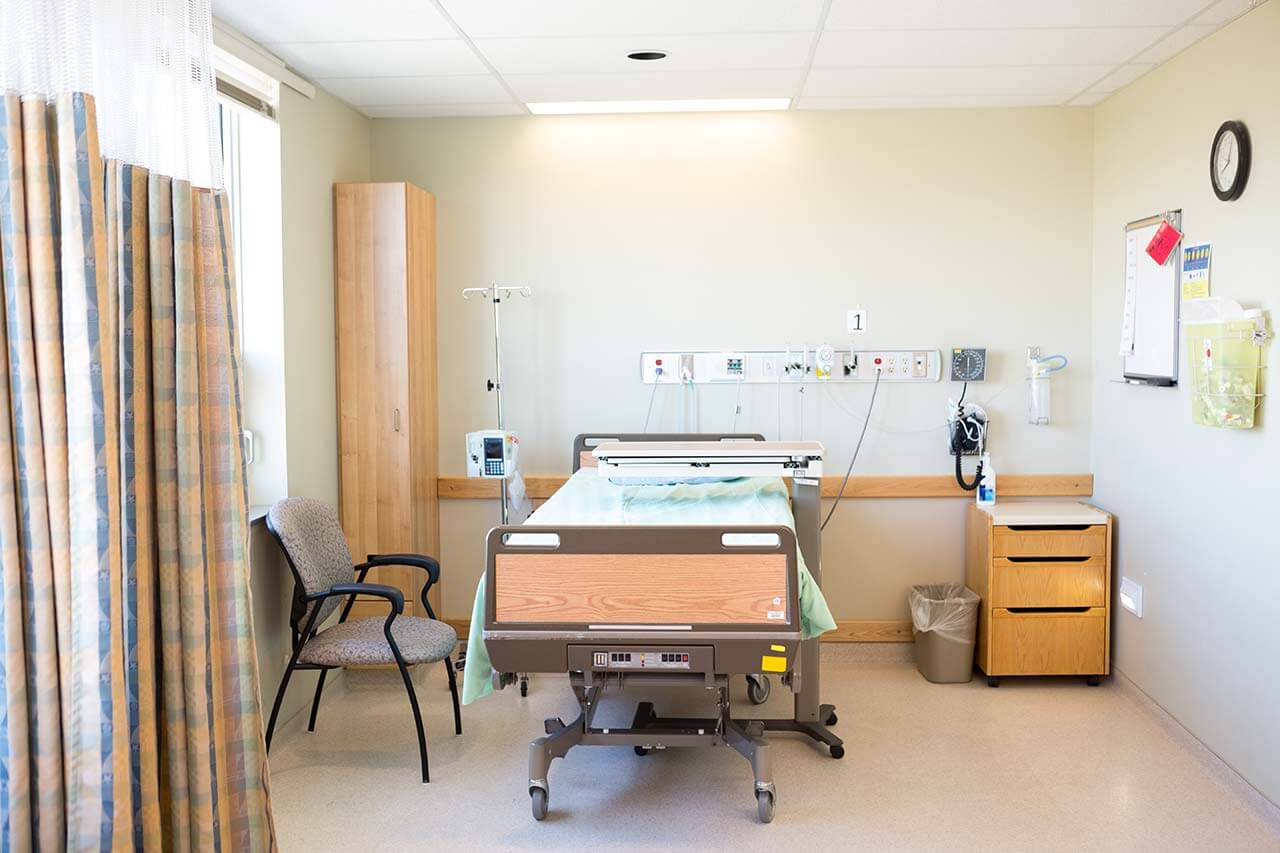
Patients rooms
The patients of the Schlosspark Hospital Berlin live in comfortable rooms with light colors. Each patient room has an ensuite bathroom with a shower and a toilet. The standard patient room includes a comfortable automatically adjustable bed, a bedside cabinet with a pull-out table, a wardrobe, a table and chairs for receiving visitors, a telephone, and a TV. Wi-Fi is available on the territory of the hospital. The hospital also offers enhanced-comfort rooms with a more exquisite design.
Meals and Menus
The patient and their accompanying person are offered three meals a day: breakfast, lunch, and dinner. A new menu is prepared for patients each week. Only high-quality and fresh products are used for cooking meals. The menu includes dietary and vegetarian dishes. The patient will be offered an individual menu if necessary.
There is a cozy cafe on the ground floor of the hospital that serves full breakfasts, a wide range of hot and cold drinks, delicious desserts, and snacks.
Further details
Standard rooms include:
Accompanying person
The accompanying person may stay with you in the patient room or at the hotel of your choice during the inpatient program.
Hotel
You may stay at the hotel of your choice during the outpatient program. Our manager will help you choose the best option.