The program includes:
- Initial presentation in the hospital
- Clinical history taking
- Review of available medical records
- Physical examination
- Laboratory tests:
- Complete blood count
- General urine analysis
- Biochemical analysis of blood
- Tumor markers
- Inflammation indicators (CRP, ESR)
- Coagulogram
- Ultrasound scan
- CT scan / MRI
- Preoperative care
- Embolization or chemoembolization, 2 procedures
- Symptomatic treatment
- Cost of essential medicines
- Nursing services
- Elaboration of further recommendations
How program is carried out
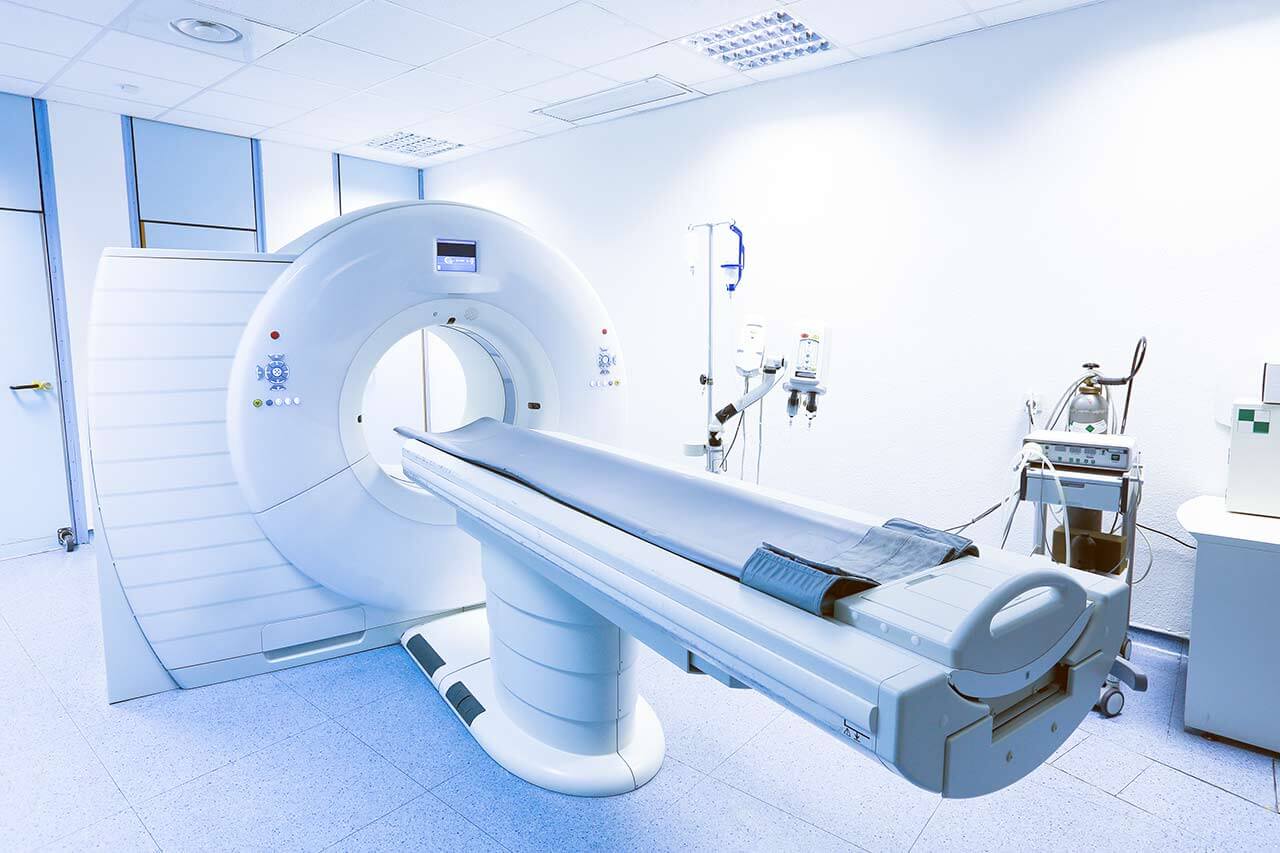
During the first visit, the doctor will conduct a clinical examination and go through the results of the available diagnostic tests. After that, you will undergo the necessary additional examination, such as the assessment of liver and kidney function, ultrasound scan, CT scan and MRI. This will allow the doctor to determine which vessels are feeding the tumor and its metastases, as well as determine how well you will tolerate the procedure.
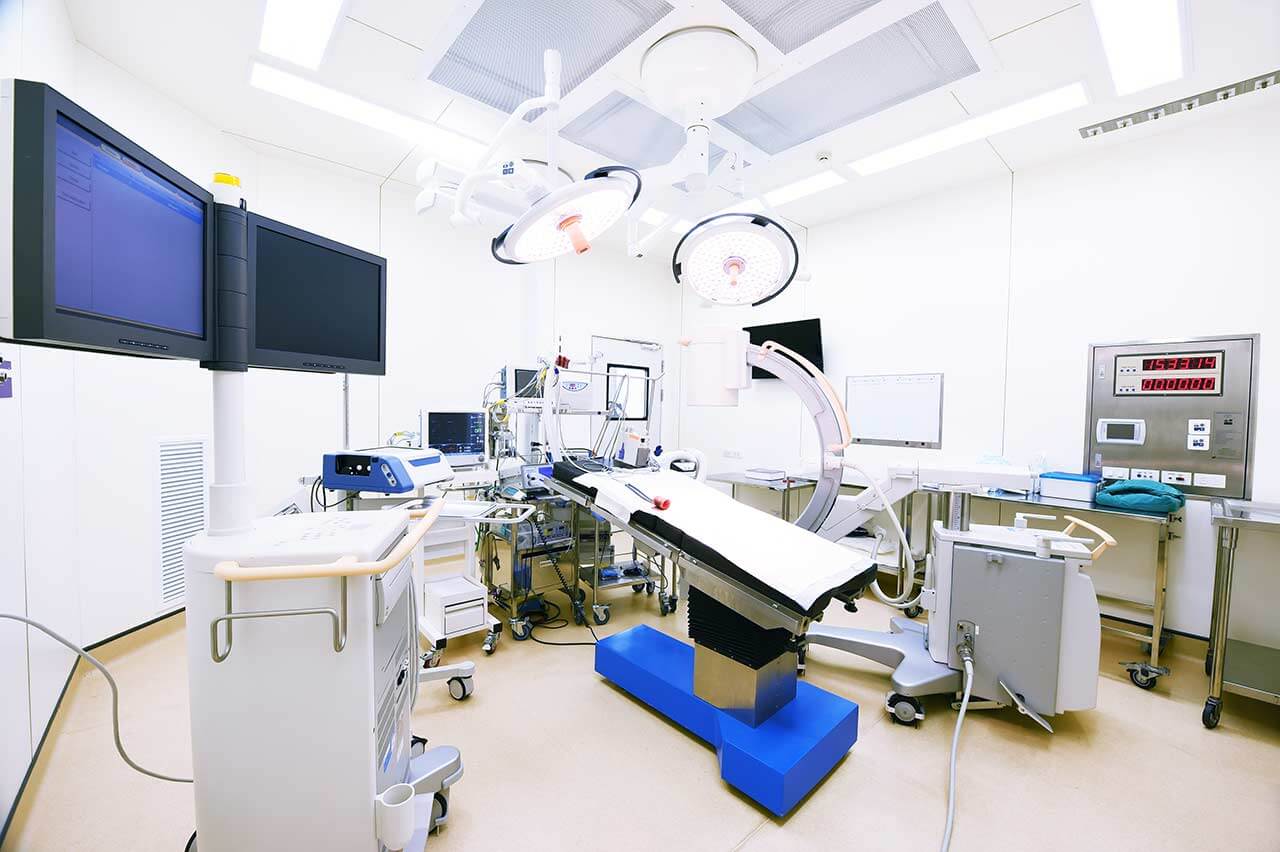
Chemoembolization begins with local anesthesia and catheterization of the femoral artery. The thin catheter is inserted through a few centimeters long incision of the blood vessel. The doctor gradually moves the catheter to the vessel feeding the primary tumor or its metastases. The procedure is carried out under visual control, an angiographic device is used for this. The vascular bed and the position of the catheter in it are displayed on the screen of the angiograph.
When the catheter reaches a suspected artery, a contrast agent is injected through it. Due to the introduction of the contrast agent, the doctor clearly sees the smallest vessels of the tumor and the surrounding healthy tissues on the screen of the angiograph. After that, he injects emboli into the tumor vessels through the same catheter.
Emboli are the spirals or the liquid microspheres. The type of embolus is selected individually, taking into account the diameter of the target vessel. When carrying out chemoembolization, a solution of a chemotherapy drug is additionally injected into the tumor vessel. Due to the subsequent closure of the vessel lumen with an embolus, the chemotherapy drug influences the tumor for a long time. In addition, the drug does not enter the systemic circulation, which allows doctors to use high doses of chemotherapeutic agents without the development of serious side effects. Chemoembolization leads to the destruction of the tumor or slowing down its progression.
After that, the catheter is removed from the artery. The doctor puts a vascular suture on the femoral artery and closes it with a sterile dressing. During chemoembolization, you will be awake. General anesthesia is not used, which significantly reduces the risks of the procedure and allows performing it on an outpatient basis, avoiding long hospital stay.
After the first procedure, you will stay under the supervision of an interventional oncologist and general practitioner. If necessary, you will receive symptomatic treatment. As a rule, a second chemoembolization procedure is performed in 3-5 days after the first one in order to consolidate the therapeutic effect. After that, you will receive recommendations for further follow-up and treatment.
Required documents
- Medical records
- MRI/CT scan (not older than 3 months)
- Biopsy results (if available)
Service
You may also book:
 BookingHealth Price from:
BookingHealth Price from:
About the department
The Department of Interventional Radiology at the University Hospital Erlangen offers the full range of services in this medical field. The department specializes in imaging diagnostics and image-guided interventional therapeutic procedures for the treatment of diseases of all organs and systems of the human body. The department has a progressive technological base, which allows conducting ultrasound examinations, digital radiography, CT scans and MRI, digital subtraction angiography and other diagnostic tests. Therapeutic interventional procedures are most often performed for vascular pathologies, cancers and other diseases. For its outstanding clinical activities, the medical facility was awarded the quality certificate of the German Society of Radiology (DRG) in the field of cardiovascular imaging diagnostics and the German Society for Interventional Radiology (DeGIR) in the field of interventional therapy. The department's specialists cooperate closely with oncologists, cardiologists, cardiac surgeons, neurosurgeons and other doctors of the university hospital. Such a multidisciplinary approach guarantees the best treatment results. The Chief Physician of the department is Prof. Dr. med. Michael Uder.
Imaging diagnostics plays a decisive role in making a diagnosis in almost all medical disciplines, and therefore the department diagnoses patients with suspected cancers, pathologies of joints, bones and soft tissues, breast diseases in women, cardiovascular diseases, and also provides the necessary diagnostic procedures for accidents and emergency clinical cases. If the confirmed diagnosis requires image-guided interventional therapy (for example, vascular obstruction or stenosis, vascular malformations, liver cancer), the patient immediately undergoes treatment. In other cases, the basic course of treatment takes place in a specialized department, under the guidance of highly specialized physicians.
Interventional therapy is performed using special catheters or stents. Its main advantage is that there is no need to make large incisions in the skin and soft tissues for access to the pathological focus. Therapeutic procedures are usually performed under x-ray or computed tomography guidance, so the doctor can clearly see everything that happens in the area of intervention on the screen or images, which guarantees high efficiency of manipulations. In addition, after this type of treatment, the patient does not experience any pain and has practically no risk of postoperative complications.
Since surgical interventions still involve the use of invasive techniques, the patient receives pain anesthesia: general anesthesia, regional anesthesia, or deep sedation. The optimal type of anesthesia is determined by the attending physician based on the patient's clinical data. Depending on the purpose of the therapeutic manipulation, a catheter, stent or balloon can be used. To advance the catheter to the pathological focus, the doctor makes a small incision in the forearm or groin, since this is where the largest vessels are located, through which it is easy enough to insert the catheter into the vascular bed. The interventional procedure can take less than half an hour or several hours – it all depends on the complexity of the pathology. As a rule, the patient leaves the hospital after 2-3 days.
The department's therapeutic offer includes various interventions for the dilation of arteries and veins in the upper and lower extremities, neck, thorax and abdominal cavity, as well as procedures for the elimination of blood clots, correction of thoracic and abdominal aortic aneurysms, embolization procedures for closing the vessels supplying benign and malignant tumors, chemoembolization procedures with local administration of a chemotherapy drug and other procedures. The department's specialists often resort to image-guided surgical interventions to stop internal bleeding.
The department's range of medical services includes:
- Diagnostic services
- Diagnostics of otolaryngological diseases (ENT diseases)
- Computed tomography (CT), also with contrast enhancement
- Magnetic resonance imaging (MRI), also with contrast enhancement
- Ultrasound examinations (most often used to diagnose pathologies in the neck)
- DIagnostics of the respiratory system
- Conventional X-ray examinations
- Computed tomography (CT), also with contrast enhancement
- Magnetic resonance imaging (MRI), also with contrast enhancement
- Ultrasound examinations
- Diagnostics of heart disease
- Ultrasound examination of the heart (echocardiography)
- Cardiac MRI
- Cardiac CT scans
- Diagnostics of vascular diseases
- Angiography (imaging method for interventional vascular examination)
- Ultrasound examinations
- Contrast-enhanced CT scans
- Contrast-enhanced MRI
- Diagnostics of abdominal and gastrointestinal pathologies
- Ultrasound examinations (also in combination with conventional X-ray examinations)
- Computed tomography (also for cancer staging and detecting metastases)
- Magnetic resonance imaging
- Virtual colonoscopy
- Diagnostics of kidney and urinary tract pathologies
- Ultrasound examinations
- CT scans
- MRI
- Diagnostics of pathologies of the reproductive system in men and women
- Ultrasound examinations
- CT scans
- MRI
- MRI-guided biopsy (for example, for suspected prostate cancer)
- Diagnostics of musculoskeletal pathologies
- Conventional X-ray
- Ultrasound examinations
- CT scans
- MRI
- Diagnostics of breast pathologies
- Mammography for breast cancer detection
- Breast ultrasound (including elastography)
- MRI and MRI-guided biopsy (vacuum biopsy, fine needle aspiration biopsy)
- Galactography (imaging of the milk ducts of the breast using the X-ray system)
- Tomosynthesis
- Diagnostics of otolaryngological diseases (ENT diseases)
- Therapeutic services
- Drainage placement
- Vena cava filter implantation
- Radiofrequency ablation
- Balloon angioplasty
- Stent implantation
- Embolization
- Thrombolytic therapy
- Transarterial chemoembolization (TACE)
- Correction of vascular malformations
- Renal denervation
- Image-guided interventions for internal bleeding
- Other diagnostic and therapeutic methods
Curriculum vitae
Prof. Dr. med. Michael Uder studied Human Medicine at the Saarland University in Homburg, where he also underwent board certification in Radiology. In 2002, the doctor defended his doctoral dissertation on the side effects of radiopaque drugs on the kidneys. From 2003 to 2009, he served as a Professor in the Department of Interventional Radiology at the University Hospital Erlangen. In 2009, the Professor took the post of the Head of this department.
Dr. Uder is also the first Chairman of the Bavarian Radiological Society and the Chairman of the Academy for Advanced Training in Radiology. The doctor also chairs the Working Group of the German Radiological Society (sponsored by the Professional Association of German Radiologists).
Photo of the doctor: (c) Universitätsklinikum Erlangen
About hospital
According to the Focus magazine, University Hospital Erlangen ranks among the best medical facilities in Germany!
The hospital is one of the leading healthcare facilities in Bavaria and offers top-class medical care distinguished by the close intertwining of clinical activities with research and training of medical students. The hospital was founded in 1815 and today is proud of its rich traditions, numerous medical achievements and an excellent reputation not only in Germany, but also in the international arena. The hospital has 25 specialized departments, 7 institutes and 41 interdisciplinary centers, whose experts work tirelessly for the benefit of their patients.
The hospital has the status of a maximum care center, and therefore it represents almost all fields of modern medicine. Oncology, transplant medicine, and robot-assisted surgery are among the top priorities of the clinical activities of the medical complex. Oncology is represented by the Comprehensive Cancer Center Erlangen, which is one of 13 centers of excellence in Germany certified by the German Cancer Society. The university hospital has a high-tech center with high success rates for heart, liver, kidney, pancreas, cornea and bone marrow transplants. In addition, the hospital is a leader in the use of robot-assisted surgery. The medical facility has at its disposal innovative robotic technologies, in particular the da Vinci Surgical System, with the help of which surgeons perform many sparing interventions in various medical fields.
The medical team of the hospital consists of highly professional therapists, surgeons and nursing staff. The focus of their efforts is on the patient, his health and peace of mind, as well as comfort during treatment. The clinical practice of doctors is based on an individual approach to each case, which results in high treatment success rates. State-of-the-art technical equipment also plays an important role in the therapeutic process. The hospital is proud of the most advanced devices for imaging diagnostics (X-ray, ultrasound, CT, MRI, PET-CT, SPECT-CT, etc.), endoscopic examinations, laboratory tests, as well as specially equipped operating rooms for robot-assisted interventions, image-guided therapeutic manipulations, minimally invasive and classical surgeries of any complexity. Thus, the doctors of the university hospital have all the necessary resources to effectively treat the most severe pathologies and save lives.
The combination of high-tech equipment, experienced and highly qualified personnel, as well as strict adherence to the standards of modern medicine, form a solid foundation for the provision of the best medical care at the European level. An undeniable proof of the high prestige of the hospital is the constantly growing number of patients who come here from various regions of Germany and other countries of the world.
Photo: (с) depositphotos
Accommodation in hospital
Patients rooms
The patients of the University Hospital Erlangen live in comfortable rooms with light colors and modern design. Each patient room has an ensuite bathroom with shower and toilet. The furnishing of the patient room includes an automatically adjustable bed with an orthopedic mattress, a bedside table, a wardrobe, a table and chairs for receiving visitors, a TV, a radio and a telephone. Wi-Fi can be provided upon request. The use of a mobile phone is prohibited in many rooms of the hospital.
Patients can also live in enhanced-comfort rooms with a more sophisticated design. The enhanced-comfort rooms additionally include upholstered furniture, a minifridge and a safe.
Meals and Menus
The hospital offers healthy and tasty food distinguished by many awards, including the 1st place in the prestigious ESSEN PRO GESUNDHEIT competition of the Bavarian State Ministry of the Environment and Consumer Protection.
The patient and the accompanying person have three meals a day. Breakfast is served buffet style: scrambled eggs, boiled eggs, sausage, cheese, bread and buns with butter and jam, cereals, etc. There are three set menus for lunch and dinner to choose from: a classic menu featuring local cuisine dishes, a Mediterranean menu and a vegetarian menu.
If for some reason you do not eat all the foods, you will be offered an individual menu. Please inform the medical staff about your dietary preferences prior to the treatment.
The hospital also houses many cafeterias, which will delight with a wide range of delicious dishes and drinks.
Further details
Standard rooms include:
Religion
The hospital regularly hosts catholic and evangelical devine services. The services of representatives of other religions are available upon request.
Accompanying person
During an inpatient program, an accompanying person can stay with you in the patient room or in a hotel of your choice.
Hotel
During an outpatient program, you can stay in a hotel of your choice. The managers will help you choose the most suitable options.