The program includes:
- Initial presentation in the clinic
- clinical history taking
- review of medical records
- physical examination
- laboratory tests:
- complete blood count
- general urine analysis
- biochemical analysis of blood
- TSH-basal, fT3, fT4
- tumor markers
- inflammation indicators
- indicators blood coagulation
- ultrasound
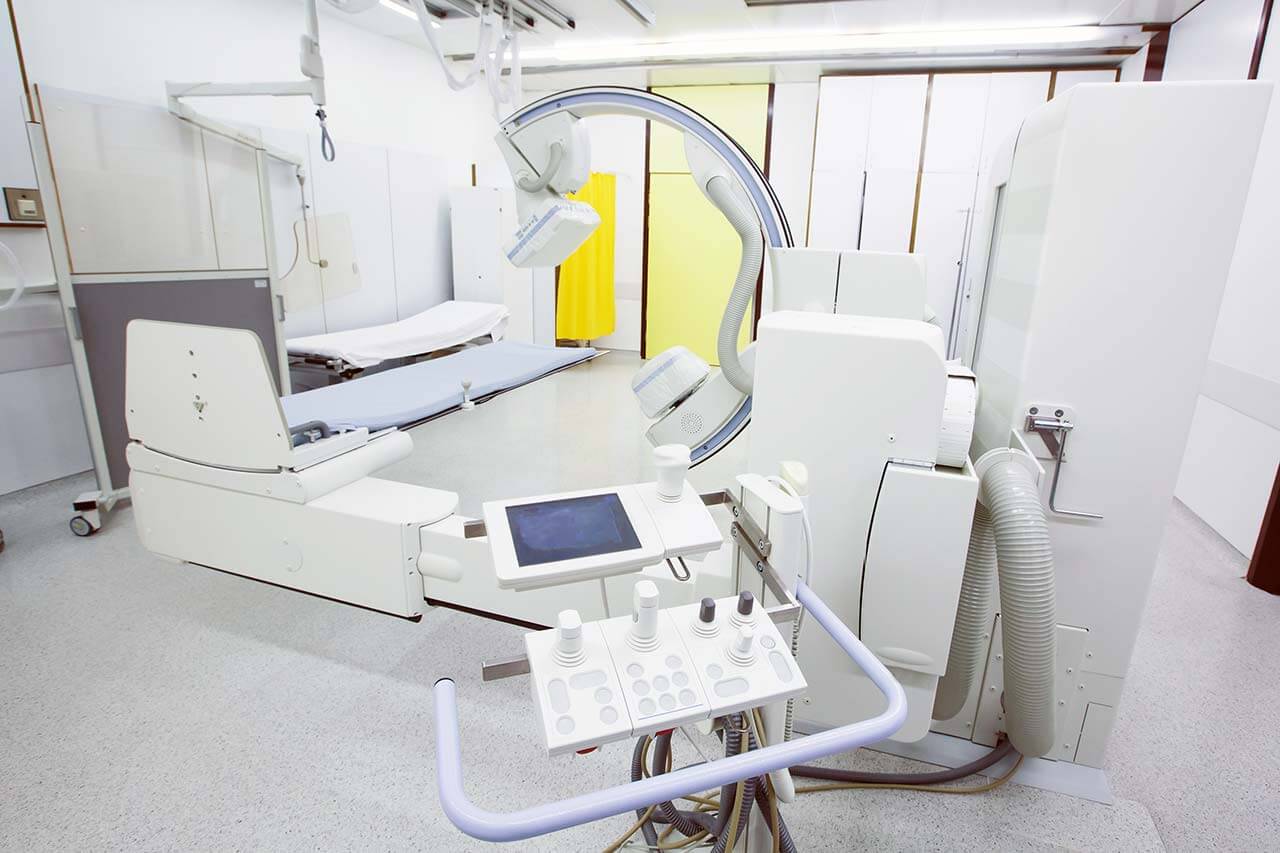
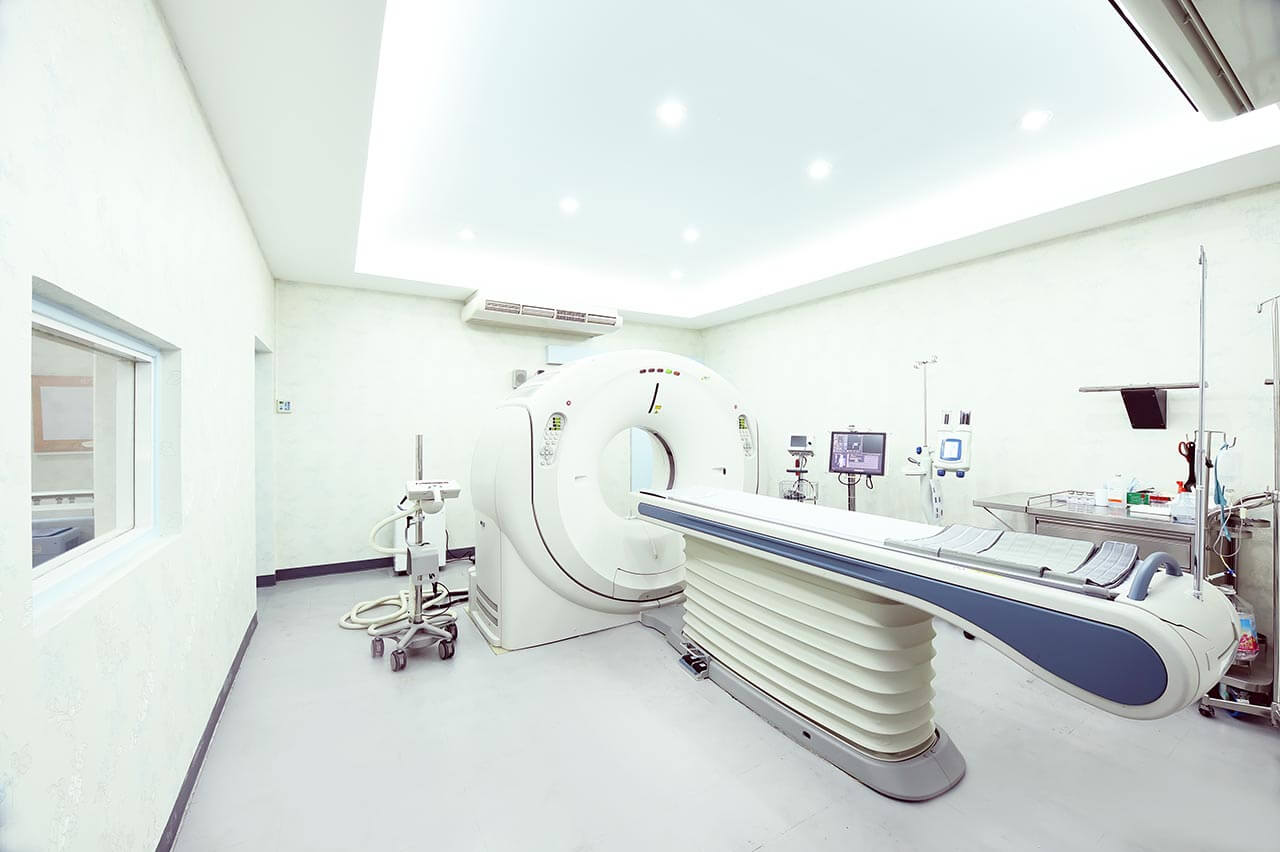
- CT/MRI scan
- proton therapy
- nursing services
- consultation of related specialists
- treatment via head doctor and all leading experts
- explanation of individual treatment plan
How program is carried out
Proton therapy is the outpatient procedure, you do not need to stay in the hospital all the time.
During the first visit, the physician will conduct a clinical examination, go through the available medical records and CT scans. If necessary, the physician will prescribe you additional examinations in order to clarify the diagnosis and determine the localization of the tumor more accurately.
Preparation for proton therapy begins with manufacturing the special device – the individual immobilizer that will fix the position of your body during a proton therapy session. Immobility is essential for high irradiation accuracy.
After the control computed tomography, during which you will stay in the immobilizer, the healthcare professionals will develop an individual treatment scheme. The treatment scheme determines the number of proton therapy sessions, the radiation dose, the angle of the rays and the depth of their penetration. In accordance with these, technical devices are manufactured that determine the depth and form of irradiation. These are the collimator (determines the shape of the proton beam) and the bolus (determines the depth of the proton beam penetration).
After that, a trial irradiation session is carried out using the individual immobilizer, collimator and bolus. Doctors evaluate the radiation dose received by the tumor and its compliance with the treatment scheme.
Proton therapy. The procedures are carried out once a day, 5 days a week. Usually Saturday and Sunday are your free days when you do not need to visit the hospital.
Before each procedure, specialists check the position of your body using X-ray in two projections. If necessary, the irradiation is synchronized with the respiratory movements. After that, the tumor is exposed to the proton beams for 1-3 minutes. The total duration of the session with all the checking procedures is 15-30 minutes.
The procedure is painless and is performed in open-type devices (this is important for overweight people or people with claustrophobia). Proton therapy does not require bed rest or other restrictions of physical activity.
Monitoring the treatment effectiveness. After completing the treatment, you will be advised to come in for the long-term follow-up. You will visit your doctor regularly for a clinical examination and, if necessary, a CT scan.
Required documents
- Medical records
- MRI/CT scan (not older than 3 months)
- Biopsy results (if available)
Service
You may also book:
 BookingHealth Price from:
BookingHealth Price from:
About the department
The Department of Adult and Pediatric Proton Therapy at the University Hospital Essen offers the full range of proton treatment and it is one of the leading and most progressive medical facilities of this kind not only in Germany, but throughout the world. The proton therapy is mostly used for the treatment of tumors of the eye, brain, spine and pelvic organs. Also, the proton therapy is an excellent treatment of tumors in children, since it has a minimal negative effect on the immature, sensitive tissues of the child’s body. The department is headed by Prof. Dr. med. Beate Timmermann.
The proton therapy is a modern and accurate type of radiation therapy for the treatment of cancer, which is considered particularly sparing and effective due to its physical properties. The standard indications for proton therapy include chordomas and chondrosarcomas of the skull base and axial skeleton, tumors of the ocular fundus and solid tumors in children.
The department is equipped with four therapeutic rooms with different proton modalities and the possibility of image guidance using X-ray, CT and MRI. The most important attention is paid to proton therapy in children (even under the age of 5 years). Also, since January 2015, the department offers a comprehensive irradiation of the central nervous system (craniospinal proton therapy). The advantages of proton therapy include its highest possible accuracy, scientifically proven efficacy and good tolerability (usually patients can immediately return to everyday life and do not experience serious side effects).
The department specializes in proton therapy in the following oncological diseases:
- Oncopathology in adult patients
- Stage I or II gliomas
- Glioblastomas
- Meningiomas
- Craniopharyngiomas
- Ependymomas, medulloblastomas, germinomas (also, the treatment of craniospinal neoplasms)
- Chordomas/chondrosarcomas of the skull base, spine and pelvic organs
- Glomus tumors
- Bone and soft tissue sarcomas of the skull base, spine and pelvic organs
- Nasopharyngeal cancer
- Cancer of the paranasal sinuses
- Progressive tumors of the pelvic organs, accompanied by lymph efflux disorders
- Salivary gland cancer
- Adenoid cystic carcinomas
- Prostate cancer (intermediate and high-risk stages)
- Complicated recurrent cancer cases
- Oncopathology in children (including children under 5 years old)
- Tumors of the central nervous system
- Parameningeal/craniofacial tumors
- Spinal tumors
- Pelvic tumors
- Other oncological diseases in adults and children
Curriculum vitae
Professional Activities
- 1993 Doctoral Degree, Faculty of Medicine, University of Hamburg, Germany.
- 2000 PhD thesis defense, Faculty of Medicine, University of Tuebingen (Supervisor: Prof. M. Bamberg).
- 2002 Medical Specialist in Radiotherapy and Radiation Oncology.
- 2002 - 2005 Head of the Center for Pediatric Proton Radiation Therapy Program (ZPT), Paul Scherrer Institute, Villigen, Switzerland.
- 2005 - 2009 Deputy Medical Director of the Center for Pediatric Proton Radiation Therapy Program (ZPT), Paul Scherrer Institute, Switzerland.
- 2007 Habilitation in Radiation Oncology, Faculty of Medicine, University of Muenster (Supervisor: Prof. Dr. N. Willich).
- 2009 - 2011 Deputy Medical Director of the West German Proton Therapy Centre Essen (WPE).
- 2011 - 2013 Medical Director of the West German Proton Therapy Centre Essen (WPE).
- 2012 Invitation to the Department of Radiation Therapy (focus on proton therapy) at the University of Duisburg-Essen.
- 2013 Appointment as the Medical Director of the West German Proton Therapy Centre Essen (WPE).
- 2014 Appointment to the position of the Head of the Department of Proton Therapy at the University Hospital Essen.
Clinical Focuses
- Sarcomas in childhood and adulthood.
- Chordomas and chondrosarcomas in childhood and adulthood.
- Brain tumors in childhood and adulthood.
- Theoretical and practical application of proton therapy.
- Clinical quality provision in radiation therapy.
- Craniospinal axis radiation therapy.
- Development of guidelines for the treatment of tumors in childhood and adolescence.
- Interdisciplinary researches.
Research Focuses
- Examination of brain tumors and sarcomas.
- Multimodal therapy in children with oncopathology.
- Detection of late effects and quality of life after radiation and proton therapy.
- Intensity-modulated proton therapy.
Memberships in Professional Societies
- German Society for Radiotherapy and Oncology (DEGRO).
- German Society of Pediatric Oncology and Hematology (GPOH).
- Working Group on Pediatric Radiation Oncology (APRO).
- European Society for Radiotherapy and Oncology (ESTRO).
- Scientific Association of Swiss Radiation Oncology (SASRO).
- Proton Therapy Cooperative Group (PTCOG).
- German Cancer Society (DKG).
- International Society of Pediatric Oncology (SIOP).
- Cancer Society of North Rhine-Westphalia.
- Certification Commission of the German Society of Pediatric Oncology.
- Primo Medico Network expert postal.
- Leading Medicine Guide expert portal.
Photo of the doctor: (c) Universitätsklinikum Essen
About hospital
According to the authoritative Focus magazine the University Hospital Essen ranks among the top German hospitals!
With 27 specialized departments and 24 institutes, the hospital in Germany is a maximum care medical facility. The hospital has 1,300 beds for inpatient treatment. A highly qualified medical team of more than 6,000 employees takes care of the health of patients. All the specialists give preference to an interdisciplinary medical care, which guarantees a comprehensive treatment taking into account the smallest aspects of a particular pathology. The hospital annually diagnoses and treats more than 50,000 inpatients and about 195,000 outpatients, which testifies to the prestige of the medical institution and the highest quality of treatment in Germany.
The hospital presents all the modern medical fields. Nevertheless, special attention should be given to the following major fields of specialization as oncology, transplantology and cardiology, as well as research activities in the field of immunology, infectology and translational examinations of pathologies of the nervous system and behavioral disorders.
Established on the basis of the standard American model of Comprehensive Cancer Centers, the West German Cancer Center (WTZ) in Essen was recognized as the best medical facility of this kind in Germany in 2009. Nowadays, the center holds leading positions both on the national and international medical markets. The basis of its successful clinical practice is the use of very latest treatment methods and an interdisciplinary approach to each clinical case. The West German Organ Transplant Centre (WZO) is also recognized as one of the best in the country and one of the few in Germany, which specializes in the transplantation of all vital organs, such as kidney, liver, pancreas, heart and lungs. Special attention is paid to kidney and liver transplantation.
The hospital in Germany is proud of its high-tech medical equipment, experienced and competent staff, productive research activities, which allow to guarantee the accurate diagnostics and effective treatment, including rare and very complex clinical cases for every patient. Consequently, the hospital is considered a perfect embodiment of high-quality treatment in Germany.
Photo: (c) depositphotos
Accommodation in hospital
Patients rooms
The patients of the University Hospital Essen live in comfortable rooms designed in bright colors. The standard room furnishing includes an automatically adjustable bed, a bedside table, a personal wardrobe, a personal call button with a built-in light panel, a telephone, a TV and a radio. The Internet access is available at an additional cost.
Meals and Menus
The patients of the hospital are offered a daily choice of three menus. The patients are also offered alternative types of menus, if their religion requires the exclusion of certain foods. If you follow a certain diet or suffer from food intolerance, you will be provided with a menu of your choice by discussing it with your attending physician in advance. The hospital also houses a bistro and a cafe, where one can have a tasty snack, enjoy hot and cold drinks.
Further details
Standard rooms include:
Accompanying person
There are a few types of hotels for the accompanying persons, who want to stay near the hospital. The hotel of the Essen University Hospital offers apartments on the first floor of the nursing high-rise building. The DRK nursing also offers single and double rooms.
The hotel in Grugapark is available for the parents, whose children stay in the hospital. The parents of children with cancer can also stay here. Moreover, The Department of Pediatrics offers its rooms for parents.