Breast cancer immunotherapy (IT) represents a groundbreaking advancement in oncology, encompassing various innovative approaches to breast cancer treatment. Breast cancer (BC, BCa) is one of the most common malignant tumors globally [1], but here's the thing – it's been considered an immunologically "cold" tumor with way less T-cell infiltration and lower mutational load compared to other "hot" solid tumors like non-small cell lung cancer and melanoma. This made it harder to treat with affecting the immune system drugs for a long time.
The most immune response-stimulating subtype in the breast cancer statistics now is triple negative breast cancer (TNBC) [2]. It demonstrates high PD-L1 expression, lots of tumor-infiltrating lymphocytes (TIL), genomic instability and high mutation rates. These are pretty good numbers – in the KEYNOTE-522 study, adding boosting the immune system medications to chemotherapy raised complete response rates, improved overall survival, and event-free survival [3]. The German specialists gained real experience with hard cases – recurring, metastatic, and triple-negative breast cancers (TNBC). With customized protocols and individually-made vaccines, they basically mobilize the body’s immune system against cancer cells to improve survival and quality of life for breast cancer patients.
When Is Immunotherapy Administered for Breast Cancer?
The main tasks of immunotherapy treatment for early and metastatic triple negative breast cancer are as follows:
- Stop or slow down the growth of the primary tumor and its metastatic cancer cells
- For unresectable triple negative breast cancer – prevent metastatic breast cancer
- For resectable triple negative breast cancer – prevent recurrence after surgery
- Increase the effectiveness of other triple negative breast cancer treatments (e.g., chemotherapy, radiation therapy)
In the early cancer stages, with large resectable tumors, the doctor may prescribe immunotherapy (IT) before surgery, in combination with chemotherapy. This helps to reduce the size of the tumor and make the operation easier: for example, to resect the breast instead of removing it completely. After the operation, immunotherapy is continued without chemotherapy; now, it is aimed at relapse prevention via enhancing the body’s immune system and suppressing the remaining sporadic cancer cells.
If doctors do not perform surgery to remove a breast tumor, then immunotherapy is used to control triple negative breast cancer. It inhibits the further tumor growth and progression of metastatic breast cancer throughout the body. This option is used in the advanced triple negative breast cancer stages, with active metastasizing, or if the woman refuses to treat breast cancer (BC) surgically for any reason. In the advanced stages of cancer, immunotherapy (IT) is combined with chemotherapy, hormone therapy, and radiation therapy. This is possible due to its excellent tolerability and the absence of severe side effects after the body’s immune system activation.
What Are the Types of Immunotherapy for Breast Cancer?
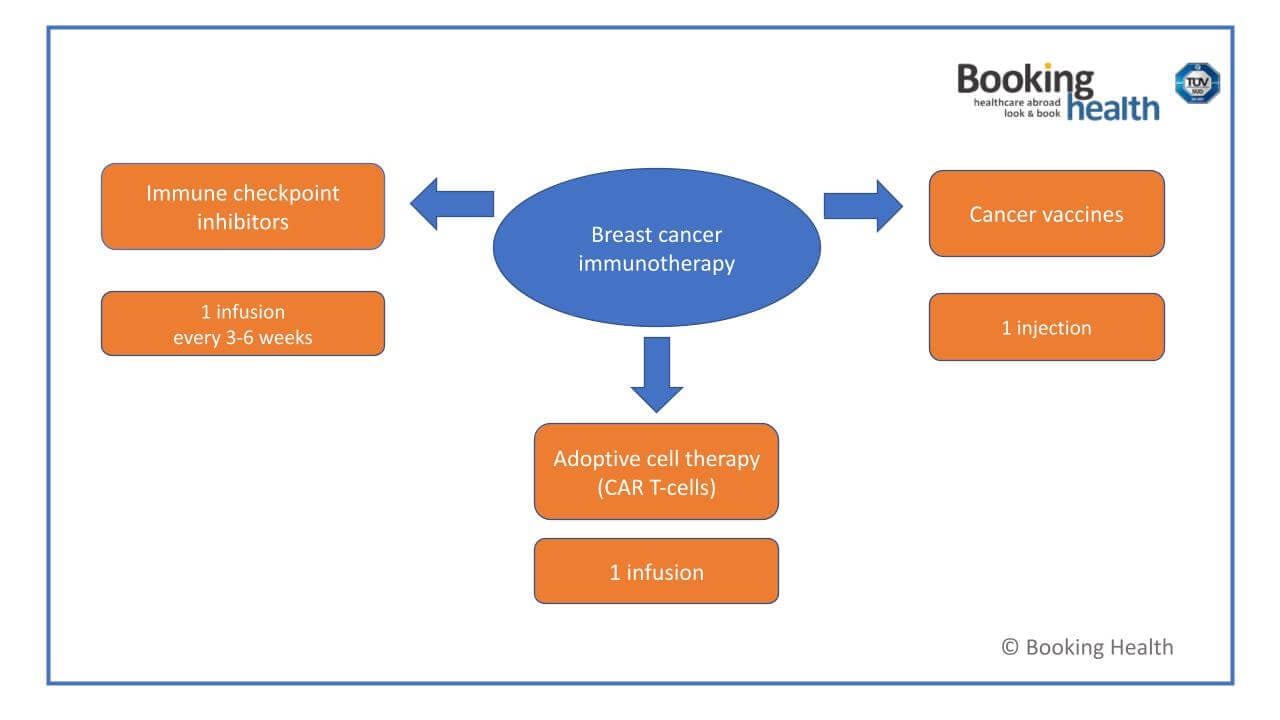
Immunotherapy combines drugs that destroy cancer cells by acting on different parts of the immune system. Sometimes these are factory-made immune response-modifying drugs; sometimes, these are drugs that are manufactured individually, using the patient's immune cells. In German hospitals, doctors use three main groups of immune system affecting drugs (some for triple negative breast cancer and some for hormone receptor positive breast cancer (HR+, HER2+), including metastatic breast cancer (mBC)), these are:
- Immune checkpoint inhibitors (PD-1/PD-L1 inhibitors, CTLA-4 inhibitors) [4]
- Cancer vaccines, e.g. dendritic cell vaccines [5]
- Adoptive immune cell therapy, i.e. CAR T-cell therapy
Immune checkpoint inhibitors (ICI) are drugs for targeted treatment that disrupt cancer cells’ ability to hide from the attacks of the immune system. Normally, a woman's immune system recognizes and destroys the very first cancer cells in the mammary gland, preventing tumor development. Unfortunately, a tumor can hide signs of malignancy and resemble healthy tissue. This is recognized and removed by immune checkpoint inhibitors (ICI). The pharmacological group includes drugs against various tumor molecules: PD-1 or PD-L1 inhibitors and CTLA-4 inhibitors (ICB). Before starting to treat breast cancer (BCa) with immune response-modifying drugs, doctors determine the initial level of PD-1 in tumor cells: to achieve a good result, and it must be high.
Dendritic cell vaccines stimulate natural specific immunity, a targeted immune response. This is a strictly individual type of hormone receptor positive and triple negative breast cancer treatment; doctors use tumor components and the patient's leukocytes to make a vaccine. In laboratory conditions, leukocytes "get acquainted" with the surface antigens (NeoAg) of a breast tumor. Such leukocytes, T-cells, are called dendritic cells, and after being infused into the blood, they become able to find the tumor and metastases. Dendritic cells help all the other immunocompetent cells detect a tumor: some of such cells directly destroy malignant foci, and others form a long-term immune response and immunological memory in order to prevent a relapse. The immune system's response is transformative – once activated, it develops and maintains a lifelong memory against the specific cancer cells.
Adoptive cell therapy (ACT) is a technologically more complex type of changing a patient's T-cells, leukocytes. After such a modification, T-cells can successfully find and attack hormone receptor positive and triple negative breast cancer foci, regardless of their localization. CAR T-cell therapy involves the genetic modification of white blood cells: a special receptor is added to them and makes them able to bind to breast cancer cells. Information about the new receptor is fixed in the genome so that it is reproduced in new generations of leukocytes to fight metastatic breast cancer (mBC) longer.
Nanotechnology is also being used to fight early breast cancer and metastatic breast cancer. Nanoparticles deliver imaging compounds (at the diagnostic stage), phototherapy compounds, or drugs (at the treatment stage) to breast cancer cells.
What to Expect During Breast Cancer Immunotherapy Treatment in Germany
Immune checkpoint inhibitors (PD-1/PD-L1 inhibitors, CTLA-4 inhibitors) are given by injections. They are dripped through a vein in an outpatient facility under medical supervision. The drug is administered intravenously once every 3-6 weeks, depending on the general therapeutic regimen. Immune checkpoint inhibitors are well tolerated and have only occasional minor side effects (e.g., fatigue, loss of appetite, nausea, diarrhea). It is a suitable option for immunotherapy for breast cancer, including metastatic triple-negative breast cancer (mTNBC).
Dendritic cell therapy represents a sophisticated yet remarkably straightforward personalized immune system-stimulating treatment approach that has been made possible by Ralph Steinman, who was awarded the 2011 Nobel Prize in Medicine for his discovery of dendritic cells.
The entire process consists of just two outpatient visits with minimal disruption to daily life. During the first visit, specialists conduct:
- Comprehensive clinical examination
- Essential laboratory testing
- Blood collection for cancer vaccine manufacturing
- Individual treatment planning to receive the best possible immune response
After just seven days, during which the personalized dendritic cell vaccine is created, patients return for a single day of treatment that includes the cancer vaccine injection and any necessary supportive care. This efficient, patient-friendly approach makes it particularly attractive for those seeking effective treatment with minimal hospital time.
To provide deeper insight into cancer vaccines, we spoke with Professor Frank Gansauge, a leading expert in dendritic cell therapy with over 22 years of experience. As the head of LDG Laboratories, which has successfully performed more than 2,500 dendritic cell procedures, Prof. Gansauge explains the innovative nature of this immune system-stimulating treatment and its remarkable effectiveness for early and metastatic breast cancer (mBC). His clinic's approach aims not only to kill cancer cells but also to maintain patients' quality of life throughout the therapy process.
Immunotherapy Expert Prof. Frank Gansauge: "Revolutionizing Cancer Treatment with Dendritic Cell Therapy"
Adoptive cell therapy (CAR T-cell therapy) requires inpatient treatment. Hospital admission is obligatory, as patients receive high-dose chemotherapy before the infusion of modified CAR T-cells. Chemotherapy temporarily reduces the level of a woman's leukocytes, so the injected modified CAR T-cells multiply more actively and provide stable anti-cancer immune system response faster. The laboratory stage of CAR T-cells creation can take up to 3 weeks, so the patient visits the clinic twice: for blood donation and directly for treatment boosting the immune system.
| Characteristic | Checkpoint Inhibitors | Dendritic Cell Vaccines | CAR T-Cell Therapy |
|---|---|---|---|
| Treatment approach | Factory-made drugs (PD-1/PD-L1, CTLA-4 inhibitors) | Personalized vaccine using patient's immune cells | Genetically modified patient's immune cells |
| Treatment setting | Outpatient | Outpatient | Inpatient (hospital admission required) |
| Number of visits | Multiple (every 3-6 weeks) | Two visits total | Two visits (blood donation + treatment) |
| Treatment duration | Ongoing course (3-6 weeks between doses) | Single procedure after 7-day cancer vaccine creation | Single intervention after 3-week cell modification |
| Preparation needed | PD-L1 testing (must be high) | Blood collection for cancer vaccine | High-dose chemotherapy before infusion |
| Side effects | Occasional minor: fatigue, appetite loss, nausea, diarrhea | Very mild, allows normal daily activities | Related to preparatory chemotherapy |
| Best suited for | PD-L1+ tumors, combination with chemo | Early-stage breast cancer, locally advanced breast cancer, stage 4 exhausted patients, personalized approach to immune cells training | Advanced breast cancer cases needing intensive intervention |
| Response rate | Up to 45% | Up to 90% | Up to 40% |
| Cost (EUR) | 375,000-420,000 (full course) | 20,000-38,000 | 450,000-550,000 |
| Key advantage | Proven in clinical trials, standard option for immune system activation | Best tolerability, lifelong immune response, highest response rate | Ability to destroy cancer cells regardless of location |
| Treatment principle | Blocks tumor's ability to hide from immune system | Trains immune system to recognize breast cancer cells | Adds special receptors to find and attack cancer cells |
Note: All costs and survival rates are based on Booking Health data and vary depending on cancer type, stage, patient condition, and their immune response.
Benefits, Expected Results and Survival Rates with Immunotherapy for Breast Cancer
In patients with breast cancer (BCa), immunotherapy has such benefits:
- Has proven efficacy in stages II-IV of cancer
- Can be used at stage I in eligible women
- Successfully treats the most aggressive forms of breast cancer
- Reduces the risk of breast cancer recurrence after surgery
- Shrinks the tumor before surgery, allowing it to be resectable
- Affects not only the primary tumor but also breast cancer cells in metastases, even undetected ones
- Effective in metastatic triple negative breast cancers (mTNBC) where many other techniques have failed
Drugs affecting the immune system are easy to use. Unlike chemotherapy, they do not have to be given in long courses, spending weeks in hospital. Most breast cancer immunotherapy medications are given once every 3 to 6 weeks. In the case of dendritic cell therapy, a single procedure is sufficient for the induction of durable anticancer immunity.
Cost of Immunotherapy for Breast Cancer in Germany
| Treatment | 2-Year Survival Rate* | Response Rate** | Cost of treatment, € *** |
|---|---|---|---|
| Dendritic cell therapy | up to 85% | up to 90% | 20,000 – 38,000 |
| Checkpoint inhibitors | up to 45% | up to 45% | 375,000 – 420,000 for the full course |
| CAR T-cell therapy | up to 50% | up to 40% | 450,000 – 550,000 |
*Booking Health data. Survival rates vary widely depending on the type of cancer, the patient's condition, and specific circumstances.
**Booking Health data. Response rate is the number of patients who show improvement after treatment.
***The cost of treatment depends on the type of tumor, stage of cancer, and other factors.
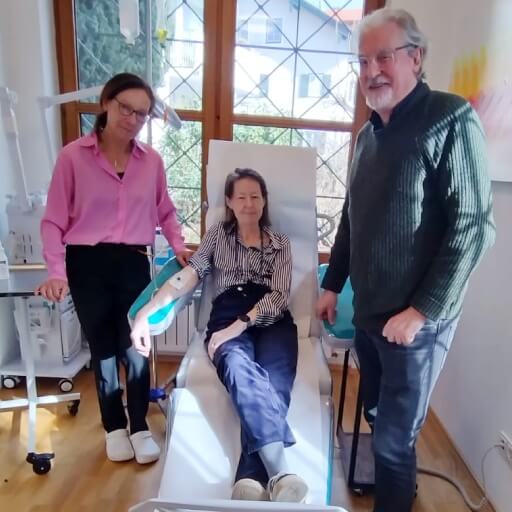
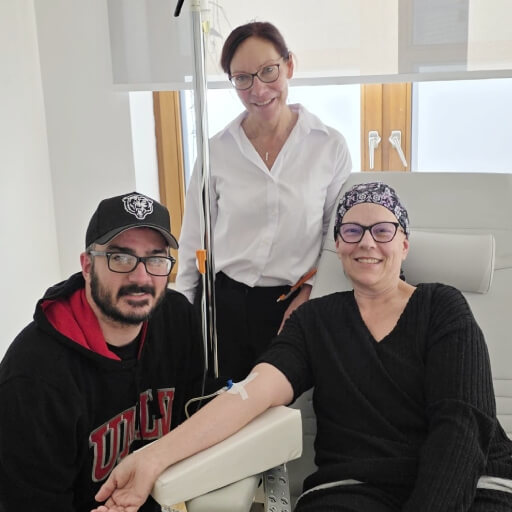
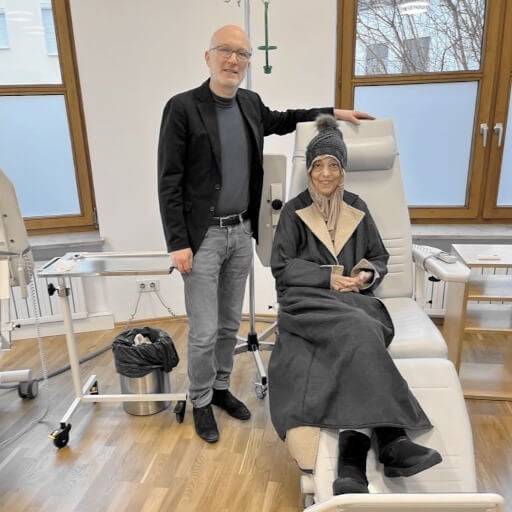
Real Patient Experiences: Cancer Treatment Success Stories
For Magdalena Ivanova, hope came unexpectedly from dendritic cell therapy at a German clinic. As a stage 4 breast cancer patient with bone metastases she had undergone years of conventional treatment in Bulgaria – eight years of monthly hospital visits, intense chemotherapy sessions and a long recovery from radical mastectomy.
It was then that her children began researching new cancer treatments worldwide. They found out about LDG Laboratories in Berg, Germany, through Booking Health, which provided personalized breast cancer immunotherapy with dendritic cells. This immune system boosting treatment surprised Magdalena at first not with the effectiveness, but with tolerability: she did not suffer from severe side effects usual for systemic medications.
The treatment process was also simple and did not require any preparation. Healthcare specialists took about 150ml of Magdalena’s blood, created a personalized vaccine in the laboratory and administered it as a simple injection. Under the guidance of an experienced professor at LDG Laboratories, Magdalena received comprehensive care.
Perhaps most striking was the contrast in her quality of life during treatment. Where traditional therapy had once dominated her daily routine with restrictions and side effects, dendritic cell therapy allowed her to maintain her normal lifestyle. Her success story at the German clinic illuminates the possibilities that modern breast cancer immunotherapy offers to advanced breast cancer patients.
Possibly most striking was her poor quality of life during the previous treatment, which Magdalena was afraid of now. Where conventional therapies had limited her daily life with side effects and restrictions, dendritic cell therapy allowed her to live normally again. Her success story at the German clinic highlights the options that modern breast cancer immunotherapy can offer advanced breast cancer patients.
"This Treatment Changed Everything": Magdalena Ivanova on Dendritic Cell Therapy in Germany
The Best Clinics for Immunotherapy in Germany
Germany has several specialized and comprehensive oncology centers for breast cancer immunotherapy. Each facility uses advanced therapeutic approaches for hormone receptor positive breast cancer (HR+, HER2+) and triple-negative breast cancer care.
- LDG Laboratories in Berg has become a world leader in dendritic-cell immunotherapy to activate immune system and kill cancer cells. And their expertise is particularly useful for patients with advanced breast cancer. The LDG Laboratories' personalized approach to vaccine creation has demonstrated impressive results – particularly in breast cancer patients seeking alternative therapies against breast cancer cells or additions to conventional therapies.
- The University Hospital Frankfurt am Main integrates breast cancer immunotherapy into a comprehensive program to boost the immune response. Their multidisciplinary approach combines immune treatments with surgical techniques and precision radiotherapy using CyberKnife. The hospital's tumor board ensures each patient receives care tailored to their specific condition and peculiarities of breast cancer cells.
- At the Clinic of Advanced Biological Medicine in Frankfurt am Main, doctors blend traditional immuno-oncology (IO) with biological therapies, focusing on strengthening the immune system while managing treatment side effects. Their four-decade experience in integrative medicine has helped establish protocols that enhance both survival rates and quality of life.
- The Asklepios Hospital Barmbek Hamburg offers state-of-the-art breast cancer immunotherapy treatments. Their medical team of 1,600 professionals serves an impressive patient volume annually, maintaining high standards to treat breast cancer recognized by the German Cancer Society.
- For patients seeking complementary approaches, the Hyperthermia Center Hannover combines immunotherapy with innovative hyperthermia treatments that influence sensitivity of breast cancer cells to therapeutic interventions. The facility offers comprehensive outpatient care that is able to destroy cancer cells and address psychological aspects of breast cancer treatment.
How Can a Woman with Breast Cancer Undergo Immunotherapy in Germany?
Pre-Treatment Preparations
Before traveling to Germany for hormone receptor positive breast cancer (HR+, HER2+) or triple-negative breast cancer immunotherapy (TNBC), several important steps need to be completed in your home country. The process begins with collecting and translating your medical records, including diagnosis details, previous treatments, and recent examination results. These documents are essential for German specialists to evaluate your case and determine the most appropriate immunotherapy approach. Initial consultations can often be conducted remotely, allowing you to discuss treatment options with German doctors while still at home.
Many women wonder about the timing of immunotherapy in relation to their current breast cancer treatment. German specialists can provide guidance on whether to complete ongoing treatments before starting immunotherapy or if a combination approach would be more beneficial.
Treatment Organization in Germany
Being already exhausted from multiple treatment sessions, having consulted numerous specialists, and having tried various therapeutic interventions, finding the best treatment strategy for your clinical situation can become a challenging task. In such a situation, it is easy to choose a first-hand option or to follow standardized therapeutic protocols with a long list of adverse effects instead of selecting highly specialized innovative treatment options.
To make an informed choice and get a personalized cancer management plan, which will be tailored to your specific clinical situation, consult medical experts at Booking Health. Being at the forefront of offering the latest medical innovations for already 12 years, Booking Health possesses solid expertise in creating complex cancer management programs in each case. As a reputable company, Booking Health offers personalized stage 4 breast cancer treatment plans with direct clinic booking and full support at every stage, from organizational processes to assistance during treatment. We provide:
- Assessment and analysis of medical reports
- Development of the medical care program
- Selection of a suitable treatment location
- Preparation of medical documents and forwarding to a suitable clinic
- Preparatory consultations with clinicians for the development of medical care programs
- Expert advice during the hospital stay
- Follow-up care after the patient returns to their native country after completing the medical care program
- Taking care of formalities as part of the preparation for the medical care program
- Coordination and organization of the patient's stay in a foreign country
- Assistance with visas and tickets
- A personal coordinator and interpreter with 24/7 support
- No hidden costs
Health is an invaluable aspect of our lives. Delegating management of something so fragile yet precious should be done only to experts with proven experience and a reputation. Booking Health is a trustworthy partner who assists you in pursuing stronger health and a better quality of life. Contact our medical consultant to learn more about the possibilities of personalized treatment with innovative methods for metastatic breast cancer with leading specialists in this field.
Immunotherapy Journey: Dendritic Cell Treatment with Booking Health
Frequently Asked Questions About Immunotherapy for Breast Cancer in Germany
Send request for treatmentImmunotherapy for breast cancer in Germany types: checkpoint inhibitors like PD-1/PD-L1 blockers, individualized dendritic cell vaccines, and CAR T-cell therapy where your own immune cells are modified. Checkpoint inhibitors are pretty simple – IV infusions every few weeks. More individualized dendritic cell therapy requires two visits.
The effectiveness of immunotherapy in TNBC in Germany is actually quite good. KEYNOTE-522 reported increased complete response rates and overall survival when an IT medication was added to the chemotherapy. High PD-L1 expression and more tumor-infiltrating lymphocytes (TIL) make triple-negative breast cancer more responsive to immunotherapy than other breast cancer types.
The side effects of immunotherapy for breast cancer in Germany are way milder than chemo. Checkpoint inhibitors might cause fatigue, loss of appetite, nausea, or diarrhea – but these are occasional and minor. Dendritic cell therapy is even gentler, letting patients keep up their normal daily activities. That's why it works well even for stage 4 patients who are already exhausted from other treatments.
As for patient selection and biomarkers for breast immunotherapy in Germany, doctors check PD-L1 expression levels in your tumor – it must be high for checkpoint inhibitors to work. Then they check the level of tumor-infiltrating lymphocytes (TIL) and the cancer subtype. The best immune system's response is for TNBC. German specialists conduct thorough testing prior to treatment to determine which immunotherapy type suits your case.
The cost of immunotherapy for breast cancer in Germany varies considerably according to treatment type. Dendritic cell therapy costs EUR20,000-38,000. Checkpoint inhibitors are EUR375,000-420,000 per full course. Most expensive is CAR T-cell therapy at EUR450,000-550,000. They depend on your cancer stage, tumor type, and more. Dendritic cell therapy has highest response rates.
Several clinics for immunotherapy for breast cancer in Germany offer advanced treatments. LDG Laboratories in Berg specializes in dendritic cell therapy with over 2,500 procedures done. University Hospital Frankfurt am Main combines immunotherapy with surgery and CyberKnife. Asklepios Hospital Barmbek Hamburg has modern facilities. Hyperthermia Center Hannover adds complementary approaches to immunotherapy.
Yes, it is: immunotherapy and combination therapy for breast cancer in Germany are common. Checkpoint inhibitors are added to chemo, especially before surgery to shrink tumors. For more advanced cases, doctors use immunotherapy + hormone therapy + RT. The dendritic cell vaccines may be combined with other treatments. The good tolerability permits such combinations without adding serious side effects.
Booking Health immunotherapy support for breast cancer in Germany includes analysis of medical reports and organization of appointments. They help you choose the right clinic, prepare documents, book consultations with specialists, deal with visas and tickets and assign you a personal coordinator with 24 hours support.
Choose treatment abroad and you will for sure get the best results!
Authors:
This article was edited by medical experts, board-certified doctors Dr. Nadezhda Ivanisova, and Dr. Bohdan Mykhalniuk. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Our editorial policy, which details our commitment to accuracy and transparency, is available here. Click this link to review our policies.
Sources:
[1] Ran R, Chen X, Yang J, Xu B. Immunotherapy in breast cancer: current landscape and emerging trends. Exp Hematol Oncol. 2025;14:77. doi:10.1186/s40164-025-00667-y. [DOI]
[2] Liying Li, Fan Zhang, Zhenyu Liu, Zhimin Fan. Immunotherapy for Triple-Negative Breast Cancer: Combination Strategies to Improve Outcome. Cancers (Basel). 2023 Jan 3;15(1):321. doi: 10.3390/cancers15010321. [DOI] [PMC free article]
[3] Essalihi A, Bouchra O, Khadiri K, Khadrouf Z, Karkouri M. Immunotherapy for triple-negative breast cancer: current trends and future prospects. J Egypt Natl Canc Inst. 2025;37:51. doi:10.1186/s43046-025-00295-x. [DOI]
[4] Debien V, De Caluwé A, Wang X, Piccart-Gebhart M, Tuohy VK, Buisseret L. Immunotherapy in breast cancer: an overview of current strategies and perspectives. NPJ Breast Cancer. 2023;9:7. doi:10.1038/s41523-023-00508-3. [DOI]
[5] Qian D, Li J, Huang M, Cui Q, Liu X, Sun K. Dendritic cell vaccines in breast cancer: immune modulation and immunotherapy. Biomed Pharmacother. 2023;162:114685. doi:10.1016/j.biopha.2023.114685. [DOI]
Read:
Comprehensive Guide to Breast Cancer Treatment: New and Standard Treatment Options