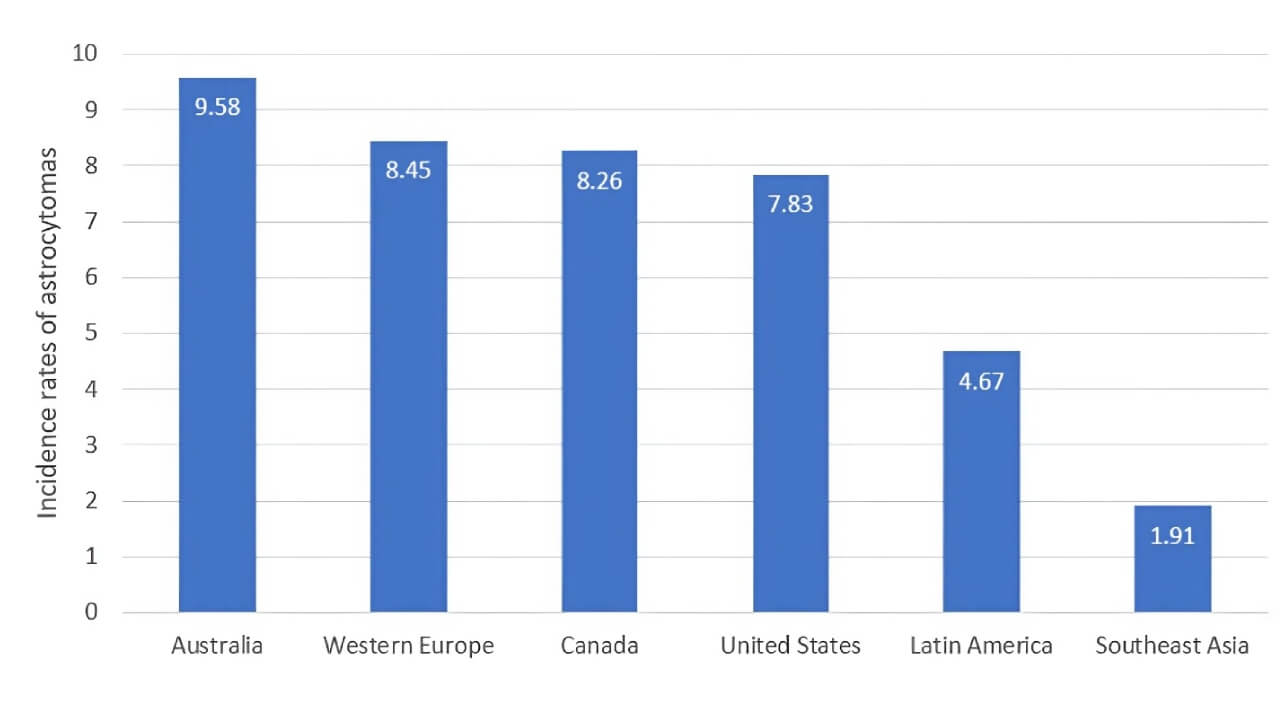
The reality drives the urgent need for novel and more effective astrocytoma treatments. Astrocytoma group of neoplasms includes relatively slow-growing grades I–III and grade IV – glioblastoma, mentioned among the most lethal cancers. In the U.S., gliomas strike roughly 6 per 100,000 people annually [1]. That is, each year, about 25,400 malignant brain or spinal astrocytoma are diagnosed – and roughly 18,760 people do not survive them.
The clinical distinction between astrocytoma and glioblastoma matters. Glioblastoma progresses rapidly; low-grade astrocytomas, including astrocytoma grade 2, follow a slower course – yet demand monitoring, since transformation into aggressive forms remains a risk.
Standard Treatment Approaches: Surgery, Proton Therapy & Radiation
Treatment plan for astrocytoma of the brain typically involves a combination: surgery and radiation-based methods. These reduce tumor burden and delay progression – though vary in precision, side effects, and long-term outcomes.
Advanced Neurosurgical Techniques in Astrocytoma Management
Modern neurosurgery bears little resemblance to what it was two decades ago. Large incisions, high neurological risk, weeks of recovery – those assumptions no longer hold. Today's techniques reach tumors once considered untouchable, and they do so with far greater precision.
Endoscopic endonasal surgery (EES) approaches the tumor through the nasal passages entirely – no craniotomy, no brain retraction. For midline and skull base astrocytomas, this means dramatically reduced recovery time, fewer postoperative complications, and no visible scarring. Patients with tumors near the optic nerve or pituitary region often regain normal function with striking speed.
Not every case suits EES, of course. Another option is keyhole craniotomy – smaller, strategically positioned openings that access the tumor with surrounding structures largely intact. Clinical advantages are less blood loss, shorter hospital stays, lower infection rates versus conventional open surgery. Precision without the collateral cost.
And then there are tumors positioned against the brain's most critical zones – language centers, motor pathways. How do surgeons operate there without causing the very damage they're trying to prevent? Awake brain mapping solves that problem. Patients are sedated but conscious and perform tasks in real time while surgeons detect and protect the eloquent cortex during brain tissue resection. Quality-of-life outcomes have significantly improved as a result. It is now the gold standard for surgery in functional brain zones – and rightly so.
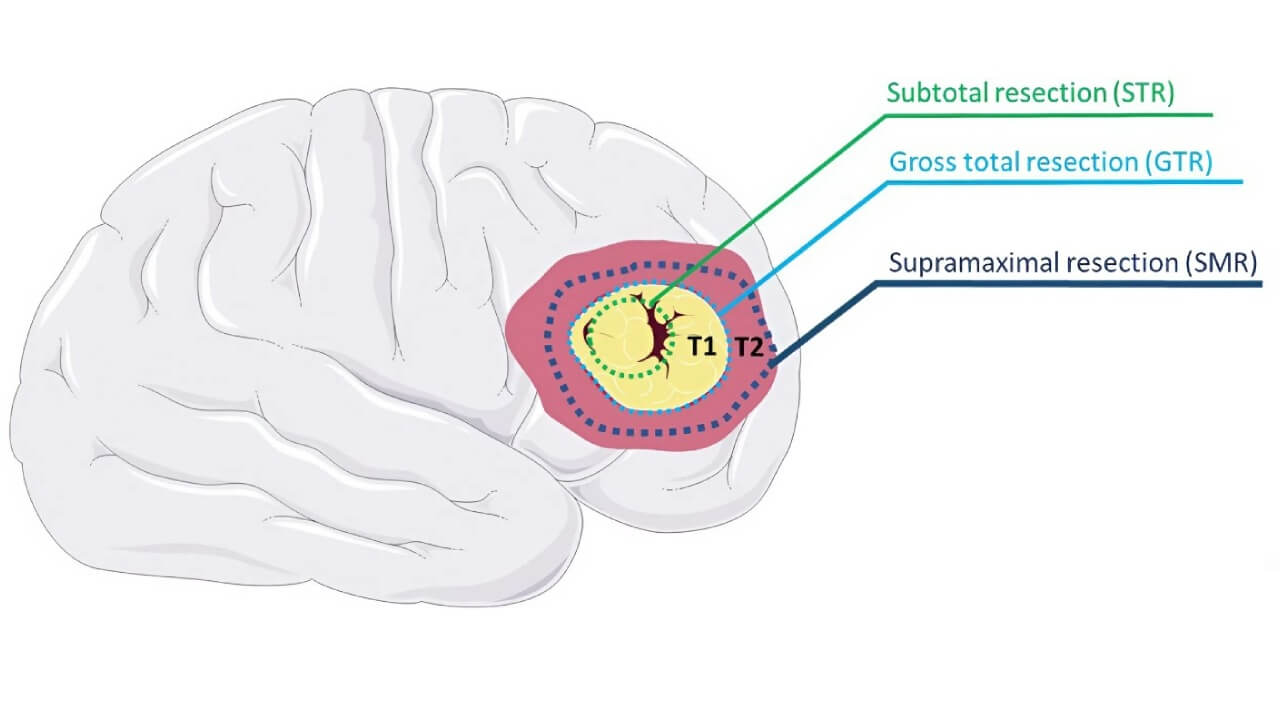
The illustration below summarizes current surgical strategies, matched to tumor location and grade. These options expand the treatment landscape for patients with both low- and high-grade astrocytomas.
Proton Therapy in Brain Astrocytoma
Proton beam therapy exploits a fundamental principle of physics: positively charged particles release most of their energy precisely at the tumor site – the Bragg peak – then stop. No significant exit dose. No unnecessary radiation scattering through healthy tissue beyond the target.
The evidence behind this precision is compelling. A systematic review covering over 800 glioma patients across grades II–IV found survival rates comparable to conventional radiotherapy – with notable advantages in protecting cognitive- and neuro-sensitive regions [3]. Dosimetric comparisons with VMAT and 3D-CRT revealed mean dose reductions of up to 99% in the contralateral hippocampus [4]. For patients facing long-term neurocognitive consequences, that number is significant.
Precision Radiation Therapy in Brain Astrocytoma
Radiation remains foundational to astrocytoma treatment – particularly following surgical resection. Its role: targeting residual tumor cells that surgery cannot safely reach and slowing disease progression. Standard protocols typically deliver 50–60 Gy across daily sessions over approximately six weeks.
The results, when radiation integrates into a multimodal regimen, can be striking. One large investigation reported a doubling of two-year survival when radiation combined with systemic therapy – compared to radiation alone [5].
Modern delivery systems – Intensity-Modulated Radiation Therapy (IMRT) and Volumetric-Modulated Arc Therapy (VMAT) – sculpt the dose to match the tumor's precise three-dimensional shape, sparing adjacent critical structures and reducing the cognitive toll that radiation has historically carried. Better targeting. Fewer consequences. More life preserved.
Reprogramming Immunity: How Dendritic Cell Therapy Is Shaping the Future of Brain Tumor Care
What if the powerful weapon against brain tumors was already inside the body? Dendritic cell therapy operates on exactly that premise – harnessing the immune system's own architecture to identify, target, and eliminate astrocytoma cells with a precision that conventional treatments simply cannot match. Highly personalized, mechanistically elegant, and carrying a far gentler side-effect profile than standard therapies, it represents one of the most compelling shifts in neuro-oncology today.
How It Works
Dendritic cells are the immune system's educators. Their core function: presenting antigens to T-cells, effectively instructing the body's defenses on what to destroy. This mechanism – and its profound implications for medicine – earned Canadian immunologist Ralph M. Steinman the 2011 Nobel Prize in Physiology or Medicine [6].
The process is deeply personal. A patient's immune cells are collected, loaded with tumor-specific antigens in the laboratory, then reintroduced into the body. After the activation reprogrammed dendritic cells can cross the blood-brain barrier – a boundary many drugs never breach – and direct the immune system against astrocytoma cells with high specificity.
Targeted. Adaptive. Entirely the patient's own biology, turned against the tumor.
Why This Matters in The Treatment of Astrocytoma Brain Tumor
Radiation and chemotherapy don't make difference. Healthy tissue and cancerous tissue absorb the damage together – a fundamental limitation that becomes especially consequential inside the brain. Dendritic cell therapy overcomes this issue and confines the immune response to malignant cells alone.
The advantages are numerous:
- Selective targeting.
- Immune response can evolve as the tumor mutates, reducing the risk of relapse and immune memory enables ongoing, lifelong, surveillance against cancer cell regrowth.
- Lower toxicity.
- Blood-brain barrier access.
If you’re looking into astrocytoma treatment options, this innovative immunotherapy for astrocytoma may offer new hope – especially when conventional approaches are limited.
Clinical Evidence and Use Cases in Brain Astrocytoma
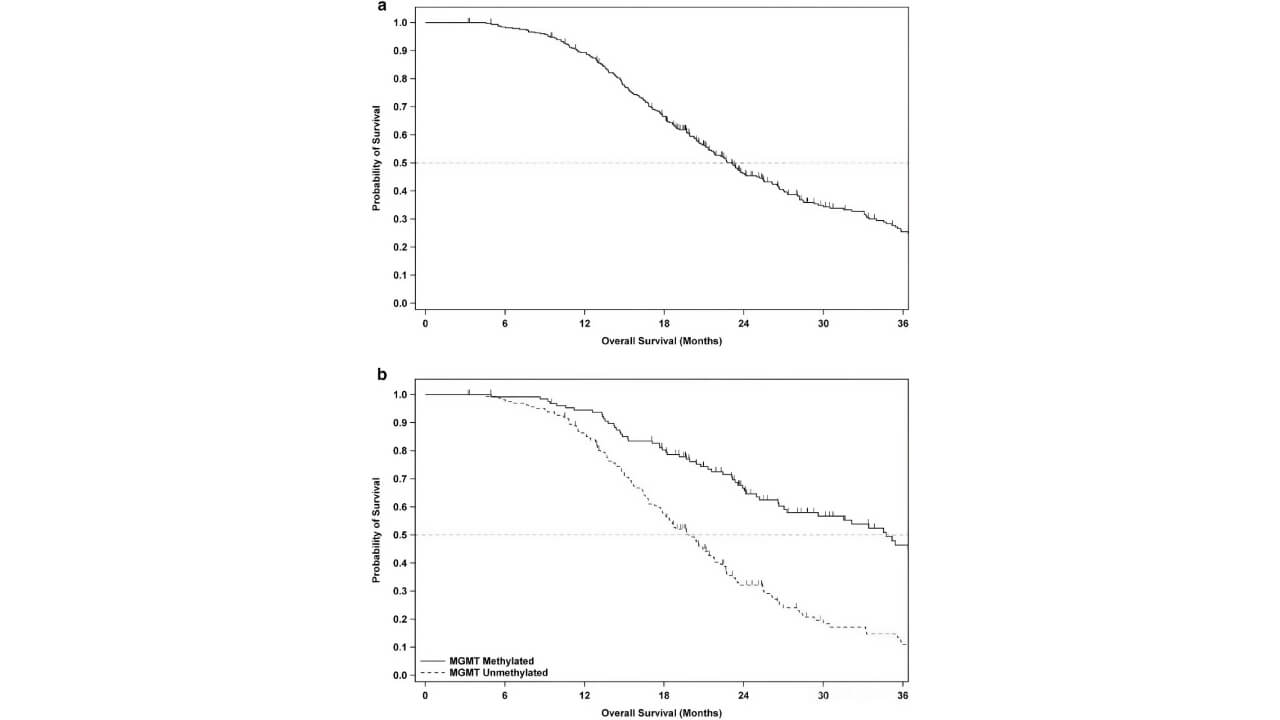
Recent Phase III studies have shown encouraging results. One large-scale trial involving over 300 glioblastoma patients found that adding dendritic cell vaccination to standard care extended median overall survival and significantly improved five-year survival rates – from 5.7% to over 13% [7]. Side effects were minimal and mostly limited to mild flu-like symptoms.
This approach is now being considered across different stages of astrocytoma, including:
- After surgical resection, to target remaining tumor cells.
- As part of multimodal regimens, complementing radiation and other systemic therapies.
- In recurrent or inoperable astrocytoma brain tumors, where other options may be limited.
It’s especially valuable in patients seeking new glioma treatments that go beyond conventional methods.
New Treatments for Brain Astrocytoma: Interventional Radiology Techniques
For patients with astrocytomas in surgically risky areas, minimally invasive procedures guided by imaging offer a safe effective alternative. Interventional radiology is an essential part of the modern neuro-oncology. Its methods help reduce surgical complications and enhance local tumor control. Let’s take a closer look at different options.
Laser Interstitial Thermal Therapy (LITT) for Brain Astrocytoma
LITT uses focused laser energy. It ablates tumor tissue from within and is guided in real-time by magnetic resonance imaging. The method offers several important clinical benefits:
- Accesses the tumor through a small skull opening with minimal disruption to surrounding tissue
- Uses real-time MRI to guide heat delivery, ensuring precise control of thermal damage
- Preserves healthy brain structures while effectively destroying tumor cells
- Particularly suitable for small tumors and patients who cannot undergo conventional surgery
- May temporarily open the blood–brain barrier, improving the delivery of subsequent treatments
This approach has shown favorable survival outcomes in selected patients – with deep-seated or recurrent gliomas. [8]
Electrochemotherapy for Brain Astrocytoma
Different problem, different tool. Electrochemotherapy doesn't destroy tissue thermally – it exploits electric pulses to momentarily increase cancer cell membrane permeability, allowing chemotherapeutic agents to penetrate tumor cells up to 300 times more efficiently than standard delivery [9]. Effects remain confined strictly to the treated region. The procedure can be completed in a single session, even intraoperatively when circumstances allow – making it particularly valuable for tumors in eloquent or surgically complex areas.
When Chemo Can't Get Inside Cancer Cells: The Electroporation Solution
Embolization for Brain Astrocytoma
Then there's the question of blood supply. Highly vascular astrocytomas feed on it – and embolization attacks that dependency directly, cutting off tumor-feeding arteries before surgery even begins. Angiography first identifies and maps those vessels with precision; embolic materials – particles, glues, or coils – then travel through microcatheters to seal them off. The procedure is typically performed 24–48 hours before resection, allowing maximum effect to take hold.
The surgical payoff is significant [10]. Less intraoperative bleeding means surgeons can work more thoroughly and more safely, achieving more complete tumor removal with reduced risk to surrounding structures – particularly valuable when the lesion sits near critical brain regions. Well-established in neurosurgical planning and continuously refined through newer embolic agents and advanced imaging guidance, embolization remains one of the most strategically important preparatory steps in complex astrocytoma surgery.
| Treatment Approach | Response Rate | Survival Benefit | Side Effects | Treatment Duration | Treatment Cost Range (Europe) |
|---|---|---|---|---|---|
| Surgery | 60-80% (early stages of glioblastoma) 20-30% (advanced) | Foundation for other treatments | Pain, infection risk, and recovery time | One-time procedure | €25,000 - €50,000 |
| Conventional Radiation | 40-60% (early) 15-20% (advanced) | Part of the standard protocol | Fatigue, skin irritation, cognitive effects | 6 weeks (daily sessions) | €28,000 - €42,000 |
| Proton Therapy | 50-70% (early) 15-25% (advanced) | Similar to conventional radiation with reduced side effects | Mild to moderate | 6 weeks (daily sessions) | €56,900 - €90,500 |
| Dendritic Cell Therapy | 85-95% (early) 60-80% (advanced) | Potential for long-term survival benefit | Minimal (primarily flu-like symptoms) | One-time procedure with lasting effects | €20,000 - €38,000 |
| Electrochemotherapy | ~70% complete response in studies | 9-14 months median survival improvement | Localized effects, minimal systemic impact | Single session | €30,000 - €45,000 per treatment course |
| Laser Interstitial Thermal Therapy | Best for tumors under 11cc | ~11.5 months for recurrent disease | Minimal | One-time procedure | Part of the surgical costs |
From Diagnosis to Recovery in Brain Astrocytomaa
Marco was 42, an architect from northern Italy, and wasn't worried at first. Memory lapses, occasional confusion – easy to dismiss. But the symptoms escalated: visual disturbances, speech hesitation. A brain MRI delivered the answer no one wanted. A low-grade astrocytoma, left temporal lobe, positioned precisely where language and memory converge.
Italian specialists offered standard resection and radiotherapy. The tumor's location made that a significant gamble. His family began looking elsewhere – searching for a center that paired genuine medical innovation with something equally important: a personalized approach to the person behind the diagnosis.
Through Booking Health, they reached the astrocytoma treatment Germany offers: a specialized neuro-oncology clinic. The multidisciplinary team didn't offer a protocol. They built a plan – one centered on dendritic cell therapy, an advanced immunotherapy designed to retrain Marco's own immune system to recognize and eliminate cancer cells. Careful tumor resection using intraoperative mapping preserved cognitive function throughout. A series of dendritic cell vaccinations, developed from his own tumor antigens and white blood cells, followed. Adjunctive proton beam radiation and personalized rehabilitation completed the pathway.
Follow-up with MRIs showed no recurrence (over 18 months). So, Marco regained full independence, even returned to his profession, and reported no significant neurological deficits. "We chose a center that didn't just know how to treat low-grade astrocytoma in adults," he said. "They treated me as a person." That distinction matters more than it seems.
Hope in Cancer Treatment: Patient Success with Booking Health
Advanced-Stage Astrocytoma: Standard Treatment Fails — Innovation Offers New Hope
A late-stage brain tumor diagnosis can feel like a door closing. Rounds of treatment, limited response, narrowing options – for patients with astrocytoma grade 4, the sense that the disease has moved beyond reach is understandable. Fortunately, modern medicine doesn't stop where conventional protocols do.
Traditional approaches play a role. But they are no longer the only path, the landscape has shifted. For high-grade astrocytoma, personalized strategies – targeted therapy, precision RT, immunological methods – produce differences in outcome, often with a gentler side-effect profile than standard high-dose regimens. What determines the right approach is no longer the diagnosis alone: genetic mutations, prior therapy response, and overall health all shape the most effective course.
Leading clinics abroad now offer comprehensive, individualized treatment plans for astrocytoma and glioblastoma treatment – and through Booking Health, patients can access these programs directly, without delays or unnecessary intermediaries. Even at stage 4 astrocytoma, meaningful decisions remain available.
This isn't about false hope. It's about knowing where to look – and moving before time runs out.
A Medical Journey: Every Step of the Way With Booking Health
Finding the best treatment strategy for your clinical situation is a challenging task. Being already exhausted from multiple treatment sessions, having consulted numerous specialists, and having tried various therapeutic interventions, you may be lost in all the information given by the doctors. In such a situation, it is easy to choose a first-hand option or to follow standardized therapeutic protocols with a long list of adverse effects instead of selecting highly specialized innovative treatment options.
To make an informed choice and get a personalized cancer management plan, which will be tailored to your specific clinical situation, consult medical experts at Booking Health. Being at the forefront of offering the latest medical innovations for already 12 years, Booking Health possesses solid expertise in creating complex cancer management programs in each individual case. As a reputable company, Booking Health offers personalized astrocytomas treatment plans with direct clinic booking and full support at every stage, from organizational processes to assistance during treatment. We provide:
- Assessment and analysis of medical reports
- Development of the medical care program
- Selection of a suitable treatment location
- Preparation of medical documents and forwarding to a suitable clinic
- Preparatory consultations with clinicians for the development of medical care programs
- Expert advice during the hospital stay
- Follow-up care after the patient returns to their native country after completing the medical care program
- Taking care of formalities as part of the preparation for the medical care program
- Coordination and organization of the patient's stay in a foreign country
- Assistance with visas and tickets
- A personal coordinator and interpreter with 24/7 support
- Transparent budgeting with no hidden costs
Health is an invaluable aspect of our lives. Delegating management of something so fragile yet precious should be done only to experts with proven experience and a reputation. Booking Health is a trustworthy partner who assists you on the way of pursuing stronger health and a better quality of life. Contact our medical consultant to learn more about the possibilities of personalized treatment with innovative methods for astrocytomas with leading specialists in this field.
Frequently Asked Questions About Brain Astrocytoma
Send request for treatmentTumor of astrocytes in the CNS that affects adults and pediatric patients is an astrocytoma. Diagnosis involves MRI and biopsy; neuro-oncology specialists guide treatment.
Can be benign (low-grade) or malignant (high-grade). MRI and biopsy determine the tumor type. After the diagnosis histological confirmation, treatment includes: surgery, radiotherapy, and chemotherapy, dendritic cell vaccination – depending on the case.
Symptoms include: headaches, seizures, blurred vision, neurological deficits, etc. Tumors near the brainstem may affect vital functions, be life threatening.
Grades from I (to understand: pilocystic, benign) to IV (that is, glioblastoma, malignant) exist. Grading affects prognosis and the best treatment options for brain astrocytoma.
High-grade, malignant CNS tumor. Tumor board discussions guide complex therapy with simultaneous or sequential options and monitoring for recurrence.
Benign, low-grade tumor mostly found in pediatric patients. Surgical resection is used, and prognosis – in most cases – is excellent.
No single cause defines it. Genetic mutations and environmental factors like radiation can contribute.
Survival depends on tumor grade and treatment. Low-grade astrocytomas may allow long life with monitoring; high-grade types have shorter survival—but novel treatment options give additional years of life.
Life expectancy varies: low-grade patients often live 10+ years; high-grade median survival is under 2 years. Early diagnosis and multimodal treatment improve prognosis that is why the choice of a specialized healthcare facility matters.
Diagnosis includes MRI, CT, and biopsy – to assess tumor type and grade. Neurologists and neuro-oncology teams carry out a clinical examination first and evaluate symptoms like seizures and blurred vision.
Low grade astrocytoma can often be cured or controlled long-term by surgery. High grade astrocytoma requires aggressive therapy; cure is rare, but treatment improves survival.
Treatment includes craniotomy or other approaches to tumor resection, radiotherapy, chemotherapy, and immunotherapy, including dendritic cell vaccines. Tumor boards tailor therapy to patient needs.
Surgery is usually needed for biopsy and tumor removal—but may be limited by tumor location, or patient condition. In some cases, monitoring or non-surgical therapy is used.
Grade 4 astrocytoma (glioblastoma) has a poor prognosis with a median survival of about 12-18 months. Adding novel options improves prognosis.
Glioblastoma is a grade 4 astrocytoma – that is malignant and aggressive. Astrocytoma vs glioblastoma means: all glioblastomas are astrocytomas, not all astrocytomas are glioblastomas.
Grade shapes survival dramatically. Low-grade astrocytomas show 5-year survival over 70%, high-grade below 20%. Early diagnosis and comprehensive oncology care are vital.
Yes, dendritic cell therapy is used in addition to traditional surgery, radiotherapy, and chemotherapy. It aims to improve survival and reduce recurrence.
Advanced neuro-oncology care with experts in neurosurgery, radiotherapy, and chemotherapy, plus access to innovative immunotherapy options – these are available in Germany.
Look for multidisciplinary teams (neurologists, neurosurgeons, oncologists, etc). Booking Health, the specialized medical tourism provider) helps find top specialists and personalized treatment plans.
Astrocytoma treatment can combine surgery (keyhole or endoscopic), proton or radiation therapy, and innovative methods such as dendritic cell therapy, electrochemotherapy (ECT), and laser interstitial thermal therapy (LITT). Typically, the choice depends on tumor grade and location.
In Europe, astrocytoma treatment prices range from €20,000 to €90,500: surgery €25,000-€50,000, proton therapy €56,900-€90,500, dendritic cell therapy €20,000-€38,000, and ECT €30,000-€45,000. In particular, Germany offers high-quality care at moderate prices, while Great Britain tends to be more expensive. In contrast to Europe, countries, such as Australia, often provide limited access to advanced therapies (e.g., dendritic cell or proton therapy). Even when available, the cost can be several times higher than in European clinics.
Results of astrocytoma treatment can vary by method and tumor grade. To be specific, surgery can achieve 60-80% response in early stages and 20-30% in advanced ones. In turn, proton therapy can reach 50-70%, dendritic cell therapy up to 95% (early) and 80% (advanced), and ECT about 70%.
During astrocytoma treatment, radiation may cause fatigue and cognitive changes. On the other hand, proton therapy can help minimize these risks. In turn, dendritic cell therapy usually causes mild flu-like symptoms, while ECT and LITT have short-term, localized effects.
As astrocytoma treatment approaches, surgery and LITT are one-time procedures. In turn, proton and radiation therapy typically last six weeks. On the other hand, dendritic cell therapy and ECT are completed in a single session.
New astrocytoma treatments have improved patient outcomes. For example, the addition of dendritic cell therapy can more than double five-year survival, ECT can extend median survival by 9-14 months, and proton therapy can help preserve brain function and long-term quality of life.
The best treatment option for brain astrocytoma focuses on innovative, minimally invasive techniques, that provide advantages over standard therapy. In Germany advanced options include laser interstitial thermal therapy (LITT), electrochemotherapy and tumor embolization (which allow targeted tumor control while preserving healthy brain tissue).
The best hospitals for brain astrocytoma treatment are specialized neuro-oncology centers experienced in innovative procedures. In Germany such hospitals offer access to laser interstitial thermal therapy (LITT), electrochemotherapy and embolization (supported by multidisciplinary teams and advanced intraoperative technologies).
Choose treatment abroad and you will for sure get the best results!
Authors:
This article was edited by medical experts, board-certified doctors Dr. Nadezhda Ivanisova, and Dr. Bohdan Mykhalniuk. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Our editorial policy, which details our commitment to accuracy and transparency, is available here. Click this link to review our policies.
Sources:
[1] Medscape. Astrocytoma: Practice Essentials, Background, Pathophysiology. https://emedicine.medscape.com/article/283453-overview
[2] Open Exploration. Update for astrocytomas: medical and surgical management considerations. https://www.explorationpub.com/Journals/en/Article/10069
[3] Nicolas Goliot, Selim Mohssine, Dinu Stefan et al. Proton therapy for adult-type diffuse glioma: A systematic review. Crit Rev Oncol Hematol. 2024 Dec:204:104501. doi: 10.1016/j.critrevonc.2024.104501. Epub 2024 Sep 7. [DOI] [PubMed]
[4] S Adeberg, S B Harrabi, N Bougatf et al. Intensity-modulated proton therapy, volumetric-modulated arc therapy, and 3D conformal radiotherapy in anaplastic astrocytoma and glioblastoma : A dosimetric comparison. Strahlenther Onkol. 2016 Nov;192(11):770-779. doi: 10.1007/s00066-016-1007-7. Epub 2016 Jun 22. [DOI] [PubMed]
[5] Luluel Khan, Hany Soliman, Arjun Sahgal, James Perry, Wei Xu, May N Tsao. External beam radiation dose escalation for high grade glioma. Cochrane Database Syst Rev. 2020 May 21;2020(5):CD011475. doi: 10.1002/14651858.CD011475.pub3. [DOI] [PMC free article]
[6] The Nobel Prize. Nobel Prize in Physiology or Medicine 2011, Ralph M. Steinman Facts. https://www.nobelprize.org/prizes/medicine/2011/steinman/facts/
[7] Journal of Translational Medicine. First results on survival from a large Phase 3 clinical trial of an autologous dendritic cell vaccine in newly diagnosed glioblastoma. https://translational-medicine.biomedcentral.com/articles/10.1186/s12967-018-1507-6
[8] John F de Groot, Albert H Kim, Sujit Prabhu et al. Efficacy of laser interstitial thermal therapy (LITT) for newly diagnosed and recurrent IDH wild-type glioblastoma. Neuro-Oncology Advances, Volume 4, Issue 1, January-December 2022, vdac040. doi: 10.1093/noajnl/vdac040. [DOI]
[9] Birgit Agerholm-Larsen, Helle K. Iversen, Per Ibsen et al. Preclinical Validation of Electrochemotherapy as an Effective Treatment for Brain Tumors. Cancer Res (2011) 71 (11): 3753–3762. doi: 10.1158/0008-5472.CAN-11-0451. [DOI]
[10] Duffis EJ, Gandhi CD, Prestigiacomo CJ, Abruzzo T, Albuquerque F, Bulsara KR, et al. Head, neck, and brain tumor embolization guidelines. J Neurointerv Surg. 2012;4(4):251–255. doi: 10.1136/neurintsurg-2012-010350. [DOI]
Read:
Brain cancer treatments in Germany
Brain Cancer Treatment – Full Guide: All New Brain Cancer Treatment Options