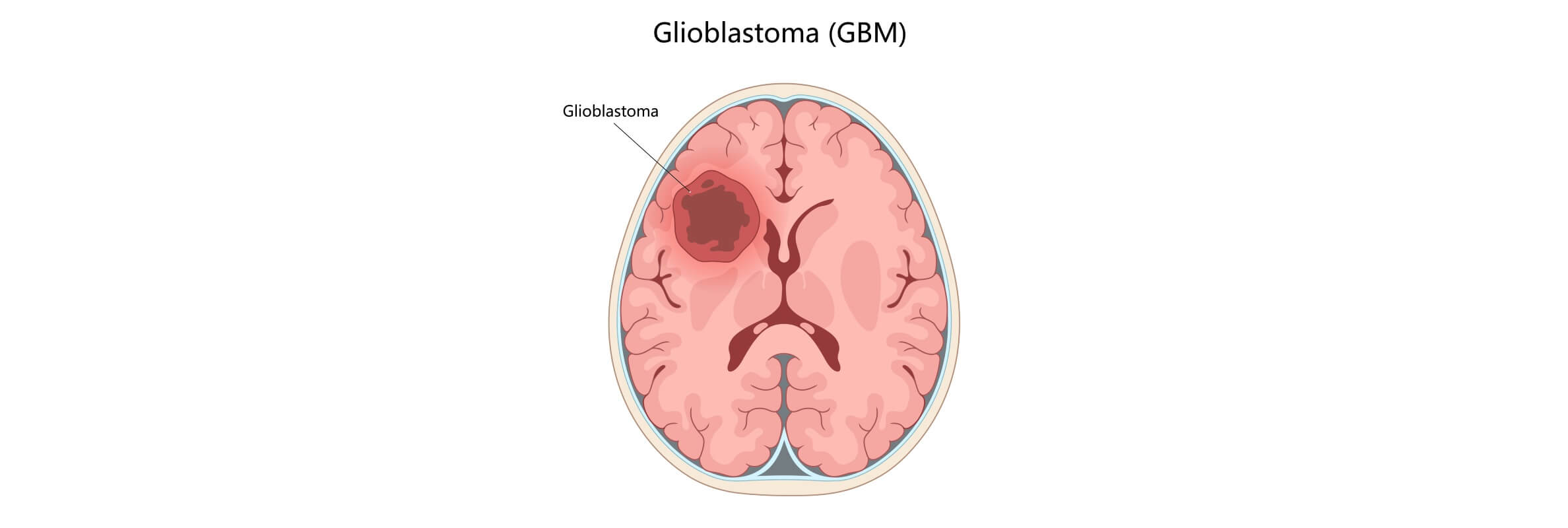
Glioblastoma (GBM) is the most common primary malignant tumor of the brain and accounts for about 16% of all primary neoplasms of the brain and central nervous system [1]. The average age-standardized incidence rate is estimated at 3.2 cases per 100,000 population [2]. As one of the most aggressive forms of brain cancer, glioblastoma represents a major therapeutic challenge despite advances in glioblastoma treatment strategies. In the vast majority of cases, glioblastoma is localized in the hemispheres of the brain, but isolated cases are also described in the brain stem, cerebellum, and spinal cord. Overall, glioblastoma belongs to the group of highly infiltrative brain tumors, characterized by diffuse invasion of the surrounding brain tissue by glioblastoma cells.
Glioblastoma Overview
About 61% of all primary gliomas occur within the four lobes of the brain, with predominant localization in the frontal (25%), temporal (20%), parietal (13%), and, much less frequently, occipital lobe (3%). The aggressive behavior of these cancer cells and their tendency to infiltrate eloquent brain regions significantly complicate surgical and adjuvant glioblastoma treatment [3].
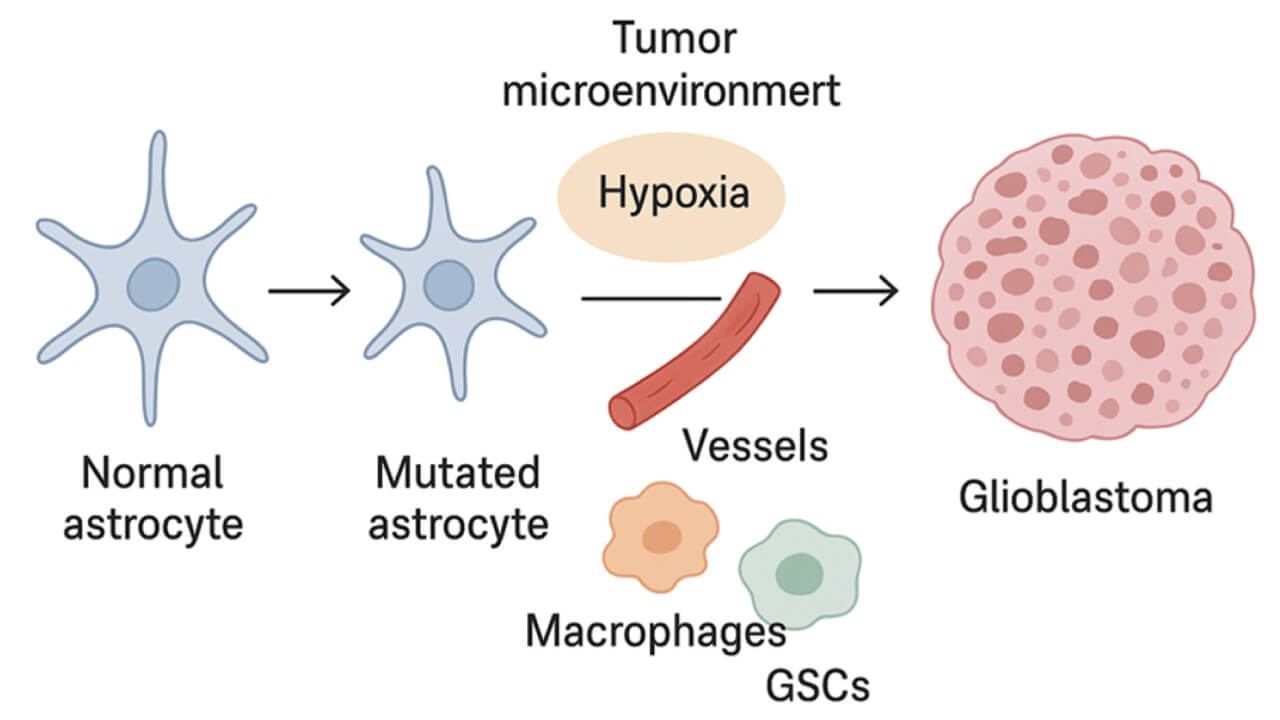
For a long time, it was believed that glioblastoma originates exclusively from differentiated glial cells. However, modern research suggests that the tumor may arise from different cell populations that have properties similar to neural stem cells. Such cells are at different stages of differentiation from stem to neuronal and glial forms, and the phenotypic diversity of glioblastomas is due mainly to molecular disturbances in signaling pathways, rather than differences in cellular origin. This biological complexity explains the growing interest in personalized therapeutic approaches, including advanced glioblastoma therapy in Germany, where molecular profiling increasingly guides therapeutic decision-making.
A multidisciplinary team plays a key role. The neurosurgeon ensures the safest possible removal of the tumor, creating a basis for further therapy. The radiotherapist is responsible for planning and conducting radiation therapy aimed at destroying residual tumor cells. The chemotherapist forms systemic therapy taking into account the molecular features of the tumor, and the pathologist performs a critical role in accurate histological and molecular verification of the diagnosis.
Special attention in the modern treatment of glioblastoma is paid to immuno-oriented approaches. In particular, dendritic cell therapy is considered a promising direction aimed at activating immune cells through the use of dendritic cells capable of "training" the immune system to recognize tumor antigens. Such strategies complement standard treatments and reflect current understanding of glioblastoma biology.
It is the combination of surgery, radiation therapy, systemic therapy, and immunological approaches that allows you to maximally influence the course of the disease and, at the same time, preserve the patient's neurological functions and quality of life.
Glioblastoma Treatment in Germany
Modern approaches continue to improve outcomes in glioblastoma treatment. Germany offers structured, evidence-based care with access to advanced neurosurgery, radiotherapy, and innovative therapies. Treatment of glioblastoma in Germany is based on a standardized, evidence-based approach, which is fundamentally important for the management of aggressive brain tumors. For glioblastoma patients, the key stage is careful therapeutic planning, which begins with a full diagnostic assessment.
It is mandatory to perform contrast-enhanced brain MRI to determine tumor localization, degree of infiltration, and involvement of functionally significant areas. Neuroimaging data serve as the basis for planning the surgical stage and subsequent brain cancer treatment. After obtaining the tumor tissue, a histological study is performed with mandatory evaluation of molecular markers, in particular MGMT and IDH, which have a prognostic and predictive value and influence the choice of further cancer treatment tactics.
All clinical decisions are made at a multidisciplinary tumor board, which includes a neurosurgeon, radiotherapist, chemotherapist and neuropathologist. This format allows the integration of imaging, morphology and molecular research data into a single individual treatment plan. This is of particular importance in cases of recurrent glioblastoma, when a re-evaluation of the possibilities of surgical intervention, radiation or systemic therapy is necessary.
Within the modern approach to the treatment of glioblastoma in certain clinical situations, immuno-oriented methods can be considered. In particular, dendritic cell vaccines aim to modulate the immune system by activating specific immune response. In these strategies, dendritic cells are used to stimulate the antitumor activity of immune cells and can be applied as an adjunct to standard treatments within an individualized plan or clinical protocols.
Thus, GBM treatment in Germany is based on accurate diagnosis, assessment of tumor molecular characteristics and collegial decision-making, which ensures a consistent and personalized approach to patient management.
Glioblastoma Surgery in Germany
Surgery is a key stage of glioblastoma treatment and the basis of the subsequent treatment plan. The main goal of the operation is the safest possible surgical resection of the tumor with the simultaneous preservation of neurological functions, which corresponds to the principles of standard treatment and determines the effectiveness of further standard therapy.
The infiltrative growth of glioblastoma significantly complicates operative treatment, as tumor cells spread beyond the visualized tumor and penetrate the surrounding healthy tissues. Even after complete macroscopic resection, microscopic residual disease often persists, necessitating adjuvant treatment.
In Germany, glioblastoma neurosurgery is based on the application of modern methods, in particular neuronavigation, intraoperative MRI, intraoperative ultrasound and fluorescence surgery using 5-ALA. These technologies improve intraoperative imaging of the tumor and allow optimizing the volume of resection with minimal risk of damage to functionally significant areas of the brain.
In the presence of damage to critical areas of the brain, functional mapping methods are additionally used, which contributes to the preservation of speech and motor functions. If surgery is associated with high risk or is not possible, glioblastoma is treated with conventional treatments, including radiotherapy and systemic therapy, according to current clinical protocols.
Thus, therapeutic strategy is individualized based on tumor location, functional risk, and imaging findings, with a primary focus on glioblastoma surgery. Germany offers access to specialized neuro-oncology centers with extensive surgical expertise [4].
Radiotherapy for Glioblastoma in Germany
Radiation therapy is a mandatory component of the standard treatment of glioblastoma and is used in most patients after surgery or biopsy. In view of the infiltrative growth of glioblastoma, it is radiation that aims to control the microscopic residual tumor, which cannot be eliminated surgically. This makes radiation therapy a key component of complex cancer treatment.
Treatment of glioblastoma in Germany with radiation therapy usually starts 3-6 weeks after surgery. Most German clinics use a combination of normofractionated radiotherapy according to international guidelines. This approach provides optimal local control of the tumor and is the basis of standard therapy.
Modern techniques and the accuracy of irradiation
Modern glioblastoma therapy in Germany is based on high-precision IMRT (Intensive Modulated Radiation Therapy) and VMAT (Volumetric Modulated Arc Therapy) technologies.
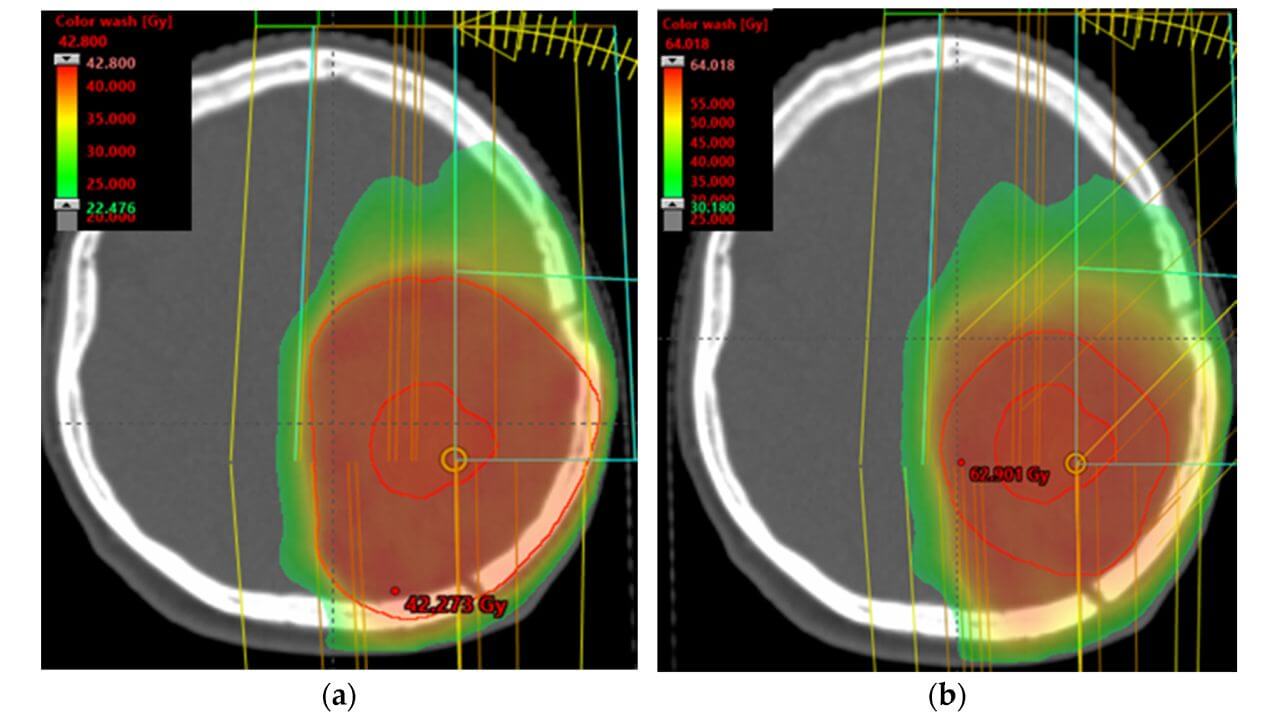
These methods allow the most accurate delivery of the radiation dose to the tumor zone, while minimizing exposure to surrounding healthy brain tissues. Treatment planning is based on a combination of CT and MRI studies, which ensures accurate determination of exposure volume and risk organs. The use of IGRT further increases the reproducibility and safety of the therapy.
One of the priorities of modern radiotherapy is the maximum protection of healthy brain structures. Thanks to accurate planning and modern techniques, it is possible to reduce the risk of neurological toxicity and preserve the quality of life of patients, which is especially important with long-term therapy [5].
Alternative regimes and special clinical situations
For elderly or functionally weakened patients, hypofractionated radiation therapy regimens are used, which have better effectiveness and tolerability. In cases of recurrent GBM, the possibility of repeated exposure is considered individually, taking into account previously received doses and the general condition of the patient, often in combination with other treatments.
Radiation therapy is an integral part of modern glioblastoma treatment and is provided into the overall therapy strategy alongside surgery and systemic treatment. The use of high-tech approaches in German clinics allows to achieve high accuracy, effective tumor control and an optimal balance between the effectiveness and safety of treatment.
Proton Therapy for Glioblastoma in Germany
Proton radiation therapy is a modern radiation option, which, in selected clinical situations, is considered within the scope of glioblastoma treatment in Germany. Unlike photon radiation therapy, protons have unique physical properties that allow for delivering energy with high spatial accuracy. A key feature is the Bragg Peak effect, in which the main dose of radiation is deposited at a well-defined depth, with a minimum dose and with virtually no significant escape from the tumor.
The biological action of protons is realized through the ionization of the molecules and precise damage to the DNA of tumor cells, which leads to their death and control of tumor growth. In clinical practice, within the treatment of glioblastoma, doses are calculated in grey equivalents (GyE), which provides a correct comparison with photon radiotherapy.
The main potential advantage of proton therapy in brain cancer is the pronounced dosimetric saving of healthy brain tissues. Due to the high dose conformity, the integral radiation load on critical structures is reduced, which is important for reducing the risk of neurocognitive and neuroendocrine complications, especially when the tumor is located near functionally significant areas.
In clinical practice, proton therapy is not the standard for all patients with glioblastoma, but can be considered individually, in particular with complex anatomical localization of the tumor, the need for repeated radiation, or in patients who have already been treated with other methods of radiation therapy. The decision to use proton therapy is made by a multidisciplinary team taking into account clinical, anatomical, and technical factors [6].
Dendritic Cell Therapy for Glioblastoma in Germany
Glioblastoma belongs to aggressive brain tumors and remains one of the most difficult problems of modern cancer treatment, even with the use of standard multimodal therapy. That is why immuno-oriented approaches are considered for individual glioblastoma patients at any stage of the disease within the brain cancer treatment.
Dendritic cell therapy (DC therapy) belongs to active immunotherapy and aims to activate a patient's immune system. Dendritic cells are key antigen-presenting cells that play a central role in the functioning of the immune system and the formation of a specific adaptive immune response. They are responsible for recognizing tumor antigens and transmitting this information to other immune cells, primarily T-lymphocytes [7].
The discovery of dendritic cells was recognized with the Nobel Prize, highlighting their fundamental importance in immunology [8]. The mechanism of dendritic cell therapy consists of the use of dendritic cells obtained from the patient's body, which, in laboratory conditions, are loaded with tumor-associated glioblastoma antigens. After insertion back into the body, these dendritic cells migrate to the lymph nodes, where they initiate a specific immune response. As a result, cytotoxic T-cells and T-helper cells are able to destroy glioblastoma cells.
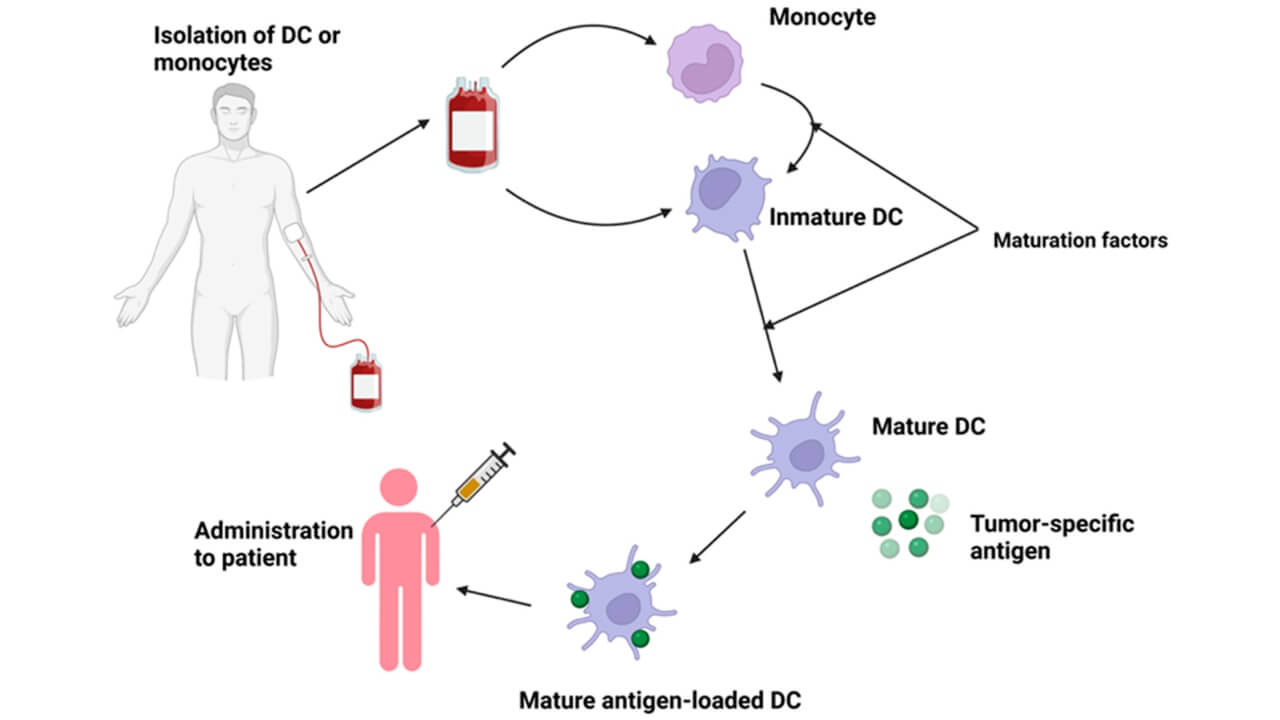
Below is a typical protocol for dendritic cell therapy:
Day 1 (30min): At the first appointment the patient’s history is taken, the informed consent is made and other possible therapeutic options, nutrition and complementary medicines are discussed with the patient.
Day 2 (90min): In the morning 150-200ml of blood is drawn, followed by an infusion containing vitamin C and vitamin B-complex. Furthermore, an intramuscular vitamin D injection (50.000 IU) is given for stimulation of the immune cells (NK). Patients can have breakfast before blood collection.
Day 9 (90min): The DCs are delivered around noon. Patients can have breakfast before DC-therapy. Dendritic cells are injected intradermally as recommended. An infusion containing vitamin C and vitamin B-complex is given. Furthermore, an intramuscular vitamin D injection (50.000 IU) is given. Patients are advised to continue vitamin D supplementation with 40.000 IU per week orally.
Side effects and tolerability
Dendritic cell therapy is generally well tolerated. Possible side effects are usually minimal and mild, including:
- local injection site reactions (redness, induration, mild pain)
- slight increase in temperature
- flu-like symptoms
- fatigue or mild headache.
Serious complications are rarely observed. In most patients, treatment does not require hospitalization and is not accompanied by a significant deterioration in the quality of life.
Importantly, dendritic cell vaccination does not replace standard treatment, but is seen as an adjunct to it. Dendritic cell therapy for glioblastoma in Germany can be used most often as part of personalized programs or in case of recurrence of the disease, when the possibilities of standard therapy are limited. Such an approach not only aims at the direct control of the tumor, but also at the formation of immunological memory, potentially allowing the disease to be kept under control longer by activating the body's immune system [8].
In this exclusive interview, Prof. Gansauge, head of a clinic specializing in innovative dendritic cell therapy, explains in detail the scientific foundations and clinical possibilities of this method. In the video, the professor talks about the discovery of dendritic cell therapy, the principles of work of dendritic cell vaccines, indications for use in oncology, in particular in the complex treatment of malignant tumors, as well as the possibility of combining immunotherapy with other types of treatment. Particular attention is paid to practical aspects: from patient selection and therapy to safety, side effects and real clinical outcomes, including cases of long-term remission.
Thus, dendritic cell therapy is an example of modern immunotherapy that uses natural immune response mechanisms to target the tumor and expands the possibilities of glioblastoma treatment in Germany.
Below is a comparative table of glioblastoma treatment options, summarizing indications, possible side effects, and key advantages and disadvantages of each approach. This format helps you to comprehensively evaluate treatment options and understand their role in the overall treatment strategy.
| Treatment Type | Indications | Side effects | Advantages | Disadvantages |
|---|---|---|---|---|
| Surgery | All localized tumors | Pain, infection risk, recovery time | Complete tumor removal, potentially curative for early stages | Risk of complications (bleeding, infection, adverse reactions to anesthesia). Extended recovery period and hospitalization. Risk of recurrence. Need for additional treatments. |
| Radiotherapy (Proton Beam Therapy) | Primary focus of malignant tumor and metastases to the brain | Mild to moderate | Minimal damage to surrounding tissue, precise targeting, reduced long-term side effects. | Limited availability. Higher cost compared to conventional radiation. Limited to brain, eye, and spinal cord tumors, pediatric cancers. |
| Chemotherapy and Radiotherapy | Malignant tumors of all stages | Severe (nausea, fatigue, hair loss, immunosuppression, skin irritation) | Synergistic effect, can be given before/after surgery | Increased toxicity, increased risk of severe side effects. Reduced quality of life during treatment. Extended treatment duration. Limited effectiveness, especially for advanced cancers. |
| Dendritic Cell Vaccination | Malignant tumors of all stages | Minimal (flu-like symptoms) | Highly personalized, life-long immunity after a single injection, minimal side effects | Individualized manufacturing available at specialized centers only. |
The Patient's Story: The Way Through Glioblastoma and Hope
The story of Daria Rogers is the path of a patient diagnosed with glioblastoma multiforme, a rare and aggressive form of brain cancer, which she went through with her husband Maurice. After the diagnosis, the couple quickly realized that there is no time for doubts, and standard treatment options have limited possibilities.
Daria openly talks about the moment of diagnosis, fear, and confusion, but at the same time, about the determination to look for all possible options. That is why it was decided to consider treatment abroad. In the search process, they learned about dendritic cell therapy, an innovative immunotherapeutic approach that became a real chance for them.
By contacting Booking Health, Daria and Maurice received clear, structured information and support at every stage, from the development of an individual treatment program and the organization of urgent access to therapy and full patient support at all stages of glioblastoma treatment in Germany.
As Maurice recalls:
"It was important for us not just to find a method of treatment, but to understand what and why we are doing. Booking Health helped us quickly and without too much chaos".
The procedure for dendritic cell therapy, according to Daria, turned out to be much simpler than she expected and was well-tolerated. Already a few months after treatment, the control MRI showed results that became a turning point for the whole family.
"We sincerely believe that it was dendritic cell therapy that could be responsible for such outcomes", – says Daria.
Separately, the couple notes the role of the doctor and the clinic team in Germany – not only from the professional side, but also from the human side. Support, a calm explanation of each step, and a sense of partnership greatly enhanced confidence and fighting spirit during a challenging period.
Today, Daria shares her story publicly, not for her own sake, but for the sake of other glioblastoma patients:
"Don't lose hope. It is important to act early and act quickly. If we can help at least one person – it already makes sense".
The couple also emphasizes that dendritic cell therapy is not opposed to other methods, but can be part of a comprehensive treatment strategy.
"We will always be grateful to Booking Health and our manager Kate for being with us on this path", – adds Maurice.
See the full interview, where Daria and Maurice detail their journey from diagnosis to treatment in Germany, the real results of dendritic cell therapy, and words of support for other glioblastoma patients.
VIDEO
Daria Rogers, Ireland: How Modern Cancer Treatment in Germany Changed My Glioblastoma Prognosis
Dendritic Cell Therapy
FIND THE RIGHT SPECIALIST FOR MY CASE
Ron Czenczek's path to Germany began in the same place Daria's did: a diagnosis that left his healthcare system with nothing further to offer. Diagnosed with glioblastoma grade IV in December 2024, Ron went through months of high-dose chemotherapy and radiation in Canada — treatment so debilitating that he spent weeks unable to leave the couch. His oncologists were not evasive about the ceiling. They stated it clearly: the tumor might be slowed, but it would not shrink. That sentence is what his wife Freya could not accept.
Three independent physicians, when asked for alternatives, gave her the same answer: try Germany. Through Booking Health, the family organized treatment within days of their first inquiry — a process Ron's wife describes as transformative simply because someone took the logistics off her hands at the moment she had no capacity to manage them alone.
The dendritic cell therapy Ron received required no hospitalization. He sat in a chair, received vitamin infusions alongside the treatment, and experienced only a brief low-grade fever afterward — the fever that signals the immune system has recognized its target. Two subsequent MRI scans showed the tumor was smaller. The result his Canadian doctors had told him would not happen had happened.
Approaching two years since a prognosis of one to two years, Ron is planning camping trips and cycling with his children. As Freya puts it: "I have my husband. My kids have their father. You can't put a price on that." Watch the video below to hear them tell the full story.
VIDEO
Glioblastoma Grade 4: How Dendritic Cell Therapy in Germany Shrank Ronald’s "Terminal" Tumor
Dendritic Cell Therapy
BOOK CONSULTATION
Combined Glioblastoma Treatment in Germany
Treatment of glioblastoma in Germany is seen as a step-by-step strategy in which the combination of methods is of fundamental importance, given the malignant form of the disease. After oncologists manage to diagnose glioblastoma, an individual treatment plan is formed for each patient, which takes into account the volume of the lesion, molecular characteristics of the tumor, and the general functional state.
- The basis remains standard treatment, which, if possible, begins with the surgical resection. The reduction in tumor volume creates conditions of minimal residual disease, which is relevant for the effectiveness of further stages of treatment of glioblastoma.
- After surgery, most patients receive radiation therapy (including proton therapy as indicated) in combination with systemic treatment, which belongs to conventional treatments and is aimed at controlling the microscopic tumor process with the maximum possible preservation of healthy tissues.
- Within the combined approach, immuno-oriented options may also be considered in Germany, in particular dendritic cell-based vaccine therapy. Such methods belong to the category of cancer vaccines and are aimed at activating the body's immune system to form a specific antitumor immune response. This approach is considered the most promising against the background of minimal residual disease or after the completion of standard stages of treatment.
- Some clinical programs adopt individualized approaches, including personalized peptide vaccines, that are tailored to the antigenic profile of the tumor. Such options do not replace standard treatment, but are integrated into the general treatment program as an addition to surgery, radiation, and systemic therapy.
Thus, the combined treatment of glioblastoma in Germany is based on a consistent combination of techniques from surgery to adjuvant and immunotherapeutic strategies. It is this multicomponent tactic that allows you to make the most of the potential of standard and innovative approaches in the treatment of this complex disease.
Below is a comparative table of the cost of the main methods of glioblastoma treatment. It helps to navigate the financial aspects of each approach, understanding that the final cost is always formed individually and depends on the amount of treatment, the clinical situation, the chosen clinic, and the need for additional procedures or diagnostics.
| Treatment type | Germany | USA | Great Britain | Australia |
|---|---|---|---|---|
| Surgery | €25,000 – €45,000 | €65,000 – €85,000 | €35,000 – €55,000 | €20,000 –€50,000 |
| Radiotherapy (Proton Beam Therapy) | €46,900 – €86,500 | €80,000 – €140,000 | €60,000 – €95,000 | €145,000 – €360,000 |
| Chemotherapy and Radiotherapy | €21,100 – €58,400 for 1 cycle | €47,000 – €140,000 for 1 cycle | €35,000 – €83,000 for 1 cycle | up to €50,000 |
| Dendritic cell vaccine | €20,000 – €38,000 | €100,000 – €150,000 | not available | not available |
Recurrent Glioblastoma Treatment in Germany
As considered in modern neuro-oncology, glioblastoma is one of the most aggressive brain tumors, the recurrence of which is practically inevitable. The average progression-free survival is about 7 months from diagnosis. Recurrent glioblastoma is associated with an unfavorable prognosis: the median overall survival usually does not exceed one year, and there is no generally accepted standard of care in this clinical situation.
In case of recurrence of the disease, treatment is often palliative in nature. That is why in oncology, decisions regarding further treatment tactics must be strictly individualized, taking into account the potential benefits, risks and impact on the patient's quality of life.
In Germany, different categories of treatment approaches are considered for recurrence of glioblastoma. Locoregional techniques include repeated surgery in the presence of indications, repeated or focal radiotherapy, and the use of tumor treating fields (TTF) technologies. In parallel, the feasibility of systemic therapies is evaluated, including chemotherapy, targeted agents, and glioblastoma immunotherapy Germany [9].
Of particular interest in relapse are immuno-oriented approaches, including vaccination, which can be considered as part of an individualized treatment strategy in specialized centers. Such methods are not the standard, but can be integrated into a comprehensive plan, provided that patients are carefully selected.
Due to the lack of a single standard of care, obtaining a second opinion on medical treatment is a particular value in the recurrence of glioblastoma. Consultation in specialized centers in Germany allows you to re-evaluate the clinical situation, compare all available options, and form a reasonable individual treatment plan in accordance with modern oncology capabilities.
Benefits of Treatment in Germany
- Clear standards and clinical protocols
Cancer treatment is carried out in accordance with international recommendations with strict quality control, which is especially important for GBM patients. Combined treatment strategies are essential for improving outcomes in glioblastoma patients. Germany offers access to advanced neurosurgery, radiotherapy, and innovative immunotherapy options.
- Multidisciplinary tumor boards
Each case is considered collegially with the participation of neurosurgeons, radiotherapists, medical oncologists, and neuropathologists. This allows for individual solutions to be formed even in complex or recurrent situations.
- Modern neurosurgery
Access to high-precision neuronavigation, intraoperative MRI, functional mapping, and fluorescent surgery increases the safety of interventions and expands treatment options.
- Innovative treatment methods
Innovative approaches are increasingly integrated into glioblastoma immunotherapy. Germany provides access to specialized centers with experience in immune-based treatment strategies, which can be considered as an addition to standard treatment for selected patients who want to more actively fight brain cancer.
- Developed medical infrastructure
Specialized neuro-oncology centers, modern diagnostics, and experienced teams form the environment in which the best hospitals in Germany for glioblastoma treatment work.
- Coordination and continuity of treatment
All stages – from the initial consultation to treatment and follow-up – are built as a single, logical system without wasting time.
A separate role in this process is played by Booking Health, which helps patients organize treatment in Germany in a comprehensive manner: from selecting a clinic and obtaining a second opinion to coordinating visits, translations, and logistics. Such support allows patients to focus on the main thing – treatment and recovery.
A Medical Journey: Every Step of the Way With Booking Health
Finding the best treatment strategy for your clinical situation is a challenging task. Being already exhausted from multiple treatment sessions, having consulted numerous specialists, and having tried various therapeutic interventions, you may be lost in all the information given by the doctors. In such a situation, it is easy to choose a first-hand option or to follow standardized therapeutic protocols with a long list of adverse effects instead of selecting highly specialized innovative treatment options.
To make an informed choice and get a personalized cancer management plan, which will be tailored to your specific clinical situation, consult medical experts at Booking Health. Being at the forefront of offering the latest medical innovations for already 12 years, Booking Health possesses solid expertise in creating complex cancer management programs in each case. As a reputable company, Booking Health offers personalized glioblastoma treatment plans with direct clinic booking and full support at every stage, from organizational processes to assistance during treatment. We provide:
- Assessment and analysis of medical reports
- Development of the medical care program
- Selection of a suitable treatment location
- Preparation of medical documents and forwarding to a suitable clinic
- Preparatory consultations with clinicians for the development of medical care programs
- Expert advice during the hospital stay
- Follow-up care after the patient returns to their native country after completing the medical care program
- Taking care of formalities as part of the preparation for the medical care program
- Coordination and organization of the patient's stay in a foreign country
- Assistance with visas and tickets.
- A personal coordinator and interpreter with 24/7 support
- Transparent budgeting with no hidden costs
Health is an invaluable aspect of our lives. Delegating management of something so fragile yet precious should be done only to experts with proven experience and a reputation. Booking Health is a trustworthy partner who assists you in pursuing stronger health and a better quality of life. Contact our medical consultant to learn more about the possibilities of personalized treatment with innovative methods for glioblastoma with leading specialists in this field.
Hope in Cancer Treatment: Patient Success with Booking Health
Frequently Asked Questions About Glioblastoma Treatment in Germany
Send request for treatmentNew approaches within glioblastoma treatment in Germany include advanced therapies for GBM, such as tumor treating fields, immunotherapy strategies, and personalized treatment protocols integrated with standard care. These methods complement standard GBM therapy and are considered on an individual basis.
GBM therapy in Germany is the most optimal variant due to its evidence-based protocols, high-volume neuro-oncology centers, and access to innovative treatments. Patients also turn to obtain a glioblastoma second opinion in Germany, which emphasizes the authority of this country.
The best places are specialized neuro-oncology centers in Germany with experience in complex brain tumors, access to multidisciplinary care, and participation in advanced treatment programs.
The cost of glioblastoma treatment in Germany varies depending on the treatment strategy, including surgery, radiotherapy, chemotherapy, and optional advanced therapies. Final costs are determined individually after medical review.
Core glioblastoma treatment options include surgery, radiotherapy, chemotherapy, Tumor Treating Fields, and selected cases of glioblastoma immunotherapy in Germany, all combined within a comprehensive treatment strategy.
Glioblastoma treatment planning in Germany is performed through a multidisciplinary tumor board. Glioblastoma treatment is usually considered by the team of neurosurgeons, oncologists, radiotherapists, and pathologists, who jointly define the optimal approach.
Glioblastoma surgery in Germany focuses on maximal safe resection of glioblastoma, aiming to reduce tumor burden while preserving neurological function, and is a cornerstone of treatment when feasible.
Radiotherapy for glioblastoma in Germany is used postoperatively or after biopsy and includes precision radiotherapy glioblastoma techniques such as IMRT, VMAT, or proton therapy within GBM radiation therapy in Germany.
Yes, chemotherapy for glioblastoma in Germany is a standard component of care. Glioblastoma treatment includes chemo as a part of first-line therapy.
Tumor treating fields are a non-invasive treatment method that uses alternating electric fields to disrupt tumor cell division and may be integrated into standard GBM therapy for selected patients.
Yes, glioblastoma immunotherapy in Germany is available in selected centers and may include vaccine-based or immune-modulating approaches as part of advanced therapies for GBM.
Recurrent glioblastoma treatment in Germany includes repeat surgery, re-irradiation, systemic therapy, and immunotherapy options, forming GBM recurrence treatment options. Second-line glioblastoma therapy is based on individual assessment.
Patients typically select among the best hospitals in Germany for glioblastoma treatment by considering experience, outcomes, access to innovation, and the expertise of glioblastoma doctors in Germany.
Choose treatment abroad and you will for sure get the best results!
Authors:
This article was edited by medical experts, board-certified doctors Dr. Nadezhda Ivanisova, and Dr. Daria Sukhoruchenko. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Our editorial policy, which details our commitment to accuracy and transparency, is available here. Click this link to review our policies.
Sources:
[1] Jigisha P Thakkar, Therese A Dolecek, Craig Horbinski et al. Epidemiologic and Molecular Prognostic Review of Glioblastoma. Cancer Epidemiol Biomarkers Prev. 2014 Jul 22;23(10):1985–1996. doi: 10.1158/1055-9965.EPI-14-0275. [DOI] [PMC free article]
[2] Quinn T Ostrom, Haley Gittleman, Jordonna Fulop et al. CBTRUS Statistical Report: Primary Brain and Central Nervous System Tumors Diagnosed in the United States in 2008-2012. Neuro Oncol. 2015 Oct 26;17(Suppl 4):iv1–iv62. doi: 10.1093/neuonc/nov189. [DOI] [PMC free article]
[3] Mary Elizabeth Davis. Glioblastoma: Overview of Disease and Treatment. Clin J Oncol Nurs. 2016 Oct 1;20(5):S2–S8. doi: 10.1188/16.CJON.S1.2-8. [DOI] [PMC free article]
[4] Stephen J Price, Jasmine G Hughes, Swati Jain et al. Precision Surgery for Glioblastomas. J Pers Med. 2025 Feb 28;15(3):96. doi: 10.3390/jpm15030096. [DOI] [PMC free article]
[5] Castalia Fernández, Raquel Ciérvide, Ana Díaz et al. Radiotherapy in Glioblastoma Multiforme: Evolution, Limitations, and Molecularly Guided Future. Biomedicines. 2025 Sep 1;13(9):2136. doi: 10.3390/biomedicines13092136. [DOI] [PMC free article]
[6] Nicholas Aderinto, Gbolahan Olatunji, Emmanuel Kokori et al. A review of proton beam therapy’s role in glioma management. Medicine (Baltimore). 2025 Jul 4;104(27):e43071. doi: 10.1097/MD.0000000000043071. [DOI] [PMC free article]
[7] Angeliki Datsi, Rüdiger V Sorg. Dendritic Cell Vaccination of Glioblastoma: Road to Success or Dead End. Front Immunol. 2021 Nov 2;12:770390. doi: 10.3389/fimmu.2021.770390. [DOI] [PMC free article]
[8] Roman Volchenkov, Florian Sprater, Petra Vogelsang, Silke Appel. The 2011 Nobel Prize in physiology or medicine. Scand J Immunol. 2012 Jan;75(1):1-4. doi: 10.1111/j.1365-3083.2011.02663.x. [DOI] [PubMed]
[9] Maria Angeles Vaz-Salgado, María Villamayor, Víctor Albarrán et al. Recurrent Glioblastoma: A Review of the Treatment Options. Cancers (Basel). 2023 Aug 26;15(17):4279. doi: 10.3390/cancers15174279. [DOI] [PMC free article]
[10] Karol Sadowski, Adrianna Jażdżewska, Jan Kozłowski et al. Revolutionizing Glioblastoma Treatment: A Comprehensive Overview of Modern Therapeutic Approaches. Int. J. Mol. Sci. 2024, 25(11), 5774. doi: 10.3390/ijms25115774. [DOI]
[11] Domingos Roda, Pedro Veiga, Joana Barbosa Melo et al. Principles in the Management of Glioblastoma. Genes 2024, 15(4), 501. doi: 10.3390/genes15040501. [DOI]
[12] Kinga Królikowska, Katarzyna Błaszczak, Sławomir Ławicki et al. Glioblastoma—A Contemporary Overview of Epidemiology, Classification, Pathogenesis, Diagnosis, and Treatment: A Review Article. Int. J. Mol. Sci. 2025, 26(24), 12162. doi: 10.3390/ijms262412162. [DOI]
Read:
Treatment for Glioblastoma – Full Guide: New and Standard Treatments
Innovative Treatment for Glioblastoma in Germany: Dendritic Cell Therapy for Cancer