Metastatic brain lesions occur approximately 10 times more frequently than primary tumors, accounting for approximately 200,000 of the 225,000 brain tumors diagnosed each year. The increasing incidence of brain metastases is associated with improved treatment of primary malignant tumors, which in turn leads to increased survival [1].
Neurosurgical interventions pursue two aims: removing pathological loci in the brain and preserving healthy surrounding nervous tissue. Only a combination of these two factors guarantees the success of the procedure and the absence of complications.
Magnetic resonance imaging (MRI) is an extremely helpful technique that is aimed at investigating the structure of the brain and detecting harmful changes. Now this technique is an integral part of the cutting-edge intervention – MRI-guided laser ablation with the help of Visualase™ system.
The Visualase brain tumor treatment makes complex neurosurgical procedures much more comfortable for patients. Once a doctor recommends that you undergo brain surgery, you should definitely check to see if this technique is suitable for your medical case.
How Does the Visualase™ System Work?
The Visualase brain tumor treatment consists of several technical components that provide controlled and safe laser ablation of brain tissue.
MRI-guided laser ablation consists of a few consecutive steps. The first one is the stereotactic procedure – taking detailed 3D scans and determining the exact localization of the abnormal brain region. In contrast to the usual 2D images, the stereotactic frame provides the doctor with a stereoscopic picture and, thus, more comprehensive information. This is called "neuronavigation".
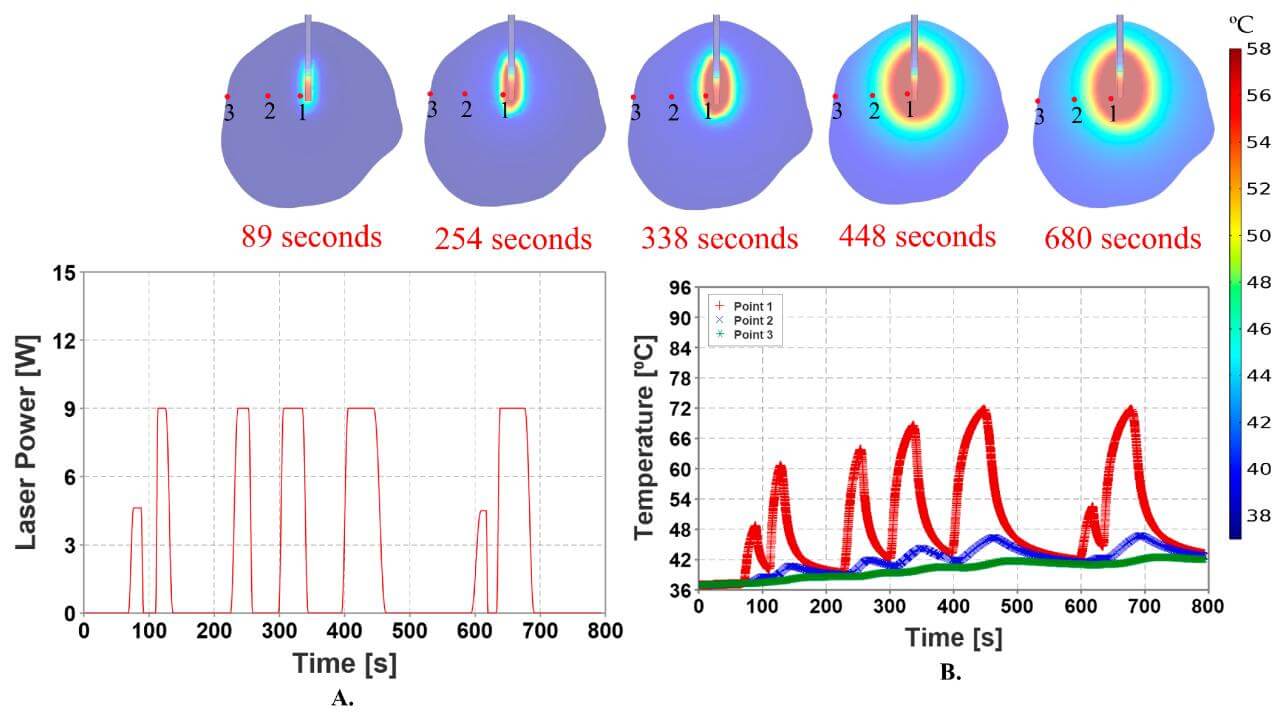
The main element is a 15W diode laser with a wavelength of 980 nm, which delivers thermal energy through a disposable fiber-optic probe. The probe is equipped with internal cooling with saline and is installed through a thin cooling catheter about 1 cm long and 1.65 mm in diameter, which allows the procedure to be performed percutaneously, through minimal access. The procedure is performed under constant MRI control.
Magnetic resonance imaging generates thermometric images that reflect the temperature distribution in the tissues in real time. Based on them, the computer system creates so-called ablation zone maps, which allow the doctor to accurately estimate the volume of the treated tissue.
When the catheter reaches the targeted area, the laser inside it starts releasing energy. Due to this, the targeted tissue is gradually warmed up and destroyed. The neurosurgeon monitors the process with the help of real-time MRI scans. Doctors control the intensity and duration of the laser work. Specific MRI thermographic images also show the temperature of nearby tissues – it is substantial for protecting vital regions of the brain.
Finally, when the active part of the work (thermal ablation) is completed, the surgeon gently removes the catheter and fixes the defects of the skull and the overlaying skin. The patient returns to his ward and stays under medical supervision for at least a day. Usually, the procedure is well-tolerated, so a patient can go home the next day.
The system software allows you to set temperature thresholds:
- Up to 90 °C near the probe tip to prevent overheating, carbonization, and tissue vaporization
- Up to 50 °C at the periphery of the treatment area to protect surrounding intact brain tissue [1]
Why Do Doctors Recommend the Visualase™ System Method for Brain Tumor Treatment?
The Visualase brain tumor treatment combines the advantages of precise neuronavigation and state-of-the-art technical advances, leading to the following benefits:
- Using the smallest ever neurosurgical catheter with a diameter of only 1.65 mm. The thin and flexible catheter moves through the nervous tissue easily and carefully, allowing a surgeon to work in the most hard-to-reach brain regions.
- Naturally, this leads to the next advantage – almost invisible skin incision and tiny hole in the skull bone. Skin incision usually requires only one suture to be completely fixed. The diameter of the skull perforation is only 3.2 mm.
- Using brain tumor laser surgery offers the opportunity to reduce or totally avoid hair removal. You will not be embarrassed by your appearance after the intervention, and you will choose headwear only if you like it. Later, the diminutive postoperative scar will be completely hidden by the hair.
- Visualase brain tumor treatment makes serious neurosurgical interventions much easier for the patients. There won’t be any blood loss, dizziness, or constant pain. You will be able to leave the hospital and go home the next day after the operation.
- Excellent visualization during the procedure gives doctors and patients the possibility of avoiding the removal of vast skull flaps. MRI substitutes direct field of view, giving even more detailed images.
- Postoperative irradiation of the head is not performed as well, because the tumor or the pathological loci are thoroughly destroyed. At the same time, neighboring tissues remain viable, as the process of ablative laser treatment is controlled perfectly [10].
When to Choose Visualase™ as a Treatment?
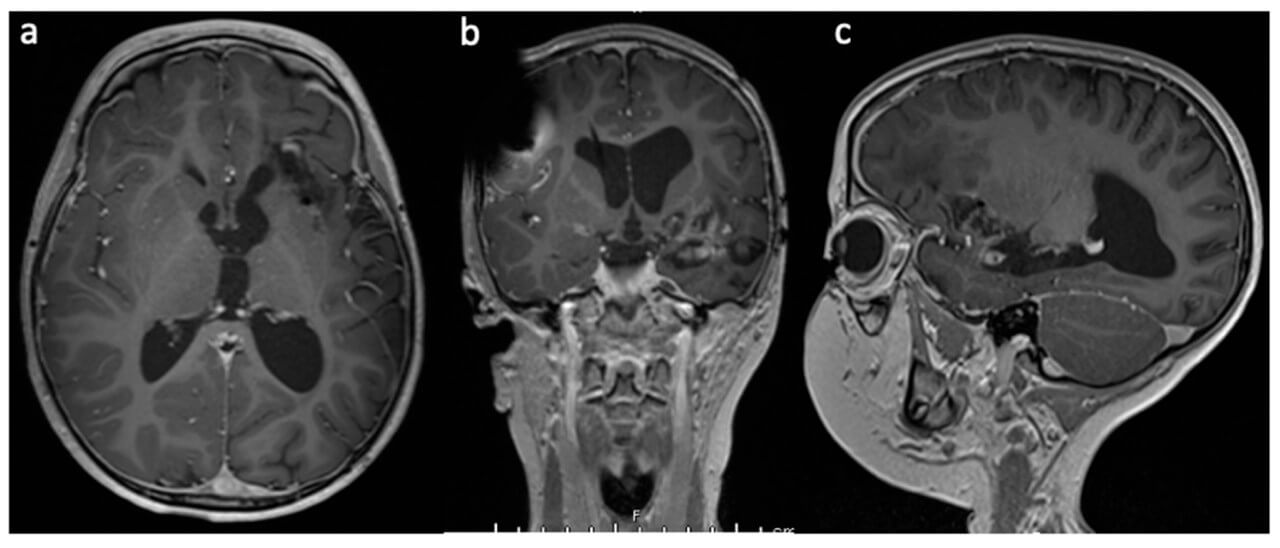
Visualase brain tumor treatment can destroy soft tissues with extremely high precision laser therapy. The possibility of performing controlled ablation makes this technique optimal in terms of removing or destroying the tiniest undesirable changes in the brain.
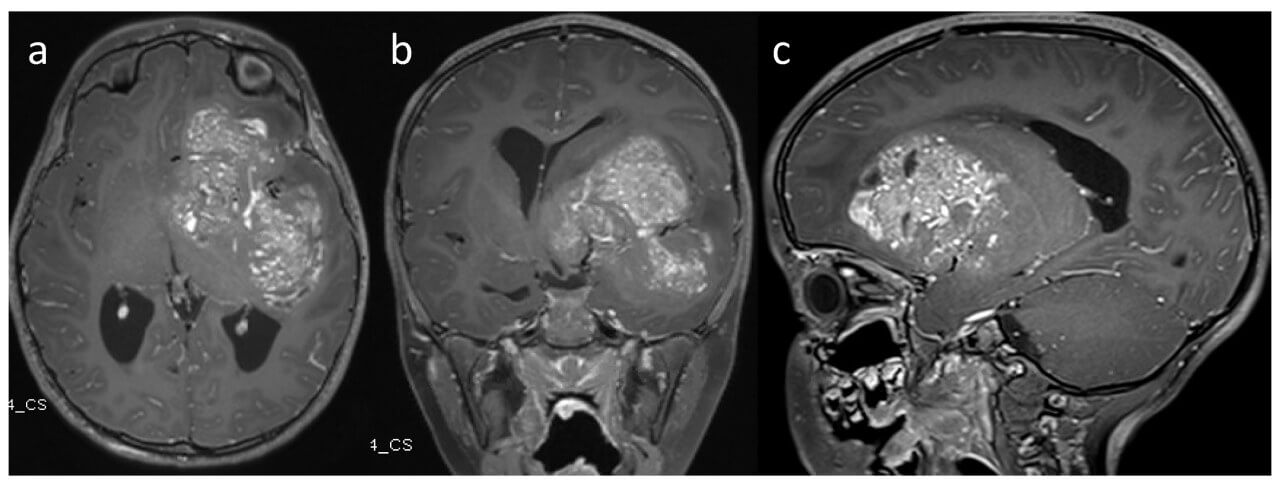
- Brain tumors, including gliomas, glioblastoma multiforme, anaplastic astrocytomas, radiation-resistant tumors, and inoperable tumors in the hard-to-reach regions, are perfect candidates for this technique. The small size of the neoplasm is not an obstacle, as well – preliminary stereotactic marking makes it clearly visible during the surgery [8].
- Epilepsy, namely, drug-resistant mesial temporal lobe epilepsy. This is the most widespread type of partial or localization-related epilepsy, detected in one-third of all patients. The constant epileptogenic locus in the brain tissue causes seizures, which can’t be alleviated with any number or type of anti-epileptic drugs. Directly destroying the pathologic locus is the only effective cure for such a disorder.
- Metastases of diverse tumors in the brain. Infection of the cerebral tissue with metastases of distant tumors is no less dangerous than the development of the primary neoplasm. MRI-guided laser therapy with the help of Visualase™ system offers the chance to destroy the smallest loci of the unwanted tissue [3].
- Radiation necrosis. It is a common complication in neuro-oncology practice. The overall incidence of its development after various types of radiotherapy is approximately 5-10%; however, in patients who have previously received stereotactic radiosurgery (SRS), the risk may increase to 50%, especially when doses in the range of 16-22 Gy are used [2].
In addition to neurosurgery, the technology of MRI-guided laser therapy can be used in other areas of medicine: cardiovascular surgery, ear-nose-throat surgery, head and neck surgery, gynecology, urology, and radiology. For example, the Visualase brain tumor treatment can be helpful in removing radiation necrosis foci formed due to prior radiation therapy.
Benefits of the Visualase™ System Over Traditional Treatments
Compared to traditional treatment methods, the brain tumor laser surgery offers a more gentle, controlled, and technologically precise approach. Below are the key advantages of this ablation laser surgery that determine its clinical value in modern neurosurgical and neurooncological practice.
Below is a table that systematizes the main advantages of the Visualase brain tumor treatment and provides brief explanations for each of them [9].
| Minimally invasive approach | The procedure is performed through a small percutaneous access, without craniotomy, which reduces surgical trauma and postoperative pain. |
| High precision tissue ablation | Provides targeted destruction of pathological tissue with maximum preservation of the surrounding functionally important brain structures. |
| Real-time MRI guidance and thermal control | Allows continuous control of the temperature and ablation limits in real time, increasing the safety of the intervention. |
| Reduced risk of neurological complications | Controlled temperature thresholds minimize the risk of damage to healthy brain tissue and the development of neurological deficits. |
| Shorter hospital stay and faster recovery | Most patients require a shorter hospitalization and return to daily activities faster compared to open surgery. |
| Option for hard-to-reach or inoperable lesions | Allows treatment of lesions that are difficult or dangerous for traditional surgical resection. |
| Alternative to repeat radiation therapy | Is an important option for patients with radiation necrosis or recurrences when re-irradiation is limited due to cumulative toxicity. |
| Effective for multiple indications | Used for brain tumors, metastases, drug-resistant epilepsy, and radiation necrosis. |
Limitations to the Visualase™ System
Despite its numerous advantages and wide clinical application, the Visualase brain tumor treatment has certain limitations that must be considered during patient selection and treatment planning. Understanding these limitations allows for a proper assessment of the technology’s role in the overall treatment strategy and ensures the safest and most predictable outcome.
- General contraindications to MRI.
Absolute contraindications include the presence of metallic implants in the body (e.g., coronary and peripheral artery stents, prosthetic heart valves, cochlear implants, and gastric reflux devices), implanted pacemakers or defibrillators, tattoos and cosmetics with particles of metals, claustrophobia, etc.
- Long-term intake of certain medications.
For example, some systemic anticancer drugs used to treat glioblastoma, including its recurrent forms, as well as metastatic malignant neoplasms. If treatment with the brain tumor laser surgery is planned, such drugs should be temporarily discontinued, as their action may increase the risk of complications and affect the safety of the procedure.
- Low availability of the equipment and qualified specialists.
An even more significant restriction is the limited number of hospitals that offer such cutting-edge, expensive equipment and properly trained neurosurgeons. Patients with brain lesions often need urgent help, but long waiting lists postpone the procedure for months.
In addition to the general limitations of the method, there are also contraindications that must be considered before planning treatment using the Visualase™ system, as they directly affect the safety and feasibility of the procedure.
Absolute contraindications to the use of the Visualase™ system are rare but include the lack of safe pathologic access to the lesion, severe immunosuppression, active local or systemic infection, uncorrected coagulation disorders, and the patient's refusal to provide informed consent for the intervention.
Relative contraindications include a significant lesion volume and proximity of the pathological focus to functionally critical structures, when it is impossible to provide adequate temperature control or effective protection of surrounding tissues during ablation [4].
Treating Brain Tumours Using the Visualase™ System
When we talk about the treatment of foreign patients, the first place belongs to Germany. Compared to other European countries, Germany has the largest number of clinics equipped with the Visualase brain tumor treatment. German neurosurgeons are qualified enough to perform hundreds of MRI-guided laser ablation brain procedures in patients with advanced brain cancer and epilepsy. For example, Beta Klinik in Bonn is famous all over the world due to its success in the treatment of epilepsy. Germany remains a leading destination for foreign patients due to its advanced medical infrastructure, broad availability of high-tech systems such as Visualase, and extensive experience of neurosurgical teams in treating complex brain disorders.
Learn more about brain cancer treatment
The increase in the incidence of brain metastases is directly related to the improvement in the effectiveness of modern oncological treatment of primary malignant tumors, which leads to an increase in the life expectancy of patients and, accordingly, to a greater number of secondary lesions of the central nervous system. In this context, thermal ablation is considered a safe and minimally invasive alternative to traditional treatment methods for carefully selected patients.
The Visualase™ system has proven effectiveness in the treatment of various types of tumors, including brain tumors. The use of MRI-guided laser ablation for brain tumor treatment with the Visualase system combines the advantages of this approach with high precision, controllability, and minimal invasiveness, which makes the method particularly valuable in complex clinical cases [5].
A Medical Journey: Every Step of the Way With Booking Health
Finding the best treatment strategy for your clinical situation is a challenging task. Being already exhausted from multiple treatment sessions, having consulted numerous specialists, and having tried various therapeutic interventions, you may be lost in all the information given by the doctors. In such a situation, it is easy to choose a first-hand option or to follow standardized therapeutic protocols with a long list of adverse effects instead of selecting highly specialized innovative treatment options.
To make an informed choice and get a personalized cancer management plan, which will be tailored to your specific clinical situation, consult medical experts at Booking Health. Being at the forefront of offering the latest medical innovations for already 12 years, Booking Health possesses solid expertise in creating complex cancer management programs in each case. As a reputable company, Booking Health offers personalized treatment with the Visualase™ Thermal Therapy System with direct clinic booking and full support at every stage, from organizational processes to assistance during treatment. We provide:
- Assessment and analysis of medical reports
- Development of the medical care program
- Selection of a suitable treatment location
- Preparation of medical documents and forwarding to a suitable clinic
- Preparatory consultations with clinicians for the development of medical care programs
- Expert advice during the hospital stay
- Follow-up care after the patient returns to their native country after completing the medical care program
- Taking care of formalities as part of the preparation for the medical care program
- Coordination and organization of the patient's stay in a foreign country
- Assistance with visas and tickets.
- A personal coordinator and interpreter with 24/7 support
- Transparent budgeting with no hidden costs
Health is an invaluable aspect of our lives. Delegating management of something so fragile yet precious should be done only to experts with proven experience and a reputation. Booking Health is a trustworthy partner who assists you on the way of pursuing stronger health and a better quality of life. Contact our medical consultant to learn more about the possibilities of personalized treatment with the Visualase™ Thermal Therapy with leading specialists in this field.
Cancer Treatment Abroad: Patient Experiences with Booking Health
Frequently Asked Questions About Visualase™ System
Send request for treatmentLaser ablation is a minimally invasive medical procedure in which controlled thermal energy is used to destroy abnormal tissue, with minimal impact on surrounding healthy structures.
The Visualase™ system is a state-of-the-art laser treatment technology that combines laser ablation with real-time MRI control, allowing the physician to precisely control the treatment area and temperature during the procedure.
The Visualase™ system is used to treat brain tumors, metastatic lesions, radiation necrosis, and drug-resistant epilepsy.
Data show that the Visualase™ system is a safe laser ablation method, as the procedure is performed under constant MRI control with automatic temperature limitation.
After laser treatment using the Visualase™ system, the recovery period is usually short, and most patients return to daily activities much faster than after open neurosurgery.
Choose treatment abroad and you will for sure get the best results!
Authors:
This article was edited by medical experts, board-certified doctors Dr. Nadezhda Ivanisova, and Dr. Daria Sukhoruchenko. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Our editorial policy, which details our commitment to accuracy and transparency, is available here. Click this link to review our policies.
Sources:
[1] R. Medvid, A. Ruiz, R.J. Komotar, J.R. Jagid, M.E. Ivan, R.M. Quencer and M.B. Desai. Current Applications of MRI-Guided Laser Interstitial Thermal Therapy in the Treatment of Brain Neoplasms and Epilepsy: A Radiologic and Neurosurgical Overview. American Journal of Neuroradiology November 2015, 36 (11) 1998-2006. 2021 Jan 14;7(1):3. doi: 10.3174/ajnr.A4362. [DOI]
[2] RF Barajas, JS Chang, PK Sneed et al. Distinguishing Recurrent Intra-Axial Metastatic Tumor from Radiation Necrosis Following Gamma Knife Radiosurgery Using Dynamic Susceptibility-Weighted Contrast-Enhanced Perfusion MR Imaging. AJNR Am J Neuroradiol. 2009 Feb;30(2):367–372. doi: 10.3174/ajnr.A1362. [DOI] [PMC free article]
[3] Ammar H Hawasli, Swapnil Bagade, Joshua S Shimony et al. Magnetic Resonance Imaging-Guided Focused Laser Interstitial Thermal Therapy for Intracranial Lesions: Single-Institution Series. Neurosurgery. 2013 Sep 19;73(6):1007–1017. doi: 10.1227/NEU.0000000000000144. [DOI] [PMC free article]
[4] Anthony Ryan, Caoimhe Byrne, Claudio Pusceddu et al. CIRSE Standards of Practice on Thermal Ablation of Bone Tumours. Cardiovasc Intervent Radiol. 2022 Mar 29;45(5):591–605. doi: 10.1007/s00270-022-03126-x. [DOI] [PMC free article]
[5] Clark Chen, Ian Lee, Claudio Tatsui et al. Laser interstitial thermotherapy (LITT) for the treatment of tumors of the brain and spine: a brief review. J Neurooncol. 2021 Feb 21;151(3):429–442. doi: 10.1007/s11060-020-03652-z. [DOI] [PMC free article]
[6] Yash Lad, Avesh Jangam, Hayden Carlton et al. Development of a Treatment Planning Framework for Laser Interstitial Thermal Therapy (LITT). Cancers 2023, 15(18), 4554. doi: 10.3390/cancers15184554. [DOI]
[7] Jason E. Chung, Omar Iqbal, Chandra Krishnan, Virginia Harrod et al. Neoadjuvant Chemotherapy with Laser Interstitial Thermal Therapy in Central Nervous System Neuroblastoma: Illustrative Case and Literature Review. Brain Sciences. Volume 13. Issue 11. doi: 10.3390/brainsci13111515. [DOI]
[8] Amanda Munoz-Casabella, Mohammed Ali Alvi, Masum Rahman et al. Laser Interstitial Thermal Therapy for Recurrent Glioblastoma: Pooled Analyses of Available Literature. World Neurosurg. 2021 Jun 1;153:91–97.e1. doi: 10.1016/j.wneu.2021.05.114. [DOI] [PMC free article]
[9] Rory Geoghegan, Le Zhang, Alan Priester et al. Interstitial Optical Monitoring of Focal Laser Ablation. IEEE Trans Biomed Eng. 2022 Jul 18;69(8):2545–2556. doi: 10.1109/TBME.2022.3150279. [DOI] [PMC free article]
[10] Seamus Bartlett, Tavarekere N Nagaraja, Brent Griffith et al. Persistent Peri-Ablation Blood-Brain Barrier Opening After Laser Interstitial Thermal Therapy for Brain Tumors. Cureus. 2023 Apr 10;15(4):e37397. doi: 10.7759/cureus.37397. [DOI] [PMC free article]
Read:
Comprehensive Guide to Brain Cancer Treatment: New and Standard Treatment Options
Brain cancer treatments in Germany
Treatment for Glioblastoma – Full Guide: New and Standard Treatments