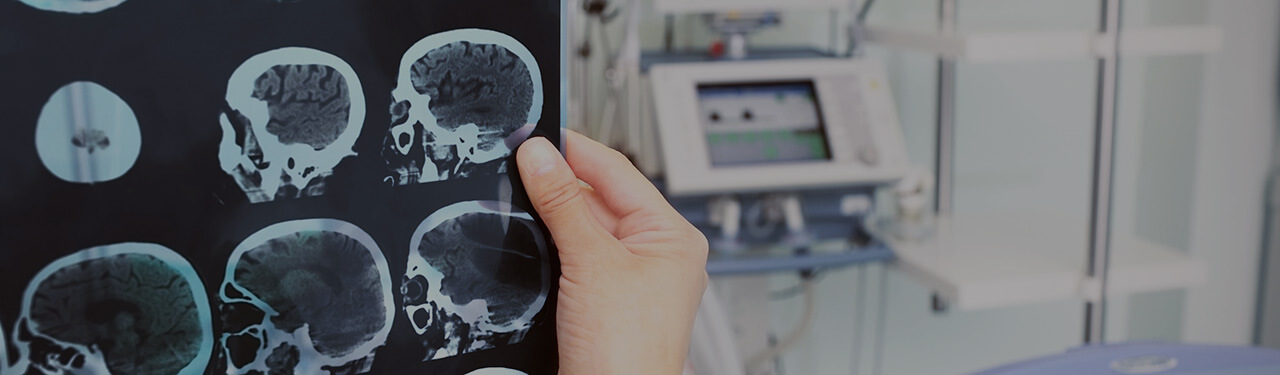
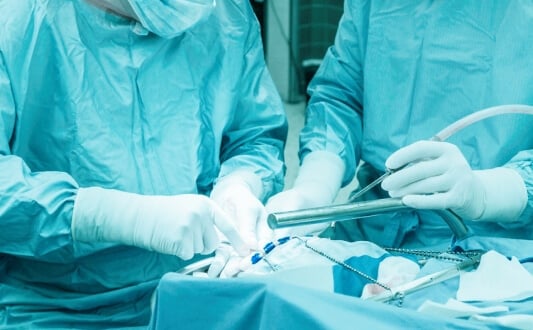
Robotic assisted technology is the latest breakthrough in neurosurgery. Robotic Surgery Assistance or ROSA as it is commonly called, is now being used at the University clinic in Frankfurt, Germany.
The advantages of using robotic surgery is minimally invasive, less pain, small incisions, reduced blood loss, quick recovery time, less time spent on recovery and healing which means a short hospital stay, low risk of infections and less scarring.
It must be noted that ROSA doesn't replace the surgeon, it merely takes over measurements, calculations and fine works that are necessary to perform such operations. In this way, miscalculations and other human errors are avoided. The robot assistant is used especially for target specific procedures, like brain tumors, epilepsy and Parkinson. It is also used to treat aneurysms and abscesses.
Content
How ROSA works in neurosurgery
In cases where surgeons need to access deeper regions of the brain, for instance to take biopsies or place electrodes, ROSA acts as an assistant. Using previously taken MRI scans, the device creates a 3D map of the brain, to determine the spot, as well as the angle, where the hole has to be drilled into the patient's skull, kind of like the way your GPS works. This kind of precision reduces the risk of damage to vessels and functional areas of the brain. Prior to ROSA neurosurgeons used stereotactical holders, a metal frame with two axises that look similar to a sextant. The head of the patient was fixed into the frame and scanned by a CT. The scans helped determine the localization of the procedure with coordinates, which had to be adjusted to the frame. Here there has always been a risk of transmission errors. ROSA now performs the same task but in a considerably less time.
In a recent case, the patient underwent a biopsy for a brain tumor. The patient first experienced epileptic seizures. After further tests, the doctors found a shadow on the scans, suspecting a tumor. The doctors now want to confirm the diagnosis and determine if the tumor is benign or malign. The patient receives general anaesthetic, which according to Dr. Freiman is not really necessary, because brain operations don’t hurt. During some brain operations, the patient has to be awake, for instance to monitor speech and motor functions.
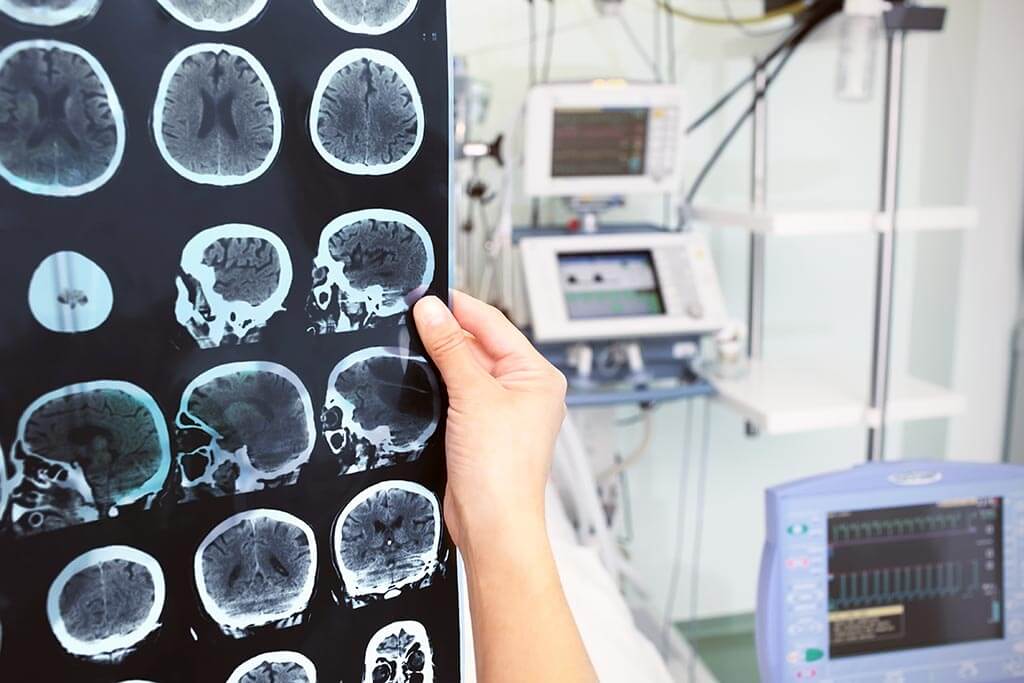
The patient's head is first fixed at three points in the metal frame of the device, so that the position of the head doesn’t move during the operation. In the case of a seizure, he or she must not be able to break free. After calibration, the robot arm scans the face of the patient. It orientates itself on certain landmarks, like the nose or the beginning and end of the eyelid. The first scan the device performs by itself, a second scan is performed by the surgeon, just to be safe. Then the computer calculates the optimal entry point while the robot arm indicates that spot with a laser on the skin. The doctor marks that spot with a pen. After this, doctors check to see if the robot arm and the instruments can actually reach the target, or the device has to be moved into another position. Then only will the machine and the patient be covered in sterile drapes and the operation spot will be disinfected. In addition, the patient receives IV fluids and antibiotics.
The robot arm places a guidance tube for the drill on the calculated spot. This guidance makes sure that the entry angle is correct. During the drilling, bone particles and blood are being sucked away. A bleeding could lead to permanent damage. As soon as the intended position is reached, which Dr. Freiman can see on ROSA's monitor, he takes several biopsies. The pathologist examines some of them immediately, inside the theatre under a microscope, to ensure that the actual tumor was hit. The rest will be analysed in the lab. In the past, doctors would have waited when they found a benign tumor. Today aggressive chemotherapy is administered sooner than later. This, however, doesn’t apply to brain tumors of children though, because the undeveloped brain is often damaged during chemo and radiation. So in these cases, biopsies are very important to determine if a treatment is actually necessary. ROSA offers a gentler procedure. It doesn’t require the mechanical pressure, which can deform the soft skull of children, as well as the radiation of a CT. The technique may soon be used for a new therapy of deep, inoperable tumors, this is currently in the clinical trial phase. Using a catheter, viruses and killer cells are placed inside the tumor to activate the immune system, which also attacks the tumor cells.
The epileptologists want to use ROSA to place electrodes for an EEG inside the brain. Many epileptic seizures originate in the depth of the brain. With a standard EEG those epicenters can’t be found.
Also Parkinson patients receive implanted electrodes to stimulate certain areas of the brain. This brings great relief to those who don’t respond to medication any more.
Frankfurt University Hospital bought the 500,000 Euro device from the French manufacturer Medtech. Making it the first University hospital to advance itself with robotic technology. The technology is also being used for research. ROSA is likely to be used for about 10 percent of the 2000 procedures by neurosurgeons. The investment pays off after about 3 years of use.
Neurosurgical treatment abroad with ROSA with Booking Health
If you need brain surgery, you should pay attention to hospitals in Germany. Both traditional and innovative robotic treatment methods are successfully used here.
The medical tourism operator Booking Health will organize your treatment in Germany. You can delegate all issues to Booking Health staff and focus on treatment.
Booking Health services include:
- Communication with the administration of a foreign clinic
- Translation of medical reports
- Making an appointment for the next dates
- Assistance in visa issuing
- Providing patients with medical insurance covering unforeseen medical expenses
- Accompaniment of interpreter
- Organization of a rehabilitation course after surgery
- Communication with the doctor after the completion of the treatment course
- Organizational services: booking airline tickets and hotels, transfer, etc.
With Booking Health you will save your time and money. We will take care of reducing the cost of treatment by excluding additional fees for foreign patients.
Choose treatment abroad and you will for sure get the best results!
Authors:
This article was edited by medical experts, board-certified doctors Dr. Nadezhda Ivanisova, and Dr. Bohdan Mykhalniuk. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Our editorial policy, which details our commitment to accuracy and transparency, is available here. Click this link to review our policies.
Sources:
Journal of Neurology, Neurosurgery and Psychiatry
Read:
Why Booking Health - questions and answers
How to make right decision when choosing the clinic and specialist
7 reasons to trust to the rating of clinics on the Booking Health portal