Since the 20th century, endoscopic technologies have gradually transformed neurosurgical practice, transforming from an auxiliary tool to one of the main methods of access to the deep parts of the brain and spinal cord. Their implementation allowed interventions to be performed in complex anatomical areas with minimal impact on healthy tissues and reduction of surgical trauma [1]. The parallel development of neuroanatomical and neurophysiological knowledge, as well as the improvement of optical systems, in particular the improvement of image clarity and the expansion of the viewing angle, have significantly expanded the diagnostic and surgical capabilities of neuroendoscopy, making it an integral part of modern minimally invasive neurosurgery.
What is?
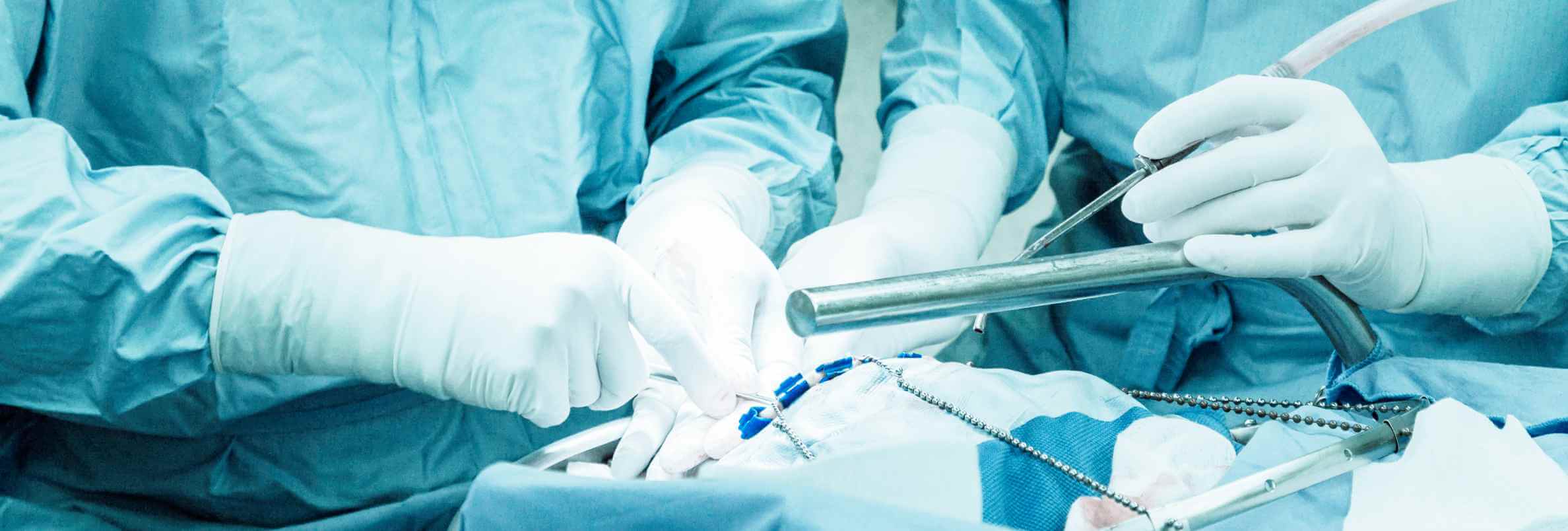
Endoscopic brain surgery is a modern direction of minimally invasive neurosurgery based on the use of optical endoscopic systems in combination with specialized microtools. Operative interventions are performed through minimal accesses under direct visual control, which allows reaching the pathological focus without the need for a wide tissue dissection. This approach is especially valuable when working in deep or anatomically complex areas, where traditional methods can be accompanied by greater traumatization.
The widespread introduction of neuroendoscopy became possible thanks to its ability to maximally preserve the intactness of healthy structures, reduce the intraoperative load on the body and reduce the frequency of postoperative complications. The combination of high-quality endoscopic imaging with modern microsurgical instruments opens up the possibility of performing complex manipulations through extremely limited accesses, which is of particular importance in brain and spinal cord operations [2].
During the intervention, the surgeon constantly focuses on an enlarged high-definition image, which is broadcast to the monitor in real time, which ensures the accuracy of each movement. The use of an endoscope allows penetration into the subarachnoid space, ventricular system, brain parenchyma and spinal canal, expanding the possibilities of access to various pathological processes. Due to this, the range of neurosurgical interventions that can be performed with minimal impact on the surrounding tissues is significantly increased, maintaining a high level of safety and accuracy.
It is also important to say that regular follow-up examinations are extremely important for early detection of brain tumor recurrence after surgery and timely correction of subsequent treatment tactics.
When Is Endoscopic Brain Surgery Used?
Today, endoscopic brain tumor surgery is used for intracranial tumors, obstructive hydrocephalus, various intraventricular lesions, hypothalamic hamartomas, craniosynostosis, tumors of the base of the skull, as well as for spinal pathologies [2].
In the surgical treatment of intracranial tumors, endoscopic technologies are widely applied to perform diagnostic biopsies, simultaneously ensuring the outflow of cerebrospinal fluid, as well as for intraoperative evaluation of residual tumor tissue after microsurgical removal of the neoplasm.
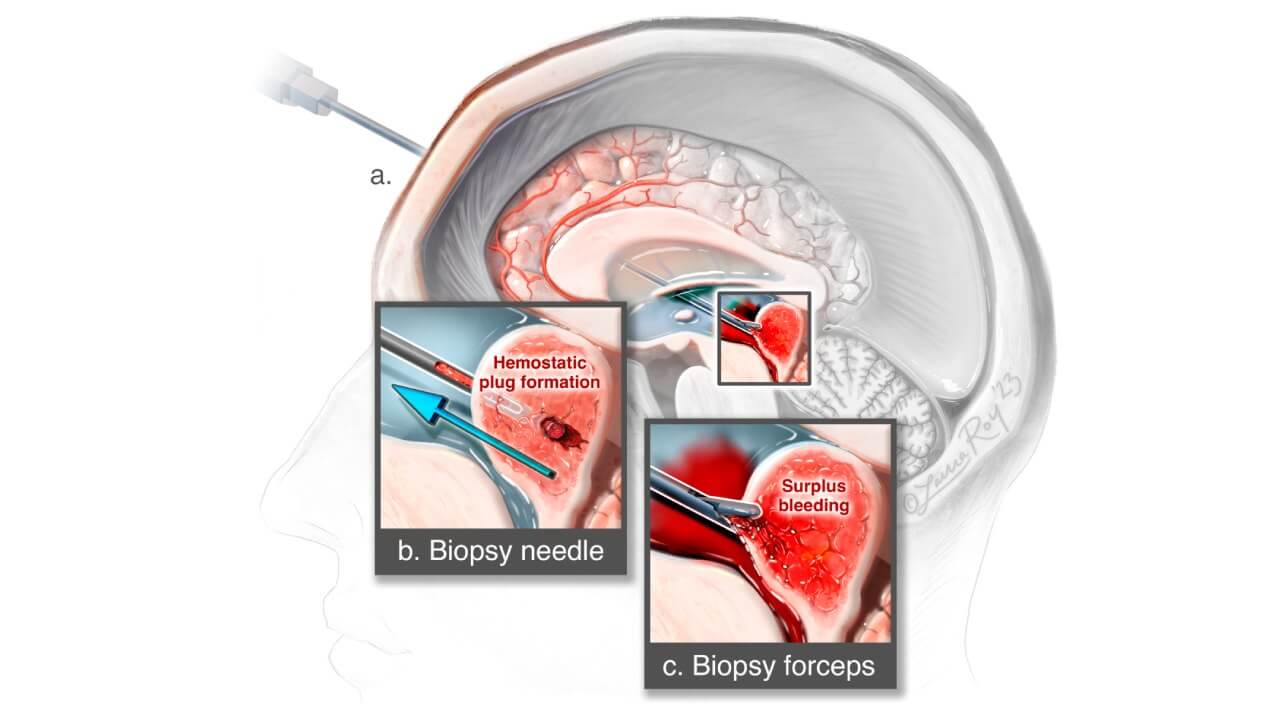
During transnasal and separate transcranial interventions, the endoscope can act mainly as an imaging system, while active surgical manipulations are carried out by instruments carried out in parallel with it, and not through its working channel. This format of work makes it possible to use tools of a larger diameter, which provide faster resection of tumor tissue and more reliable hemostasis. In many cases, this is technically more effective than applying tools limited by the narrow lumen of the endoscope.
At the same time, such a technique has not become universal for brain tumor surgery, in particular for intraventricular and periventricular tumors. The main restraining factor remains the risk of traumatization of critical structures of main vessels, conductive pathways and cranial nerves, as a result of repeated insertion of instruments into the deep parts of the brain outside a visually stable channel. In order to improve safety, the use of a two-endoscopic technique is described, where one endoscope provides continuous visualization of the operative field and the second is used to perform direct manipulations during the removal of tumors or tumor-like cysts in the intracranial space.
Despite significant progress in the development of optics and tools, complete endoscopic resection of most intracranial tumors continues to be a difficult task. Mild neoplasms of small size (up to 2 cm), completely localized in the ventricular system, with low or moderate vascularization, present hydrocephalus and available direct surgical trajectory are considered the most favorable for total endoscopic removal [3]. It is the combination of these factors that determines the technical feasibility and safety of such an approach.
How Does Endoscopic Brain Surgery Work?
Endoscopic brain surgery is a minimally invasive method of treatment, the main advantage of which is the absence of the need to perform a craniotomy. Instead of large surgical incisions, access to the affected areas is through natural anatomical pathways, most often through the nose (endonasal access) or through small milling holes in the skull. This approach makes it possible to significantly reduce trauma to healthy tissues.
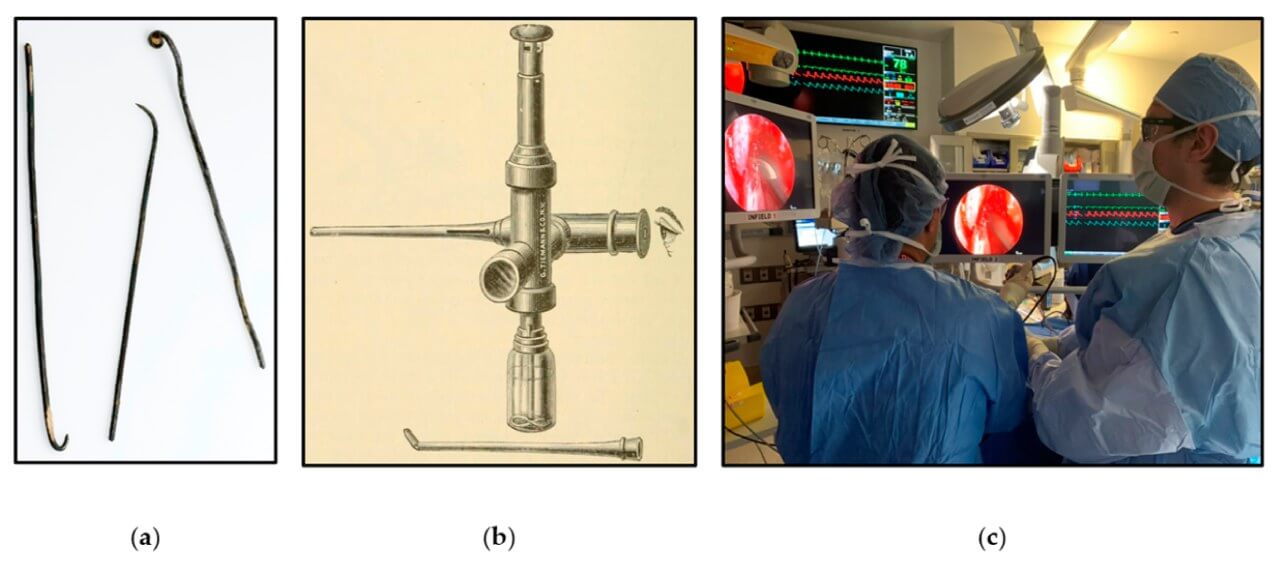
During brain tumor surgery, the surgeon gradually forms minimal access and introduces a thin endoscope equipped with a high-definition optical system and an intense light source. With the endonasal approach, the instrument is passed through the nasal passages and sinuses to the area of the base of the skull, which allows doctors to reach the pathological focus without external incisions. An enlarged image of the operating field is broadcast to the screen in real time, providing accurate orientation in anatomically complex areas.
At the same time as the endoscope, long microsurgical instruments are used, with the help of which tumor tissue is resected, biopsies are performed, or cerebrospinal fluid circulation is restored, in particular in obstructive hydrocephalus. Modern neuroendoscopic operations are complemented by 3D imaging, neuronavigation systems and high-precision aspiration-cutting devices, which allows to increase control over manipulations, minimize trauma to surrounding structures and ensure a greater level of safety during brain tumor surgery.
Once the surgical goal is achieved, the endoscope and instruments are removed. In the case of endonasal access, the intervention area is carefully closed, sometimes using a tissue graft, to prevent cerebrospinal fluid leakage and ensure proper healing.
Benefits of Endoscopic Brain Surgery
The main advantages of endoscopy procedure implementation in the field of brain tumor surgery are obvious:
- There are no large incisions, tissues damage is significantly reduced
- No need for craniotomy
- Endoscopy procedure helps to reach areas of the brain previously inaccessible for surgical interventions
- Low risk of intraoperative complications, including lethal ones
- Low risk of postoperative complications, such as bleeding or infection
- Reduced risk of damage to the blood vessels or peripheral nerves
- Accelerated rehabilitation period
- Less postoperative pain
- Good aesthetic effects as there are no large scars after brain tumor endoscopic surgery
Neuroendoscopy has a number of technological and clinical advantages that determine its role in modern minimally invasive neurosurgery. Optical systems provide powerful focused illumination and a clear magnified image of the operating field, allowing detailed evaluation of anatomical structures even in deeply located areas. High controllability of tools and the possibility of accurate visual control significantly increase the safety of manipulations, especially when working in a limited space. Passing through minimal accesses makes it possible to reach the pathological focus without a wide dissection of tissues and provides high-quality visualization of deep structures with maximum detail.
In transcranial neuroendoscopy, an additional advantage is the use of lenses with different viewing angles, which allows to look behind anatomical barriers and expand the visible operational field. As a result, the surgeon receives an inspection of the site, which may be several times the size of the primary access, while maintaining a minimum level of trauma [4]. Endoscopic brain surgery recovery with this approach is usually faster, but its duration is determined individually and depends on the amount of resection, tumor localization and patient compliance with recommendations in the rehabilitation period.
Risks/Limitations of Endoscopic Brain Surgery
Endoscopic brain surgery, in particular in the treatment of skull base tumors, provides significant advantages of a minimally invasive approach, but is accompanied by several specific risks. Among the most significant complications are the leakage of cerebrospinal fluid (CSF), damage to cranial nerves, and infectious processes. Key limitations of the method include limited instrument maneuverability, possible pituitary function disorders, and, in some cases, vascular injuries. Although endoscopic interventions are considered safer compared to traditional open approaches, they are still associated with potential complications, including pituitary insufficiency (up to 14.1% in some studies), visual impairment, and the need for complex reconstructive steps [5].
Main risks of endoscopic brain surgery
- Cerebrospinal fluid (CSF) leak. It is one of the most common complications, but in most cases, it can be controlled and effectively eliminated by modern reconstructive methods.
- Endocrine changes. Temporary or, much less often, persistent disorders of the hormonal balance can occur due to the proximity of the pituitary gland to the intervention area.
- Impaired vision or cranial nerve function. They can be temporary in nature and depend on the localization of the tumor.
- Vascular complications. They are rare, but require special attention during an endoscopic brain surgery procedure.
- Infectious complications. Including meningitis or local inflammatory processes, more often associated with cerebrospinal fluid [6].
Limitations of Endoscopic Methods
Despite the significant advantages, endoscopic methods have certain limitations that are important to consider when choosing treatment tactics.
- Anatomical features. Narrow nasal passages or complex anatomy can limit the maneuverability of instruments.
- Tumor size and spread. Large neoplasms or tumors with significant lateral spread are not always subject to purely endoscopic treatment.
- Visualization features. In complex cases, particularly bleeding, orientation may be technically more difficult.
- Experience of the surgical team. Endoscopic neurosurgery requires a high level of training and specialization [7].
Endoscopic Brain Surgery Cost
Endoscopic brain surgery cost depends on the complexity of the operation, the location of the lesion, the need for reconstruction, the duration of hospitalization, and the experience of the neurosurgical team. Prices also vary significantly between countries due to health system specificities and the level of medical costs. Below is a comparative table of the estimated cost of treatment in Germany, the USA, Great Britain, and Australia.
| Treatment type | Germany | USA | Great Britain | Australia |
|---|---|---|---|---|
| Surgery | €25,000 – €45,000 | €65,000 – €85,000 | €35,000 – €55,000 | €15,000 – €30,000 |
Alternative Treatments for Brain Tumors
In addition to endoscopic surgery, other methods are used for the treatment of brain tumors, the choice of which depends on the type of tumor, its location, the stage of the disease, and the general condition of the patient.
Alternative brain tumor treatment includes both classical and high-tech approaches, the choice of which is determined by the morphology of the tumor, its size, localization and biological behavior. Open neurosurgery remains the basic method in cases of large, infiltrative or anatomically complex neoplasms, when extensive examination and radical removal of tissue is necessary. Radiation therapy, including high-precision techniques such as proton-beam irradiation, allows for targeted effects on tumor cells, minimizing stress on adjacent healthy structures. Chemotherapy and combined chemo-radiation treatments are used as stand-alone or adjuvant methods, especially in malignant gliomas and metastatic lesions.
A separate direction is modern immunotherapeutic technologies, in particular dendritic cell therapy, the purpose of which is to stimulate the body's own immune response to recognize and destroy tumor cells. Such approaches are at the stage of active development and are increasingly integrated into complex treatment protocols. The essence of this method is to create an individual vaccine based on dendritic cells, which "teach" the immune system to respond to tumor antigens. This strategy shows the most promising results in glioblastoma, especially in combination with surgical removal of the tumor. The combination of radical resection and immunostimulation potentially reduces the risk of recurrence and improves long-term treatment outcomes.
The optimal strategy is always determined individually by a multidisciplinary team, including neurosurgeons, oncologists, radiologists and other specialists. It is the systematic approach and access to advanced technologies that make Germany one of the leading centers for the treatment of brain tumors. High standards of care, modern equipment and strict adherence to clinical protocols provide patients with individualized, safe and scientifically based treatment.
A Medical Journey: Every Step of the Way With Booking Health
Finding the best treatment strategy for your clinical situation is a challenging task. Being already exhausted from multiple treatment sessions, having consulted numerous specialists, and having tried various therapeutic interventions, you may be lost in all the information given by the doctors. In such a situation, it is easy to choose a first-hand option or to follow standardized therapeutic protocols with a long list of adverse effects instead of selecting highly specialized innovative treatment options.
To make an informed choice and get a personalized cancer management plan, which will be tailored to your specific clinical situation, consult medical experts at Booking Health. Being at the forefront of offering the latest medical innovations for already 12 years, Booking Health possesses solid expertise in creating complex cancer management programs in each case. As a reputable company, Booking Health offers personalized endoscopic brain cancer treatment plans with direct clinic booking and full support at every stage, from organizational processes to assistance during treatment. We provide:
- Assessment and analysis of medical reports
- Development of the medical care program
- Selection of a suitable treatment location
- Preparation of medical documents and forwarding to a suitable clinic
- Preparatory consultations with clinicians for the development of medical care programs
- Expert advice during the hospital stay
- Follow-up care after the patient returns to their native country after completing the medical care program
- Taking care of formalities as part of the preparation for the medical care program
- Coordination and organization of the patient's stay in a foreign country
- Assistance with visas and tickets.
- A personal coordinator and interpreter with 24/7 support
- Transparent budgeting with no hidden costs
Health is an invaluable aspect of our lives. Delegating management of something so fragile yet precious should be done only to experts with proven experience and a reputation. Booking Health is a trustworthy partner who assists you on the way of pursuing stronger health and a better quality of life. Contact our medical consultant to learn more about the possibilities of personalized treatment with innovative methods for brain cancer with leading specialists in this field.
Every Patient Has a Story: Booking Health Treatment Journeys that Inspire
Frequently Asked Questions About Endoscopic Brain Surgery
Send request for treatmentThe rate of tumor re-growth after surgery depends on its type, degree of malignancy, and completeness of removal. In some cases, brain tumor recurrence may occur after months or years, while in aggressive forms, the risk of recurrence is higher and requires additional treatments and regular follow-up.
The duration of the operation depends on the complexity of the case, the location of the tumor, and the chosen surgical approach. On average, brain surgery time can be between 2 and 6 hours; however, complex interventions can take longer, especially if reconstruction or intraoperative monitoring is required.
Endoscopic brain surgery is considered less traumatic compared to open surgery, but may be accompanied by risks such as cerebrospinal fluid leakage, temporary neurological disorders, or infectious complications. Proper patient selection, advanced equipment, and careful postoperative control play a key role in reducing the likelihood of complications and have a positive effect on the brain tumor surgery success rate.
Recovery after endoscopic surgery is usually faster than after open neurosurgery. Most patients return to daily activity within a few weeks, while full recovery may take several months, depending on the extent of the intervention and individual characteristics of the body.
Choose treatment abroad and you will for sure get the best results!
Authors:
This article was edited by medical experts, board-certified doctors Dr. Nadezhda Ivanisova, and Dr. Daria Sukhoruchenko. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Our editorial policy, which details our commitment to accuracy and transparency, is available here. Click this link to review our policies.
Sources:
[1] Aneela Darbar, Fatima Mustansir , Ummey Hani, Mir Ibrahim Sajid. A Review of Common Endoscopic Intracranial Approaches. Asian J Neurosurg. 2020 Aug 28;15(3):471–478. doi: 10.4103/ajns.AJNS_367_19. [DOI] [PMC free article]
[2] Kyu Won Shim, Eun Kyung Park, Dong-Seok Kim, Joong-Uhn Choi. Neuroendoscopy: Current and Future Perspectives. J Korean Neurosurg Soc. 2017 May 1;60(3):322–326. doi: 10.3340/jkns.2017.0202.006. [DOI] [PMC free article]
[3] Aaron Mohanty. The current role of endoscopes in intracranial tumor surgery. J Neurosci Rural Pract. 2013 Jan-Mar;4(1):3–5. doi: 10.4103/0976-3147.105599. [DOI] [PMC free article]
[4] Long Zhou, Xiongfei Jing, Chang Wang et al. Clinical application of transcranial neuroendoscopy combined with supraorbital keyhole approach in minimally invasive surgery of the anterior skull base. Sci Rep. 2024 Jun 27;14:14886. doi: 10.1038/s41598-024-65758-y. [DOI] [PMC free article]
[5] Mohamad Namvar, Arad Iranmehr, Mohamad Reza Fathi et al. Complications in Endoscopic Endonasal Pituitary Adenoma Surgery: An Institution Experience in 310 Patients. J Neurol Surg B Skull Base. 2022 Jul 5;84(3):255–265. doi: 10.1055/a-1838-5897. [DOI] [PMC free article]
[6] Rudrashish Haldar, Sukhminder Jit Singh Bajwa. Potential Neuroendoscopic Complications: An Anesthesiologist's Perspective. Asian J Neurosurg. 2019 Jul-Sep;14(3):621–625. doi: 10.4103/ajns.AJNS_37_17. [DOI] [PMC free article]
[7] Matthew R Naunheim, Ahmad R Sedaghat, Derrick T Lin et al. Immediate and Delayed Complications Following Endoscopic Skull Base Surgery. J Neurol Surg B Skull Base. 2015 May 15;76(5):390–396. doi: 10.1055/s-0035-1549308. [DOI] [PMC free article]
[8] Bojan Jelaca, Nebojsa Lasica, Milica Gledja et al. Endoscopic Biopsy of Intra- and Paraventricular Brain Lesions: Practical Advantages and Clinical Experience. Medicina 2026, 62(2), 260. doi: 10.3390/medicina62020260. [DOI]
[9] Luisa F. Figueredo, Andrea L. Martínez, Paola Suarez-Meade et al. Current Role of Endoscopic Endonasal Approach for Craniopharyngiomas: A 10-Year Systematic Review and Meta-Analysis Comparison with the Open Transcranial Approach. Brain Sci. 2023, 13(6), 842. doi: 10.3390/brainsci13060842. [DOI]
[10] Jakub Jarmula, Erion Junior de Andrade, Varun R. Kshettry and Pablo F. Recinos. The Current State of Visualization Techniques in Endoscopic Skull Base Surgery. Brain Sci. 2022, 12(10), 1337. doi: 10.3390/brainsci12101337. [DOI]
Read:
Innovative Glioblastoma Immunotherapy Treatment