Globally, lung cancer remains the leading cause of cancer mortality, with about 2 million new diagnoses and 1.8 million deaths annually. Neoplasms of the lungs are the second most common cancer diagnosis among men and women worldwide (after prostate and breast cancer, respectively). [1]
This novel approach gained widespread popularity in lung cancer, particularly in cases of non-small cell lung cancer (NSCLC) and pleural mesothelioma. Cancer immunotherapy was granted the Nobel Prize in Medicine in 2011 and 2018. Immunotherapy of lung cancer is successfully applied in Germany for cancer of different stages. Doctors help the immune system of the patient to recognize and destroy cancer cells and metastases. In advanced lung cancer, immunotherapy is the only possible treatment, whereas in the earlier stages, doctors can use it with other treatments such as radiation therapy, chemotherapy, or surgery. German oncologists tailor the treatment of cancer by relying on their genetic and molecular properties of individual tumors.
When is Immunotherapy Administered for Lung Cancer?
A potent therapeutic option for patients with advanced, recurring, or early-stage lung cancer is immunotherapy. Modern international and German protocols recommend earlier administration, as this improves overall survival and prolongs relapse-free periods by strengthening the patient’s immune response against tumor cells.
Immunotherapy is now indicated in the following cases:
- Neoadjuvant therapy before surgery in people with large primary tumors. This approach helps shrink the neoplasm, making it easier for surgeons to remove affected tissue while protecting normal cells.
- Adjuvant therapy after surgery is aimed at lowering the risk of recurrence. Eligible lung cancer patients are usually those with lymph node involvement or extensive primary tumors.
- Metastatic or advanced lung cancer, where immune checkpoint inhibitors and other drugs are often a standard cancer treatment option.
- Maintenance therapy in combination with chemotherapy, designed to delay disease progression and extend disease control.
In addition, innovative drugs and combinations with other lung cancer treatments are being tested in many ongoing clinical trials, including cancer vaccines and novel forms of adoptive cell therapy. German scientists are also exploring ways to optimize cell activation and enhance the role of CAR T-cells and activated T-cells in targeting tumors.
German centers are also at the forefront with modern treatment of lung cancer, which incorporates radiation therapy, hyperthermia, supportive care, and the use of infusion based immunotherapy treatment of lung cancer. The aim of this strategy is to alleviate pain, improve the quality of life, and boost the immune system to combat cancer more effectively.
How is immunotherapy different from other lung cancer treatments?
Immunotherapy lung cancer protocols differ from other lung cancer treatments because they do not directly destroy the tumor. Instead, they stimulate the body’s own immune system to recognize and attack cancer cells, including circulating lung cancer cells and hidden tumor cells. In contrast, chemotherapy or radiation therapy act by directly damaging DNA or cell structures to destroy cancer cells, which can also affect surrounding normal cells.
The primary goal of the immunotherapy of lung cancer is to strengthen the immune response of the body and to allow immune cells, especially T-cells, to identify and control malignant cells. This approach can provide lung cancer patients with years of relapse prevention and postponement of the development of the disease.
Immunotherapy offers systemic control and can be used in conjunction with targeted therapy, chemotherapy, and checkpoint-based treatments like immune checkpoint inhibitors. Treatment increases the survival of activated T-cells.
Side effects represent yet another important difference. Immunotherapy treatment rarely results in severe toxicity, in contrast to chemotherapy or radiation therapy. The majority of people only have minor side effects, including rash, diarrhea, or exhaustion. Overall, this type of cancer treatment is safer than traditional approaches and often well-tolerated.
| Toxicity | Patient Eligibility Criteria | Duration of treatment effect | |
|---|---|---|---|
| Dendritic cell vaccines | Very low (about 1%) | Suitable for both early and advanced stages, can be used post-surgery or as a standalone therapy | Reliable long-term result, long-lasting remission, lifelong immune memory |
| Chemotherapy | High (65-80%) | Adequate organ function (especially liver and kidneys), no severe comorbidities | Short-term effect, limited to the course of treatment |
| Targeted therapy | Low (15-20%) | Must have specific genetic mutations (like EGFR, ALK, or ROS1) | The effect is quite long-lasting in the presence of specific mutations in the tumor |
*Booking Health data. Success rates vary depending on cancer type, stage, and individual patient factors.
What are the Types of Lung Cancer Immunotherapy?
Lung cancer immunotherapy encompasses a number of novel medication classes that boost the immune system and enhance its capacity to fight cancer in various ways. While some preparations serve as ready-made compounds that replace specific immune activities, others trigger T-cells, reveal tumors, and teach immune cells to more effectively identify and attack cancer cells without endangering nearby normal cells. By doing this, the body can eradicate cancer cells while preserving healthy tissues.
The main types of cancer immunotherapy applied in lung cancer treatment include:
- Dendritic cell-based cancer vaccines
- Monoclonal antibodies
- Immune checkpoint inhibitors
- Adoptive cell therapy
Depending on the stage and form of the disease—whether non-small cell lung cancer or small cell lung cancer—oncologists may recommend a single drug or a combination with other lung cancer treatments such as chemotherapy, targeted therapy, or radiation therapy. The selection is always tailored to maximize efficacy and extend survival for lung cancer patients.
Dendritic Cell-based Vaccines for Lung Cancer
Non-small cell lung cancer at both early and advanced lung cancer stages can be treated with dendritic cell-based cancer vaccines after partial or complete surgical tumor removal (adjuvant therapy). Vaccination has shown effectiveness in patients with glandular and squamous cell carcinoma, with clinical studies reporting an increase in 5-year survival by 65%. This therapy strengthens the immune response, helping immune cells and T-cells to attack cancer cells and eliminate cancer cells that may remain after surgery.
In most cases, the lung tumor is removed during surgery, and blood monocytes serve as material for creating a personalized vaccine. The final product is injected subcutaneously, is well-tolerated, and typically causes no significant side effects. Even a single injection can generate a stable antitumor immune response, particularly valuable for early-stage lung cancer patients. It not only targets residual tumor cells and micrometastases but also creates immunological memory, helping prevent recurrence.
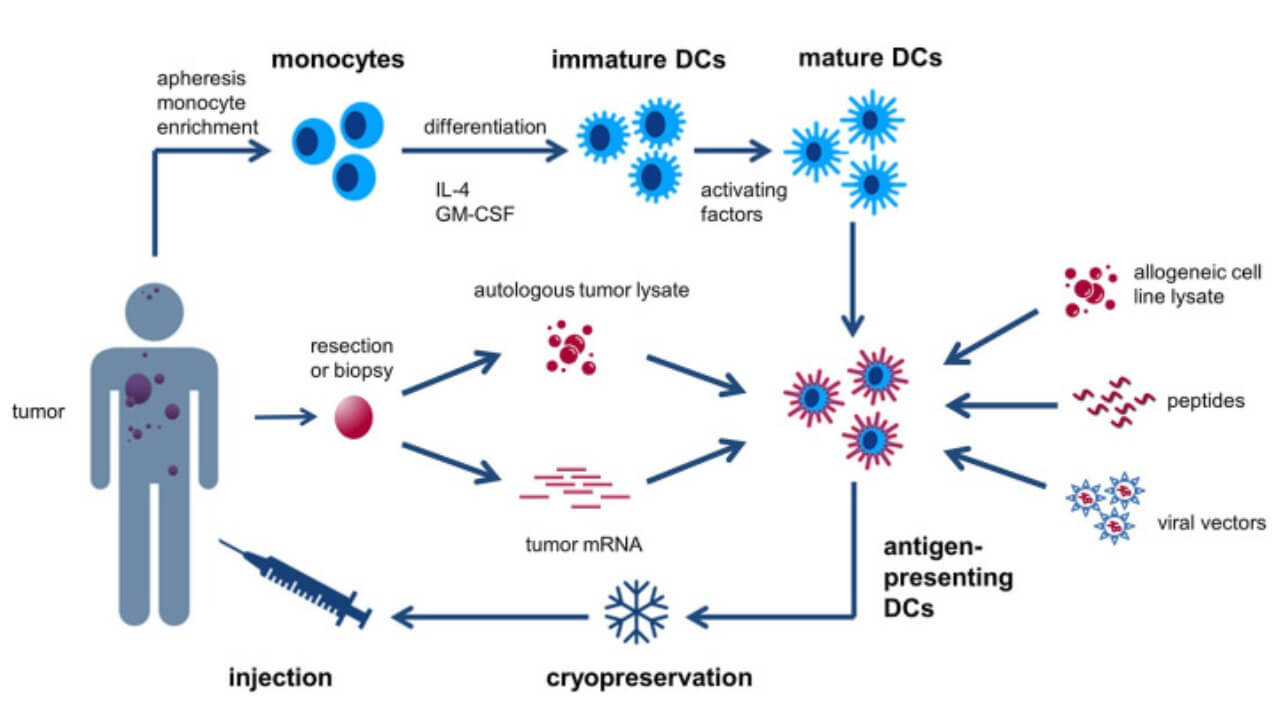
For advanced lung cancer, promising results have been observed when dendritic cell vaccines are combined with the Newcastle disease virus and γδ T-cell-based therapy. This combination enhances cell activation, reinforces the immune system, and demonstrates high success rates in clinical studies for patients with stage 3 and 4 disease.
An Expert Perspective on Dendritic Cell Therapy for Lung Cancer
We spoke with Professor Frank Gansauge, a renowned specialist with more than 20 years of expertise in lung cancer immunotherapy, to gain a deeper understanding of this innovative strategy. He is one of the pioneers in dendritic cell-based cancer vaccines and has helped come up with modern lung cancer treatment regimens, offering hope to lung cancer patients at any stage, including in advanced lung cancer.
Combining DC vaccines with other methods used to treat lung cancer, Professor Gansauge's clinical experience demonstrates that it is possible to use these vaccines as part of comprehensive treatment strategies that enhance the immune system capacity to attack the tumor cells. One of his areas of specialization is the development of innovative therapies to treat individuals at stage 4, wherein the use of conventional medicines yields patchy outcomes.
His practice in the context of immunotherapy treatment is centrally based on individual care, a strategy that prescribes the individual treatment plan to suit the specific case of the patient without negatively affecting their quality of life. Since these vaccines enable the activation of T-cells and other immune cells to annihilate cancer cells effectively, they may be incorporated into a composite therapy or may be administered alone of other therapies.
In the interview that follows, Professor Gansauge speaks of patient screening, treatment plans, and the promising future of dendritic cell therapy in the treatment of cancer. Professor Gansauge is also providing useful tips to cancer patients and healthcare practitioners who are considering cancer immunotherapy.
"Every Patient Deserves Individual Approach": Interview with Renowned German Immunologist Prof. Gansauge
Monoclonal Antibodies for Lung Cancer
Protein molecules known as monoclonal antibodies attach themselves specifically to particular tumor cells or distinctive antigens on their surface. These drugs can also target molecules on tumor blood vessels, helping to attack cancer cells and disrupt their growth.
Synthesized in the laboratory, monoclonal antibody preparations are tailored for each target. For lung cancer treatment, doctors often use agents that suppress vascular endothelial growth factor (VEGF), preventing new blood vessel formation and effectively starving tumor cells of oxygen and nutrients. This approach contributes to the broader strategy of treating lung cancer by reinforcing the immune system and enhancing the immune response.
Some immune checkpoint inhibitors are also monoclonal antibodies. While they belong to the same protein-based family, their mechanisms allow activated T-cells to attack cancer cells more effectively, making them a critical part of cancer immunotherapy. Research continues in ongoing clinical trials to discover new targets and expand the applications of these innovative agents for advanced lung cancer.
Immune Checkpoint Inhibitors for Lung Cancer
Every day, millions of cancer cells can be eliminated by the human immune system. Malignant tumors, on the other hand, can avoid detection by passing for normal cells. Immune checkpoint inhibitors successfully reactivate the body's immune response against covert tumor cells by restoring T-cells and other immune cells' capacity to attack cancer cells.
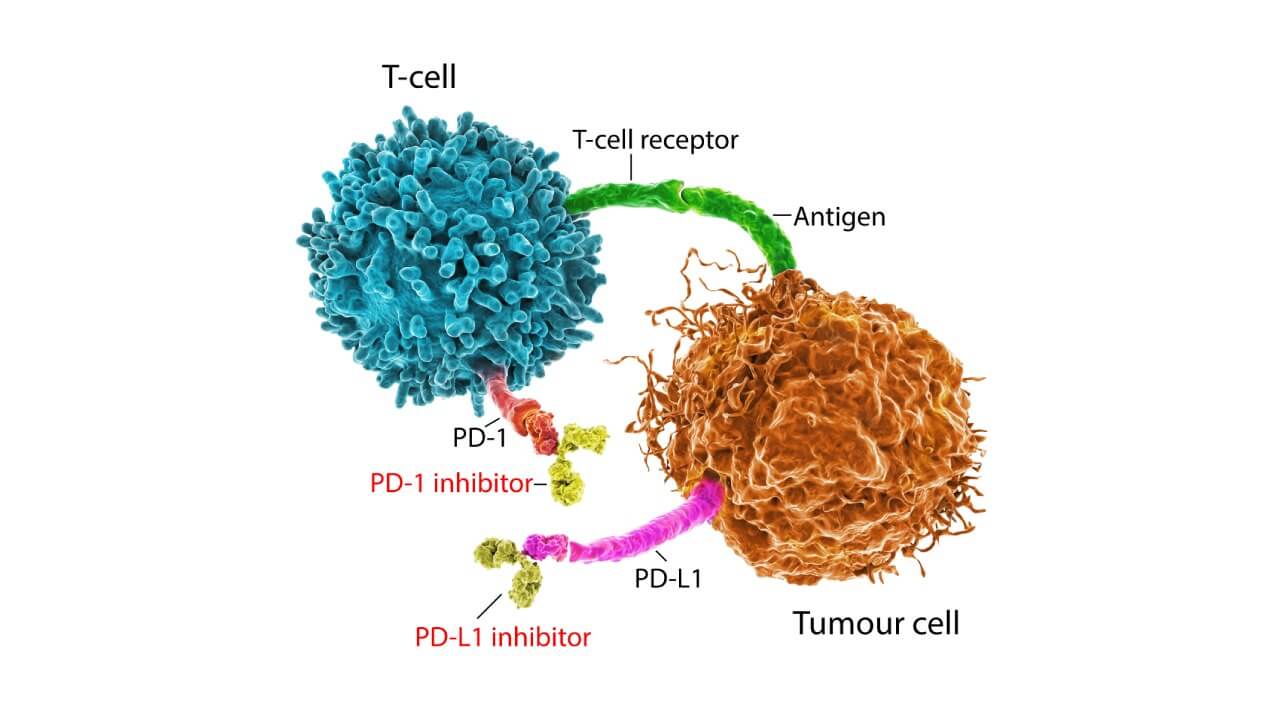
This class is the most extensively studied and widely used in clinics in Germany for non-small cell lung cancer and squamous cell carcinoma. Lung cancer immunotherapy with checkpoint inhibitors includes three main types:
- PD-1 inhibitors act on proteins in T-cells (killer cells of the immune system) to make tumor cells visible to the immune system.
- PD-L1 inhibitors enhance the same process by targeting the ligand expressed on lung cancer cells, boosting activated T-cells’ ability to attack cancer cells.
- CTLA-4 inhibitors regulate T-cell activity, increasing their efficiency in destroying cancer cells. They can be combined with PD-1 inhibitors and other lung cancer treatments.
Thus, checkpoint inhibitors are essential to cancer immunotherapy because they enhance the immune system's ability to fight cancer and support conventional lung cancer treatment approaches.
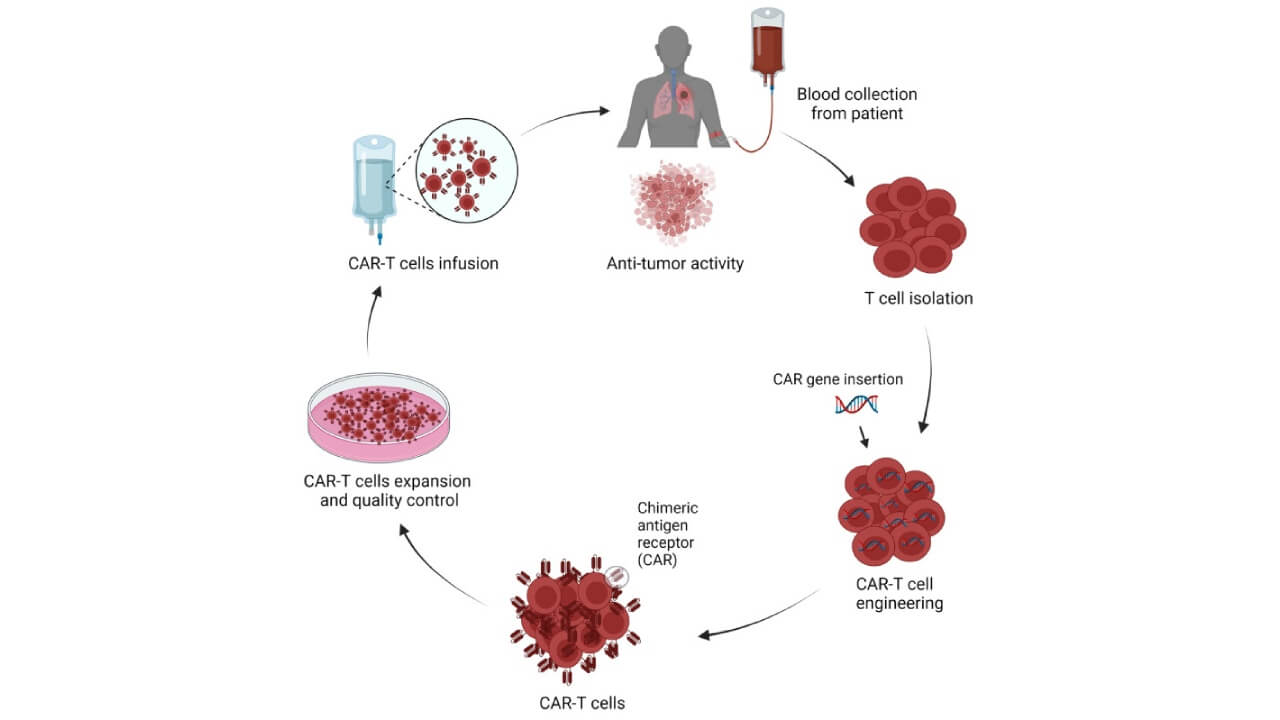
Adoptive T-Cell Transfer for Lung Cancer
CAR T-cells and other forms of adoptive cell treatment are the most advanced type of immunotherapy for lung cancer. The T-cells are taken out of the blood of the patient and are genetically modified to better attack lung cancer. This gives the immune system the power to target cancer cells.
CAR T-cell treatment enhances anti-cancer immunity by circumventing tumor masking, and shrinks primary tumors and metastases in many cases. Moreover, it alleviates such side effects as intoxication by cancer and respiratory distress. Activated T-cells have the ability to persist longer in attacking cancer cells following the treatment to ensure that an overall immune response is maintained.
An easier variant of adoptive cell therapy is where the T-cells are exposed to similar antigens that are present on lung cancer cells; the immune system can remember this and effectively target cancer cells in the future. This strategy enhances cancer immunotherapy outcomes and improves the quality of life for lung cancer patients, even in advanced lung cancer stages.
Hospitals and the Cost of Lung Cancer Treatment
Lung cancer treatment in Germany is provided by leading academic and university hospitals. These top-class facilities offer other lung cancer treatments, including minimally invasive surgery, advanced radiation therapy, and innovative lung cancer immunotherapy options. Patients can also access cancer immunotherapy protocols and participate in ongoing clinical trials when appropriate.
Doctors provide a thorough clinical examination, go over all diagnostic data, and talk about prior cancer treatments during the initial consultation. To evaluate tumor cells and the course of the disease, additional tests like CT or MRI scans might be carried out. A tumor board reviews each finding to develop a customized treatment plan.
Patients specifically seeking immunotherapy treatment can often consult remotely with German specialists before traveling. Prices for therapy vary individually, depending on the clinic, the patient’s age, and the type or stage of lung cancer being treated. This personalized approach ensures that lung cancer patients receive the most effective combination of therapies while optimizing quality of life.
| Treatment | 2-Year Survival Rate* | Response Rate** | Duration of treatment | Cost of treatment, €*** |
|---|---|---|---|---|
| Dendritic cell therapy | up to 85% | up to 90% | 1 week | 20,000 - 38,000 |
| Checkpoint inhibitors | up to 45% | up to 45% | about a year | 375,000 - 420,000 for the full course |
| CAR T-cell therapy | up to 50% | up to 40% | about 3 weeks | 450,000 - 550,000 |
*Booking Health data. Survival rates vary widely depending on the type of cancer, the patient's condition, and specific circumstances.
**Booking Health data. Response rate is the number of patients who show improvement after treatment.
***The cost of treatment depends on the type of tumor, stage of cancer, and other factors.
Benefits of Immunotherapy for Lung Cancer
The primary factors that influence the treatment decisions are the cancer stage and the general health of the patient. There are several possible advantages of immunotherapy, which can help lung cancer patients.
Key benefits include:
- Prolonged survival is superior to the outcome of conventional treatment of lung cancer in individuals with metastatic disease or advanced cancer.
- Improved life quality: unlike chemotherapy and radiation therapy, normal cells are generally spared, leading to a more favorable side effect profile. Also, immunotherapy may be applied as a palliative therapy to minimize the symptoms.
- Reduced possibility of recurrence after surgery, particularly in non-small cell lung cancer.
- The long-term disease control allows the immune system and immune cells to deal with tumor cells and transform cancer into a chronic condition instead of a lethal one.
- Greater effectiveness with other interventions.
These benefits illustrate why pulmonary cancer immunotherapy has become an essential part of cancer immunotherapy protocols in Germany, which gives cancer patients hope and improved outcomes at different stages of the disease.
Side Effects of Lung Cancer Immunotherapy
Immunotherapy of lung cancer has transformed the approach to treatment of the disease altogether by allowing the patient to employ his or her own immune system to get rid of the cancer cells in the lungs. Although it has many advantages, one should be aware of possible disadvantages and the way to handle them successfully. In contrast to the common practice in chemotherapy or radiation therapy, where the treatment may lead to widespread destruction of normal cells, immunotherapy directly hits the tumor cells and mostly spares the normal tissues. However, because this treatment relies on the activation of T-cells and other immune cells, it can sometimes result in immune-related adverse events (IRAEs) that require careful monitoring and management.
Common Side Effects
Mild to moderate side effects from lung cancer immunotherapy include fatigue, skin rash, pruritus, diarrhea, and nausea [4]. These symptoms are often temporary and can be managed with supportive care. In some patients, immune checkpoint activation may result in transient inflammation of the skin, gastrointestinal tract, or liver. Timely intervention and the right management of patients are the key to preventing side effects and preserving therapeutic effectiveness.
Rare but Serious Immune-related Adverse Events
Major immunological-related reactions can be caused by overactivation of T-cells. However, this is uncommon. The organ systems that may be affected by these events include the heart (myocarditis), endocrine glands (thyroiditis, adrenal insufficiency), liver (hepatitis), colon (colitis), and lungs (pneumonitis). Patients with small-cell lung cancer or advanced non-small-cell lung cancer may be more at risk from adoptive cell therapy or combination immune checkpoint inhibitors.
Managing Side Effects to Protect Normal Cells
One of the primary benefits of immunotherapy over conventional cancer treatment is the relative preservation of normal cells. By targeting only lung cancer cells or stimulating T-cells, the treatment lessens damage to healthy tissues. On the other hand, proactive control of side effects ensures immune cell activity and allows the patient to continue therapy without significant interruptions [5].
Strategies for Patients Undergoing Adoptive Cell Therapy
One of the most advanced forms of immunotherapy is adoptive cell treatment, which comprises the CAR T-cell therapy. The T-cells are taken out of the patient, modified to attack the cancerous cells of the lungs, and then they are reintroduced in order to boost the immune response. Such a strategy is rather successful, though, due to the hyperactivity of immune cells, sometimes it may result in neurotoxicity or cytokine release syndrome. Management involves premedication, close observations, and, in case of need, immunosuppressive medication intervention. The German institutions where such procedures are done have special teams to reduce risks and offer timely and supportive treatment.
Monitoring and Follow-up
To be safe and effective, immunotherapy must be continuously monitored. Regular blood tests, imaging studies, and clinical assessments help track tumor cell response to treatment and spot early warning signs of immune-related side effects. Modifications to the regimen, such as altering the dosage or therapy, are often guided by the patient's response and tolerance. To balance the potential risks of treatment against its benefits, regular monitoring is particularly important for patients with small-cell lung cancer (SCLC) or severe illness.
Success Stories in Immunotherapy Cancer Treatment
A Medical Journey: Every Step of the Way With Booking Health
Finding the best treatment strategy for your clinical situation is a challenging task. Being already exhausted from multiple treatment sessions, having consulted numerous specialists, and having tried various therapeutic interventions, you may be lost in all the information given by the doctors. In such a situation, it is easy to choose a first-hand option or to follow standardized therapeutic protocols with a long list of adverse effects instead of selecting highly specialized innovative treatment options.
To make an informed choice and get a personalized cancer management plan, which will be tailored to your specific clinical situation, consult medical experts at Booking Health. Being at the forefront of offering the latest medical innovations for already 12 years, Booking Health possesses solid expertise in creating complex management programs in each individual case. As a reputable company, Booking Health offers personalized treatment plans for lung cancer with direct clinic booking and full support at every stage, from organizational processes to assistance during treatment. We provide:
- Assessment and analysis of medical reports
- Development of the medical care program
- Selection of a suitable treatment location
- Preparation of medical documents and forwarding to a suitable clinic
- Preparatory consultations with clinicians for the development of medical care programs
- Expert advice during the hospital stay
- Follow-up care after the patient returns to their native country after completing the medical care program
- Taking care of formalities as part of the preparation for the medical care program
- Coordination and organization of the patient's stay in a foreign country
- Assistance with visas and tickets
- A personal coordinator and interpreter with 24/7 support
- Transparent budgeting with no hidden costs
Health is an invaluable aspect of our lives. Delegating management of something so fragile yet precious should be done only to experts with proven experience and a reputation. Booking Health is a trustworthy partner who assists you in pursuing stronger health and a better quality of life. Contact our medical consultant to learn more about the possibilities of personalized treatment with innovative methods for lung cancer with leading specialists in this field.
FAQ: Immunotherapy for Lung Cancer in Germany
Send request for treatmentImmunotherapy is a type of cancer treatment that helps the immune system fight cancer. It includes treatments like dendritic cell vaccines, checkpoint inhibitors, and CAR T-cell therapy.
Immunotherapy for lung cancer works by boosting the body's immune response against cancer cells. It can improve survival rates and is often used in combination with other treatments.
Dendritic cells are a type of immune cell that helps stimulate the immune system to attack cancer cells. They play a crucial role in cancer immunotherapy.
Dendritic cell therapy has shown promise in treating various cancers, including melanoma and prostate cancer. It works by enhancing the body's immune response to target and destroy cancer cells.
Adding immunotherapy to standard treatment significantly improves response rates in both early and advanced stages of lung cancer. It extends survival, improves quality of life, and can help manage cancer as a chronic condition.
Dendritic cell vaccines can be effective at any stage of lung cancer treatment. Other types of immunotherapy are mainly used for advanced or metastatic lung cancer.
Prices for lung cancer immunotherapy in Germany can differ a lot – even between clinics in the same city. Dendritic cell therapy cost falls somewhere between €20,000-€38,000; checkpoint inhibitors are more expensive – you will need to pay €375,000-€420,000 for the full course. CAR T-cell therapy is the most costly one, ranging from €450,000-€550,000.
Dendritic cell vaccines have low toxicity – about 1%. Thus, this treatment is among the best-tolerated ones. Chemotherapy has a high toxicity of 65-80%, while targeted therapy shows moderate toxicity of 15-20%.
Dendritic cell vaccines are suitable for both early and advanced stages; this treatment option can be used post-surgery or as a standalone. Targeted therapy is administered in the presence of specific genetic mutations like EGFR, ALK, or ROS1 in the tumor tissue.
Dendritic cell vaccines provide a reliable long-term result, up to lifelong immune memory. Chemotherapy produces temporary effects – limited to the course of treatment. Targeted therapy offers long-lasting results but only in the presence of specific mutations.
The 2-year survival rate for dendritic cell therapy is up to 85%. This is significantly higher than checkpoint inhibitors – up to 45% and CAR T-cell therapy – up to 50%. Survival rates depend on the type of cancer, comorbidities, etc.
Dendritic cell therapy demonstrates the highest response rate – it reaches 90%. Checkpoint inhibitors show response rates up to 45%, and CAR T-cell therapy achieves up to 40%.
Dendritic cell therapy is the shortest: initial consultation and examination, vaccine manufacturing and injection – all take about 1 week. CAR T-cell therapy takes about 3 weeks. The course of checkpoint inhibitors requires approximately a year of treatment.
Immunotherapy of lung cancer in Germany depends on the cost of treatment, the clinic, and the individual patient's needs. Final prices are determined by considering the assessment of specialists, taking into account the condition of the patient and the chosen treatment plan for lung cancer.
Choose treatment abroad and you will for sure get the best results!
Authors:
This article was edited by medical experts, board-certified doctors Dr. Nadezhda Ivanisova, and Dr. Bohdan Mykhalniuk. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Our editorial policy, which details our commitment to accuracy and transparency, is available here. Click this link to review our policies.
Sources:
[1] Krishna Chaitanya Thandra, Adam Barsouk, Kalyan Saginala, John Sukumar Aluru, Alexander Barsouk. Epidemiology of lung cancer. Contemp Oncol (Pozn). 2021;25(1):45-52. doi: 10.5114/wo.2021.103829. [DOI] [PubMed]
[2] Dieter Stevens, Joline Ingels, Sandra Van Lint, Bart Vandekerckhove, Karim Vermaelen. Dendritic Cell-Based Immunotherapy in Lung Cancer. Front Immunol. 2021 Feb 12;11:620374. doi: 10.3389/fimmu.2020.620374. [DOI] [PMC free article]
[3] Prameela Kandra, Rajender Nandigama, Bastian Eul et al. Utility and Drawbacks of Chimeric Antigen Receptor T Cell (CAR-T) Therapy in Lung Cancer. Utility and Drawbacks of Chimeric Antigen Receptor T Cell (CAR-T) Therapy in Lung Cancer. Front Immunol. 2022 Jun 2;13:903562. doi: 10.3389/fimmu.2022.903562. [DOI] [PMC free article]
[4] Preethika Mahalingam A, Thomas Newsom-Davis. Cancer immunotherapy and the management of side effects. Clin Med (Lond). 2024 Apr 11;23(1):56–60. doi: 10.7861/clinmed.2022-0589. [DOI] [PMC free article]
[5] Cristina Gutierrez, Colleen McEvoy, Laveena Munshi et al. Critical Care Management of Toxicities Associated with Targeted Agents and Immunotherapies for Cancer. Crit Care Med. Author manuscript; available in PMC: 2021 Jan 1. Published in final edited form as: Crit Care Med. 2020 Jan;48(1):10–21. doi: 10.1097/CCM.0000000000004087. [DOI] [PMC free article]
Read:
Germany 5 Leading Hospitals for Lung Cancer Care