Lung cancer has been one of the most common causes of cancer death in the world for many decades. It is a serious global problem that affects millions of people. Non-small cell lung cancer is the most common type of cancer diagnosed, accounting for the majority of all cases. In the past, the prognosis for such patients was poor, as the disease was usually diagnosed at a late stage, when treatment options were limited [1].
Today, the situation is changing significantly. In recent years, the treatment of non-small cell lung cancer has made great strides forward with the advent of modern targeted drugs and immunotherapy. These methods allow doctors to tailor treatment to the individual patient's tumor. As a result, therapy is more effective, and the duration and quality of life are higher.
New approaches have radically changed the standard of care and given lung cancer patients real hope where there was almost no hope before.
Non-Small Cell Lung Cancer: Types and Treatment Strategies
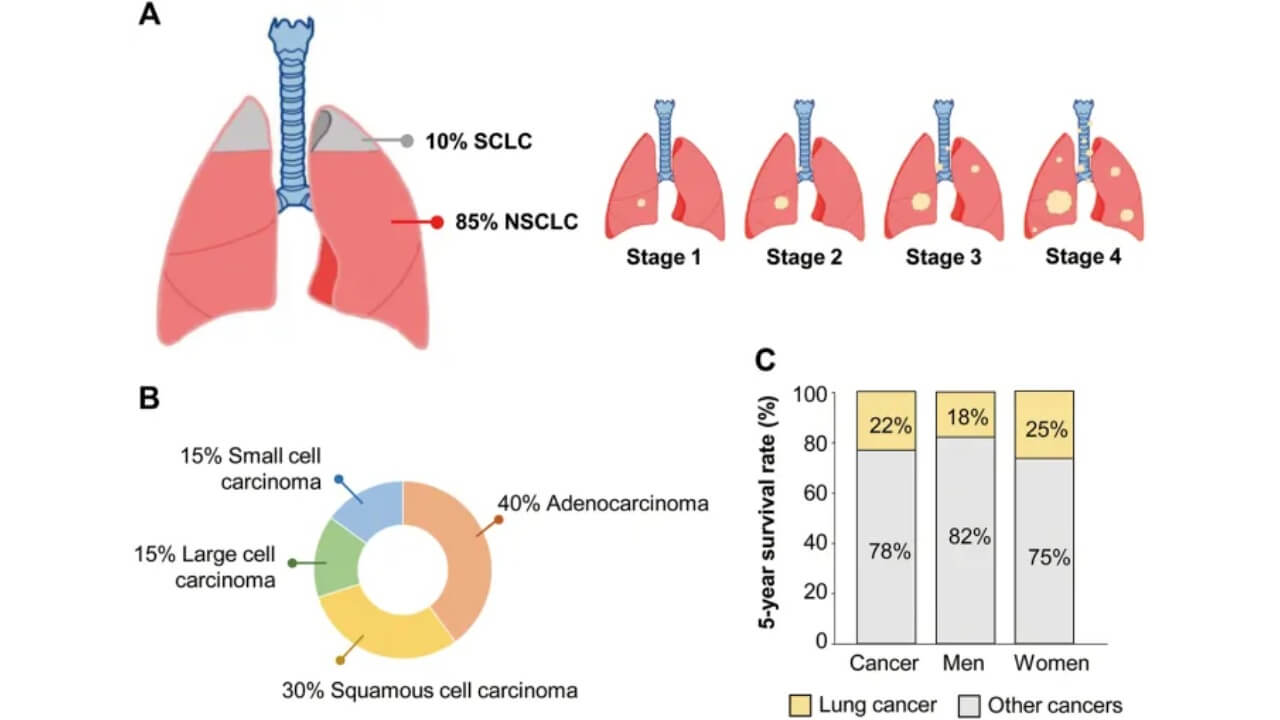
There are two main types of lung cancer: non-small cell lung cancer (NSCLC) and small cell lung cancer (SCLC). They differ in how quickly the tumor grows and how it responds to treatment.
Non-small cell lung cancer includes several main types. Adenocarcinoma is the most common variant and is often found in non-smokers; it is this type that most often reveals molecular mutations important for personalized treatment. Squamous cell carcinoma is usually associated with smoking and develops from abnormal cells of the respiratory tract. Large cell carcinoma is less common and is characterized by a less differentiated structure. Small cell lung cancer is also distinguished, which is a more aggressive form of lung cancer and requires different approaches to treatment. Large cell carcinoma is a rare subtype of lung cancer that is often diagnosed at later stages due to the lack of specific early symptoms and may have a faster growth rate compared to other forms of NSCLC.
NSCLC is the most common type. It usually grows more slowly and has more treatment options, especially if early detection of the disease was achieved or if the tumor has certain molecular features. SCLC is rarer but much more aggressive. It spreads quickly, so treatment usually begins with systemic therapy.
Because of these differences, the treatment approaches for NSCLC and SCLC are fundamentally different.
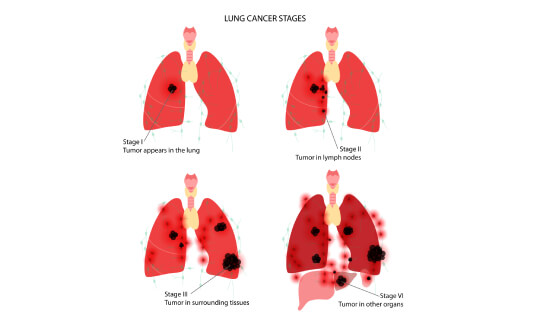
The stage of the disease indicates how far the cancer has spread.
- In early stages, the goal of treatment is to completely remove or destroy the tumor, often with a chance of cure.
- In advanced stages, treatment is aimed at controlling the disease, slowing its progression, and improving quality of life.
Therefore, the same type of lung cancer may be treated differently depending on the stage.
Why are biomarkers important?
Biomarkers are features of a tumor that tell a doctor which treatment will be most effective for that patient.
In some cases, they allow for targeted therapy or immunotherapy, which are more precise and often better tolerated than standard chemotherapy.
Treatment Options for Non-Small Cell Lung Cancer by Stage
The approach to treating non-small cell lung cancer depends on how advanced the disease is and the biology of the tumor. Today, treatment often combines several methods and is tailored to the individual.
Early stages NSCLC (I-IIIA), when the tumor can be removed surgically
During early detection of the disease, the main goal of treatment is to completely remove the tumor and reduce the risk of the disease returning.
- Surgery remains the key stage.
- After surgery, doctors may recommend additional treatment – chemotherapy or immune therapy – to destroy any microscopic cancer cells.
- In some cases, modern immunotherapy after surgery helps to significantly reduce the risk of recurrence, especially if the tumor has certain immune markers.
- Increasingly, immunotherapy or its combination with chemotherapy is used before surgery to shrink the tumor and improve the effectiveness of surgery.
This combined approach increases the chances of a long life without other factors of disease.
Stage III NSCLC, when surgery is not possible
If the tumor cannot be removed surgically, treatment is aimed at controlling the disease and prolonging life.
- The standard is a combination of chemotherapy and radiation therapy, given at the same time.
- After this stage, many lung cancer patients are given immune therapy, which helps the immune system keep the disease under control.
- This approach has significantly improved survival compared to previous treatments.
Advanced or metastatic cancer (stage IV NSCLC)
In later stages, the cancer has spread beyond the lung tissue, so treatment is systemic and affects the entire body.
- If there are no specific genetic changes in the tumor, immunotherapy becomes the mainstay of treatment – alone or in combination with chemotherapy.
- In some patients, immunotherapy can provide long-term control of the disease and allow them to live for years with a good quality of life.
- In some cases, a combined approach of two immunotherapy drugs are used, sometimes together with a short course of chemotherapy – this enhances the effect of the treatment.
- The choice of regimen depends on the general condition of the patient and the biological characteristics of the tumor.
Surgery for Non-Small Cell Lung Cancer
Today, surgical treatment of non-small cell lung cancer can be performed effectively. The choice of method depends on the size of the lesion, its location, the stage of the disease, lung function and the general condition of the patient.
Minimally invasive surgery: a modern approach
In recent decades, minimally invasive surgical techniques performed through small incisions in the chest have become increasingly popular:
- Video-assisted thoracoscopic surgery (VATS)
- Robotic-assisted thoracoscopic surgery (RATS)
Compared to classic open surgery (thoracotomy), these methods usually cause less postoperative pain, reduce the risk of complications, reduce the length of hospital stay, allowing for faster recovery from the intervention
Studies have shown that, provided the surgical team is sufficiently experienced, minimally invasive surgeries are not inferior to open ones in terms of treatment effectiveness and long-term results, especially in the early stage NSCLC [3].
Robot-assisted aurgery: what does it mean?
Robot-assisted surgery is a type of minimally invasive intervention in which the doctor controls high-precision instruments using a robotic system.
The advantages of this approach are:
- better visualization of the surgical field
- high precision of movements
- convenience of working in anatomically complex areas.
In terms of clinical results, robot-assisted surgery is generally comparable to VATS, and in some cases can facilitate the performance of complex interventions. The main limitation remains their higher cost.
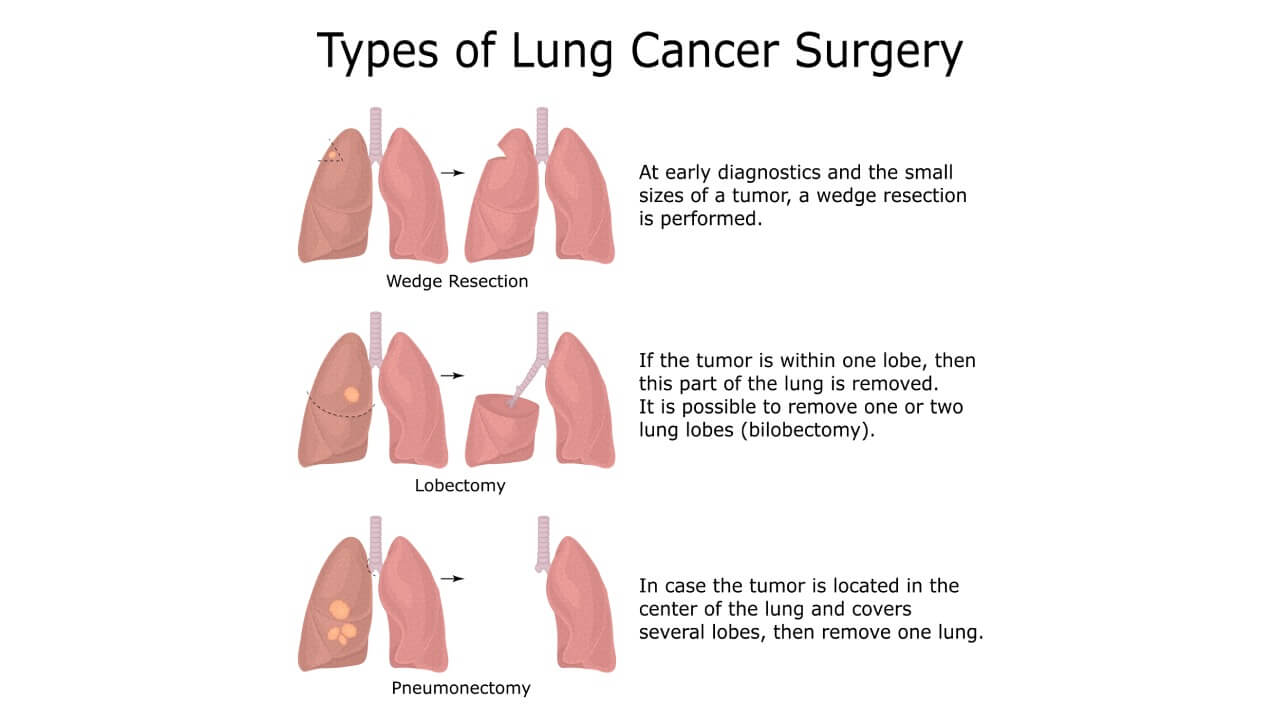
How much of the lung is removed during surgery?
Lobectomy (removal of one lobe of the lung) is considered the standard and most often recommended type of surgery for early non-small cell lung cancer.
It provides the optimal balance between effective disease control and preservation of respiratory function, allowing the other lung and remaining lung tissue to continue supporting adequate breathing capacity.
In some situations, doctors may suggest a smaller volume of surgery, for example:
- segmentectomy (removal of part of a lobe of the lung)
- wedge resection.
Such interventions may be appropriate if:
- the tumor is very small (up to 2 cm)
- the cancer has less aggressive characteristics
- the patient has reduced lung function or comorbidities
- the patient has previously undergone lung surgery.
Pneumonectomy involves removal of the whole lung and is generally reserved for selected cases of non-small cell lung cancer when the tumor is too extensive to be treated. As a rule, a pneumonectomy is performed using open techniques, since the surgeons remove not only an entire lung, but also the regional lymph nodes.
According to current data, in carefully selected patients with very early forms of cancer, limited resections can provide results comparable to lobectomy, provided there is sufficient "reserve" of healthy tissue around the tumor and adequate examination of the nearby lymph nodes [4].
Radiation Treatment Options for Non-Small Cell Lung Cancer
Radiation therapy is a noninvasive therapy that uses highly targeted radiation to kill cancer cells. For many patients with non-small cell lung cancer, it is an effective alternative to surgery or other therapies and is an important part of combined approach to treat.
Radiation therapy is most often considered in the following situations:
- if the cancer is detected at an early stage, but the patient cannot undergo surgery due to comorbidities
- if the patient refuses surgery
- as part of a combined approach to treat in later stages
- to control symptoms and improve quality of life.
Radiation therapy for non-small cell lung cancer can be delivered using a variety of methods, each with its own indications and characteristics. The most common treatments are external beam radiation therapy (EBRT) and stereotactic body radiation therapy (SBRT). The table below summarizes the key differences between these approaches to help you better understand when and why doctors choose one treatment option over another [5].
| Criteria | EBRT | SBRT |
|---|---|---|
| Essence of the method | Classical fractional irradiation with small doses | High-precision irradiation with high doses |
| Number of sessions | Usually 20-35 procedures | Usually 1-5 procedures |
| Duration of treatment | Several weeks | From several days to 1-2 weeks |
| Targeting accuracy | High | Very high |
| Effect on healthy tissues | Greater | Minimal |
| Indications | If surgery is not possible or desirable; in combination with chemotherapy for stage III disease; after surgery to reduce the risk of the disease returning; for palliative purposes to relieve symptoms such as pain or shortness of breath | In early stages of NSCLC, when the tumor is small; in patients who cannot undergo surgery due to comorbidities; as an alternative to surgery in selected cases |
In addition to classical methods of radiation therapy for NSCLC, in modern oncology there are also alternative light-oriented approaches to local effects on the tumor. One of such methods is photodynamic therapy, which allows for selective destruction of tumor cells using light of a certain wavelength, with little damage to healthy tissues, and can be used in carefully selected patients as part of an individualized treatment strategy.
Chemotherapy for Non-Small Cell Lung Cancer Therapy
Chemotherapy is one of the mainstays of treatment for non-small cell lung cancer (NSCLC). It affects cancer cells throughout the body and can be used at different stages of the disease, either alone or in a combined approach with other treatments. It is the effect of chemotherapy on healthy cells that explains such temporary phenomena as fatigue, hair loss, or changes in blood counts.
The role of chemotherapy depends on the stage of the disease, the extent of the disease, and the patient’s overall health.
Chemotherapy before surgery (neoadjuvant treatment)
In some patients with potentially operable lung cancer, chemotherapy may be given before surgery.
The main goals of this approach are shrinking the tumor, targeting microscopic areas of disease that are not yet visible on imaging and improving the effectiveness of subsequent treatment.
The decision to use chemotherapy before surgery is made on an individual basis and is usually discussed by a multidisciplinary team.
Chemotherapy in combination with radiation therapy
For locally advanced NSCLC, when surgery is not possible, chemotherapy is often used simultaneously with radiation therapy.
This approach allows:
- to enhance the effect of radiation
- to better control tumor growth
- to improve therapy outcomes compared to radiation therapy alone.
It is the combination of these methods that is considered the standard of care for certain stages of NSCLC.
Chemotherapy for advanced or metastatic cancer
When lung cancer spreads beyond the chest wall, chemotherapy becomes a systemic therapy aimed at slowing the progression of the disease, reducing symptoms, extending life and preserving its quality.
At this stage, chemotherapy can be used alone or in integrated approach with immune therapy, depending on the characteristics of the tumor [6].
Targeted Therapy for Non-Small Cell Lung Cancer with Actionable Mutations
Targeted therapy is a modern type of treatment for non-small cell lung cancer (NSCLC) that targets specific molecular "breakages" in cancer cells rather than the entire body. That’s why it’s called targeted or personalized therapy. In some patients, lung cancer develops due to specific genetic changes that "trigger" tumor growth.
Such changes are called actionable mutations because there are specific treatments for them that can specifically block these abnormalities. In simple words: if a target mutation is found, the doctor can choose a therapy that acts specifically on the cause of tumor growth, not just on its consequences.
Unlike chemotherapy, which affects all rapidly dividing cells (even normal cells), targeted therapy:
- acts selectively
- causes less damage to healthy tissue
- is often better tolerated
- can provide long-term control of the disease, even in advanced stages.
Not all patients with NSCLC have target mutations. That is why, before starting treatment, molecular profiling of the tumor is performed – a special genetic study that allows identifying mutations that drive cancer growth, determining whether targeted therapy is suitable, planning further lines of therapy in case of disease progression. This examination is a key stage in modern therapy of NSCLC. Most often, this research is carried out using modern sequencing technologies (NGS).
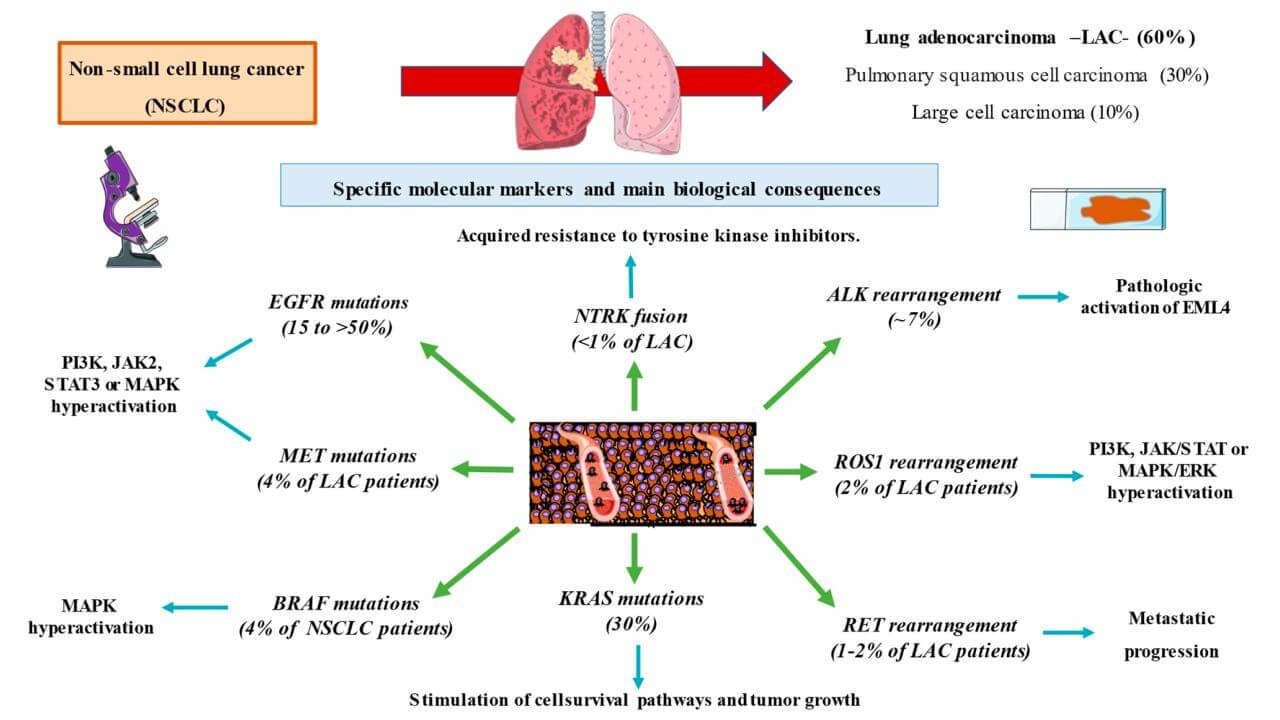
EGFR
One of the most common mutations in non-small cell lung cancer, especially among:
- women
- people who have never smoked or smoked lightly
- patients with adenocarcinoma.
This mutation leads to a constant signal for cell growth and uncontrolled division. The discovery of EGFR-mutated cancer allowed the first systemic use of targeted therapy in lung cancer.
ALK
Genetic rearrangement that is more common:
- in younger patients
- in non-smokers
- in adenocarcinoma.
ALK-associated cancer has a tendency to affect the brain, but at the same time it responds well to targeted therapy, which can effectively control both the tumor in the lungs and metastases in the CNS.
ROS1
A rare but clinically important mutation that is similar in properties to ALK.
It is usually found in young patients and non-smokers and may be an effective target for personalized therapy.
BRAF
This mutation activates signaling pathways responsible for the growth and survival of specific cancer cells. There are different subtypes of BRAF mutations, which may have different clinical significance and prognosis.
MET
Disruptions in this gene lead to increased survival and motility of cancer cells.
Some types of MET alterations are particularly characteristic of more aggressive forms of tumors, but may also be sensitive to targeted therapy.
RET
A rare genetic rearrangement that occurs more frequently in young non-smokers.
Like some other mutations, RET is associated with an increased risk of central nervous system damage, but at the same time is a clear therapeutic target.
KRAS G12C
One of the most common mutations in NSCLC, especially among smokers. For a long time, KRAS was considered a "non-treatable" target, but recent years have opened up opportunities for targeting the G12C subtype [7].
Tumor production of VEGF (vascular endothelial growth factor) and other growth factors leads to an angiogenic switch, where a new vascular network forms in and around the tumor, allowing it to grow exponentially. Overexpression of VEGF, which is often seen in lung cancer, is associated with increased angiogenesis, tumor progression, and metastasis.
Immunotherapy for Non-Small Cell Lung Cancer
Immunotherapy is a modern treatment for non-small cell lung cancer (NSCLC) that helps the body's own immune system recognize and destroy cancer cells. Unlike traditional methods, immunotherapy does not act directly on the tumor, but "turns on" the body's natural defense mechanisms.
Cancer cells can "hide" from the immune system by blocking its work. Immunotherapy removes these blockages, allowing immune normal cells to recognize the cancer cells, attack it, maintain long-term control of the disease. As a result, some patients achieve a stable response to treatment that can be maintained for a long time.
In some patients, immunotherapy can be used alone, without the addition of other treatments. This approach is possible when the tumor has signs indicating high sensitivity to immune therapy, the general condition of the patient allows avoiding additional burden, and sufficient disease control is expected without combined treatment.
In many cases, immunotherapy is combined with other treatments to enhance the effect:
- Immune therapy + chemotherapy
Chemotherapy can help "prime" the tumor for an immune response, making it more visible to the immune system.
- Immune therapy + radiation therapy
Irradiation can enhance the immune response and improve disease control.
- Combined approach of different immunotherapeutic approaches
In some cases, pairing immunotherapies with different mechanisms of action is used.
Dendritic cells therapy
The choice of a combined approach is always based on a balance of efficacy and safety.
Although modern immune therapy has already significantly changed the treatment of non-small cell lung cancer, research in this area continues. Scientists are looking for ways to even more accurately teach the immune system to recognize the tumor and make the immune response more controlled and effective. One such innovative direction is therapy using dendritic cells – a method that aims to "reprogram" the immune response at an earlier and more fundamental level.
Dendritic cell therapy is an innovative immune therapy approach that aims to train a patient’s own immune system to recognize and respond to cancer cells more effectively. The Nobel Prize in Physiology or Medicine was awarded in 2011 for the discovery of the role of dendritic cells in the immune system, which became the scientific basis for the development of dendritic cell immune therapy [10]. Unlike methods that directly destroy tumors, this approach works by activating the body’s natural defense mechanisms.
For non-small cell lung cancer, dendritic cell therapy is most often considered as part of a comprehensive treatment. It can be used in conjunction with systemic therapy or after standard treatments, especially in patients with advanced or recurrent disease. The goal of this approach is to help the immune system control the disease for longer and maintain disease stability.
We will tell you more about this approach in the article Dendritic Cell Immunotherapy for Non-Small Cell Lung Cancer.
At the same time, access to such highly specialized treatments often requires complex coordination between clinics, laboratories, specialists and other factors. This is where Booking Health plays an important role, helping patients organize dendritic cell treatment at leading medical centers, providing medical support, coordination of therapy stages and transparent access to modern immuno-oncology solutions.
Combined Therapy Options in Non-Small Cell Lung Cancer
Modern treatment of non-small cell lung cancer (NSCLC) is increasingly not limited to a single method. In many cases, the best results are achieved by combining several approaches, each of which complements the other.
| Criteria | Chemoimmunotherapy | Chemoradiotherapy |
|---|---|---|
| The essence of the approach | Combined approach of chemotherapy with immune therapy | Combined approach of chemotherapy with radiation therapy |
| How it works | Chemotherapy shrinks the tumor, immune therapy activates the immune system | Radiation therapy acts locally on the tumor, chemotherapy enhances its effects |
| When used | Mostly for advanced or metastatic cancer | Most often for locally advanced cancer when surgery is not possible |
| Treatment goal | Disease control, prolongation of life | Maximum control of the tumor in the thorax |
A key element of combined treatment is the work of a multidisciplinary team of doctors. It usually includes:
- oncologists
- surgeons
- radiation oncologists
- pathologists
- and other specialists.
It is the joint discussion that allows to correctly determine the sequence of treatment, choose the optimal combinations of methods, and avoid excessive or ineffective treatment.
For the patient, this means that the decision is made not by one doctor, but by a team of specialists, taking into account all medical nuances.
TACE for Non-Small Cell Lung Cancer
TACE (transarterial chemoembolization) is a minimally invasive treatment that combines local administration of anticancer drugs with blocking the blood supply to the tumor. This approach has long been used for some types of cancer and, in some cases, can also be used for non-small cell lung cancer, particularly as part of locoregional interventional approaches such as thoracic chemoperfusion, aimed at achieving higher drug concentrations at the tumor site while limiting systemic exposure.
The procedure is performed by an interventional radiologist through a thin catheter that is inserted into the vessels:
- The catheter is brought directly to the arteries that feed the tumor.
- The drug is delivered locally, directly to the tumor area.
- At the same time, special particles are injected that partially or completely block the blood flow to the tumor.
As a result:
- the tumor receives less oxygen and nutrients
- the concentration of drugs in the affected area is significantly higher
- the systemic effect on the body is less expressed than with conventional chemotherapy.
To gain a deeper understanding of the possibilities of transarterial chemoembolization and modern interventional approaches in oncology, we suggest watching an exclusive interview with Attila Kovács, a leading expert in interventional radiology with over 26 years of clinical experience. In the video, Prof. Dr. Attila Kovács explains in an accessible way when, how, and for what purpose TACE is used in NSCLC, and also shares his vision of the future of interventional oncology as one of the key areas of modern cancer treatment.
Treatment Options for Advanced Non-Small Cell Lung Cancer
Advanced or metastatic non-small cell lung cancer means that the disease has spread beyond one area of the lung. At this stage, the mainstay of advanced non-small cell lung cancer treatment is systemic therapy, which means treatment that affects the entire body. Surgical treatment is usually not recommended for stage IIIB or stage IVB non-small cell lung cancer, where the disease is typically managed with systemic and combined treatment approaches.
The goal of treatment for advanced NSCLC is to control the disease, slow its progression, reduce symptoms, and maintain quality of life [9].
Stage IV cancer is usually treated with drugs that target cancer cells throughout the body. These include:
- chemotherapy
- immune therapy
- targeted therapy (if there are target mutations)
- or a combination of these.
The choice to treat NSCLC depends not only on the stage, but also on the biology of the tumor and the patient’s condition.
Along with non-small cell lung cancer treatment options, supportive and palliative care plays an important role, which may include control of pain, shortness of breath and fatigue, treatment of side effects of therapy, psychological and symptomatic support, assistance in adapting to changes in daily life.
Supportive care as a stage 4 NSCLC treatment option does not mean abandoning active therapy, but is a way to improve well-being and maintain a decent quality of life.
Why Patients Choose Non-Small Cell Lung Cancer Therapy Abroad
Many patients consider NSCLC treatment abroad to gain access to advanced diagnostic tools and personalized treatment strategies.
In leading oncology centers, treating cancer begins with a complete molecular profiling of the tumor. This allows them to accurately identify target mutations, avoid ineffective treatments and select the optimal first-line systemic therapy.
Non-Small Cell Lung Cancer Treatment in Germany
Patients with non-small cell lung cancer choose Germany primarily because of the structured and technologically advanced system of oncology care, where each stage of treatment is logically connected to the previous one. Lung cancer treatment in Germany almost always begins with advanced diagnostics, including molecular profiling of the tumor, which allows you to immediately determine the biology of the disease and avoid empirical decisions. This is especially important in advanced or complex forms of lung cancer, when the right choice of first-line treatment for non-small cell lung cancer is crucial.
A key difference of the German approach is the mandatory multidisciplinary assessment of the case. In almost all certified oncology centers, the decision to treat NSCLC is made by the tumor board, where oncologists, thoracic surgeons, radiation therapists, radiologists and pathologists work together. This format allows not only to choose the optimal integrated approach of treatment methods, but also to clearly determine the sequence of therapy – for example, when it is advisable to combine systemic treatment with local methods or change the strategy when the course of the disease changes.
An important reason for choosing Germany is also the wide access to modern radiotherapy, in particular to highly precise methods such as SBRT. In German centers, these technologies are used not episodically, but as part of standard clinical protocols, which allows achieving local tumor control with minimal burden on healthy tissues. In addition, clinics have extensive experience in using combined treatment regimens, where systemic therapy is combined with radiation or interventional oncology, depending on the stage and prevalence of the process.
One of the reasons why patients choose to have their non-small cell lung cancer therapy in Germany is the opportunity to go through the entire treatment path in a clearly structured system. This is largely facilitated by the work of Booking Health, which ensures coordination between the patient, German clinics and doctors, helping to transform a complex medical process into a clear and consistent treatment strategy.
Overview of Treatment Costs
Below is a rough comparison of the costs of different treatments for non-small cell lung cancer. These data are provided for informational purposes only, as the actual cost of the main treatment may vary significantly depending on the stage of the disease, the chosen therapeutic strategy, the duration of treating cancer, the required diagnostic procedures, and the individual clinical characteristics of the patient.
| Treatment type | Cost Germany | Cost USA | Cost GB | Cost Australia |
|---|---|---|---|---|
| Surgery for NSCLC | €15,000 – €25,000 | €65,000 – €85,000 | €35,000 – €55,000 | €20,000 – €50,000 |
| Chemotherapy | €7,300 – €12,100 per cycle | €100,000 – €180,000 full course | €90,000 – €165,000 full course | €5,000 – €250,000 for one cycle |
| Radiotherapy | €28,000 – €42,000 | €40,000 – €80,000 | €35,000 – €65,000 | €17,000 – €22,000 |
| DC therapy | €20,000 – €38,000 | €40,000 – €100,000 | not available | not available |
| TACE (transarterial chemoembolization) | €6,500 – €24,000 per session | €37,000 – €150,000 | €30,000 – €118,000 | €30,000 – €80,000 |
| NSCLC targeted therapy | €375,500 – €420,000 full course | €600,000 – €1,000,000 full course | €400,000 – €500,000 full course | not available |
| Immunotherapy for NSCLC | €20,000 – €38,000 for 1 cycle | €35,000 – €60,000 for 1 cycle | €25,000 – €45,000 for 1 cycle | €50,000 – €120,000 for 1 cycle |
Patient Experience and Treatment Outcomes Abroad
Patients facing advanced non-small cell lung cancer often find themselves in a situation where not only the treatment itself is important, but also the clear organization of each stage – from logistics to communication with doctors. This is what the experience of the family of a patient from Canada with stage 4B non-small cell lung cancer with distant metastases to the brain, lungs, liver, bones and left adrenal gland emphasizes. The patient was also found to have an EGFR exon 19 deletion mutation, which played a key role in choosing a treatment plan.
When organizing NSCLC treatment options in Munich, the Booking Health team took care of all organizational issues. According to the family, translation, transfer, appointment for a consultation, and assistance with accommodation were organized in advance and clearly. All arrangements were carried out on time, and communication was fast and clear, which is especially important in a situation where every decision matters.
The main treatment and consultation were supervised by Prof. Gansauge, which gave the family a sense of confidence and a professional approach at every stage. For the patient's relatives, it was important to be able to focus not on organizational difficulties, but on supporting their loved one and making medical decisions.
This experience shows that with complex oncological diagnoses, treatment abroad – in particular in Germany – can be much easier and less stressful when all processes are coordinated by one team. It is this support that allows patients and their families to focus on the main thing – treatment and quality of life.
A Medical Journey: Every Step of the Way With Booking Health
Finding the best treatment strategy for your clinical situation is a challenging task. Being already exhausted from multiple treatment sessions, having consulted numerous specialists, and having tried various therapeutic interventions, you may be lost in all the information given by the doctors. In such a situation, it is easy to choose a first-hand option or to follow standardized therapeutic protocols with a long list of adverse effects instead of selecting highly specialized innovative treatment options.
To make an informed choice and get a personalized cancer management plan, which will be tailored to your specific clinical situation, consult medical experts at Booking Health. Being at the forefront of offering the latest medical innovations for already 12 years, Booking Health possesses solid expertise in creating complex cancer management programs in each case. As a reputable company, Booking Health offers personalized non-small cell lung cancer (NSCLC) treatment plans with direct clinic booking and full support at every stage, from organizational processes to assistance during treatment. We provide:
- Assessment and analysis of medical reports
- Development of the medical care program
- Selection of a suitable treatment location
- Preparation of medical documents and forwarding to a suitable clinic
- Preparatory consultations with clinicians for the development of medical care programs
- Expert advice during the hospital stay
- Follow-up care after the patient returns to their native country after completing the medical care program
- Taking care of formalities as part of the preparation for the medical care program
- Coordination and organization of the patient's stay in a foreign country
- Assistance with visas and tickets.
- A personal coordinator and interpreter with 24/7 support
- Transparent budgeting with no hidden costs
Health is an invaluable aspect of our lives. Delegating management of something so fragile yet precious should be done only to experts with proven experience and a reputation. Booking Health is a trustworthy partner who assists you on the way of pursuing stronger health and a better quality of life. Contact our medical consultant to learn more about the possibilities of personalized treatment with innovative methods for non-small cell lung cancer (NSCLC) with leading specialists in this field.
Modern Cancer Treatment: Patient Journeys with Booking Health
Frequently Asked Questions About Non-Small Cell Lung Cancer Treatment Options
Send request for treatmentThe main non-small cell lung cancer therapy options include surgery, radiation therapy, chemotherapy, targeted drugs, and immunotherapy, with the choice depending on the stage, biomarkers, and overall condition of the patient.
NSCLC treatment options by stage are typically as follows: in early stages, local methods (surgery or SBRT) are preferred, in stage III, combination approaches are often required, and in stage IV, systemic treatment of NSCLC with biomarker-based personalization is preferred.
Surgery for NSCLC is most often considered in early resectable stages when the tumor can be removed radically, and in selected cases after tumor shrinkage with systemic treatment.
Radiation therapy for NSCLC may include external beam radiation NSCLC for locally advanced forms and SBRT for NSCLC as a highly targeted option for small early tumors or isolated foci.
Yes, chemotherapy for NSCLC remains an important part of treatment – both as part of combination regimens and in advanced disease, especially when rapid systemic control is needed.
NSCLC targeted therapy is a treatment that targets specific «breakdowns" in tumor cells, and patients with actionable mutations in NSCLC treatment identified by molecular testing NSCLC may benefit most.
Immunotherapy for NSCLC helps the immune system to attack the tumor more actively, often by blocking the "brakes" of the immune response – this is how immune checkpoint inhibitors NSCLC work.
Current stage 4 NSCLC treatment options are usually based on metastatic NSCLC therapy: immunotherapy, chemotherapy, targeted therapy for target mutations, or a combination of these, depending on the tumor profile and patient condition.
The most common side effects of NSCLC treatment depend on the method: possible chemotherapy side effects NSCLC (fatigue, nausea, decreased blood counts), radiation side effects NSCLC (irritation of the esophagus, cough, fatigue), and immunotherapy side effects NSCLC (inflammatory reactions of the skin, intestine, lungs, or thyroid gland).
Yes, personalized NSCLC treatment often improves treatment outcomes for non-small cell lung cancer, because it allows you to choose the therapy more precisely based on molecular testing NSCLC and immune markers.
Patients choose NSCLC treatment abroad because of access to advanced molecular diagnostics, multidisciplinary solutions, modern radiotherapy and combined protocols in specialized centers of advanced oncology care abroad.
Booking Health helps organize non-small cell lung cancer therapy in Germany, providing treatment coordination in Germany: document analysis, selection of clinic and specialist, coordination of consultations, translation and logistics, so that the patient can organize NSCLC treatment in Germany more consistently and understandably.
Life expectancy is very individual and depends on the stage, tumor biology, response to treatment and general condition; the doctor can most accurately discuss the prognosis after evaluating all the data and possible NSCLC treatment options.
Some patients with early, localized disease can be treated with long-term remission, but in general, small cell lung cancer is aggressive and often requires intensive systemic treatment and radiation therapy.
Treatment for non-small cell lung cancer begins with understanding the diagnosis: non-small cell lung cancer is the most common group of lung tumors, which includes several subtypes and is usually treated based on stage and biomarkers.
Small cell lung cancer is usually considered the most aggressive type of lung cancer because it grows faster and metastasizes more often early compared to many forms of NSCLC.
Survival rates depend on the stage and biology of the tumor: in early-stage NSCLC treatment can be potentially radical, and in advanced forms, results depend on the effectiveness of systemic treatment of NSCLC and personalized therapy selection.
In recent years, immunotherapeutic approaches in combination with systemic treatment have been increasingly used for small-cell lung cancer, but the specific strategy depends on the stage and clinical situation.
The rate of progression varies: it is influenced by the tumor subtype, the presence of mutations, the overall aggressiveness of the process and the initial stage, so individual diagnostics and a plan are always important to assess the pace NSCLC treatment options by stage.
Choose treatment abroad and you will surely get the best results!
Authors:
This article was edited by medical experts, board-certified doctors Dr. Nadezhda Ivanisova, and Dr. Daria Sukhoruchenko. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Our editorial policy, which details our commitment to accuracy and transparency, is available here. Click this link to review our policies.
Sources:
[1] Freddie Bray, Mathieu Laversanne, Hyuna Sung et al. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2024 May-Jun;74(3):229-263. doi: 10.3322/caac.21834. Epub 2024 Apr 4. [DOI] [PubMed]
[2] Hyun-Ji Oh, Abdulhamid B. Imam-Aliagan, Yeo-Bin Kim et al. Clinical applications of circulating biomarkers in non-small cell lung cancer. Front. Cell Dev. Biol., 21 August 2024. Sec. Cancer Cell Biology. Volume 12 - 2024. doi:10.3389/fcell.2024.1449232. [DOI]
[3] Rachel L Medbery, Theresa W Gillespie, Yuan Liu et al. Nodal Upstaging is More Common with Thoracotomy versus VATS During Lobectomy for Early Stage Lung Cancer: An Analysis from the National Cancer Data Base. J Thorac Oncol. Author manuscript; available in PMC: 2017 Feb 1. Published in final edited form as: J Thorac Oncol. 2016 Jan 11;11(2):222–233. doi: 10.1016/j.jtho.2015.10.007. [DOI] [PMC free article]
[4] Chi-Fu Jeffrey Yang, Zhifei Sun, Paul J Speicher et al. Use and Outcomes of Minimally Invasive Lobectomy for Stage I Non-Small Cell Lung Cancer in the National Cancer Data Base. Ann Thorac Surg. Author manuscript; available in PMC: 2017 Mar 1. Published in final edited form as: Ann Thorac Surg. 2016 Jan 26;101(3):1037–1042. doi: 10.1016/j.athoracsur.2015.11.018. [DOI] [PMC free article]
[5] Robert Timmerman, Rebecca Paulus, James Galvin et al. Stereotactic Body Radiation Therapy for Inoperable Early Stage Lung Cancer. JAMA. Author manuscript; available in PMC: 2010 Sep 1. Published in final edited form as: JAMA. 2010 Mar 17;303(11):1070–1076. doi: 10.1001/jama.2010.261. [DOI] [PMC free article]
[6] Mani Akhtari, Eric H Bernicker, Bin S Teh . Chemotherapy in non-small cell lung cancer: opportunities for advancement. Chin J Cancer. 2016 Jun 23;35:56. doi: 10.1186/s40880-016-0119-x. [DOI] [PMC free article]
[7] Juan Pablo Castañeda-González, Jonathan W Riess, María Paula Gómez-Gómez et al. Actionable mutations and targeted therapy in non-small cell lung cancer among Latin American and Hispanic patients: a systematic literature review of prognosis and meta-analysis. Transl Lung Cancer Res. 2025 Sep 28;14(9):3410–3429. doi: 10.21037/tlcr-2025-99. [DOI] [PMC free article]
[8] Ortega MA, Pekarek L et al. Updated Views in Targeted Therapy in the Patient with Non-Small Cell Lung Cancer. Journals. JPM. Volume 13. Issue 2. doi: 10.3390/jpm13020167. [DOI]
[9] Maria Anna Bareschino, Clorinda Schettino, Antonio Rossi et al. Treatment of advanced non small cell lung cancer. J Thorac Dis. 2011 Jun;3(2):122–133. doi: 10.3978/j.issn.2072-1439.2010.12.08. [DOI] [PMC free article]
[10] Roman Volchenkov, Florian Sprater, Petra Vogelsang, Silke Appel. The 2011 Nobel Prize in physiology or medicine. Scand J Immunol. 2012 Jan;75(1):1-4. doi: 10.1111/j.1365-3083.2011.02663.x. [DOI] [PubMed]
Read:
Comprehensive Guide to Lung Cancer: New and Standard Treatment Options
Dendritic Cell Immunotherapy for Non-Small Cell Lung Cancer
Top German Hospitals for Lung Cancer Treatment by Booking Health