Conventional treatment for pulmonary fibrosis offers limited hope — it slows progression but never reverses damage or restores lung function [1]. Dendritic cell immunotherapy is a novel approach that trains the immune system to eliminate the specific cells that cause lung scarring and protect healthy tissue. This approach works. Unlike traditional medications requiring daily dosing with significant side effects, dendritic cell therapy involves a single personalized treatment that can halt fibrosis progression and measurably improve breathing capacity. This paradigm shift — from damage control to genuine healing — suggests new possibilities for patients with end-stage disease (who previously faced almost zero options).
Understanding Pulmonary Fibrosis: The Challenge We Face
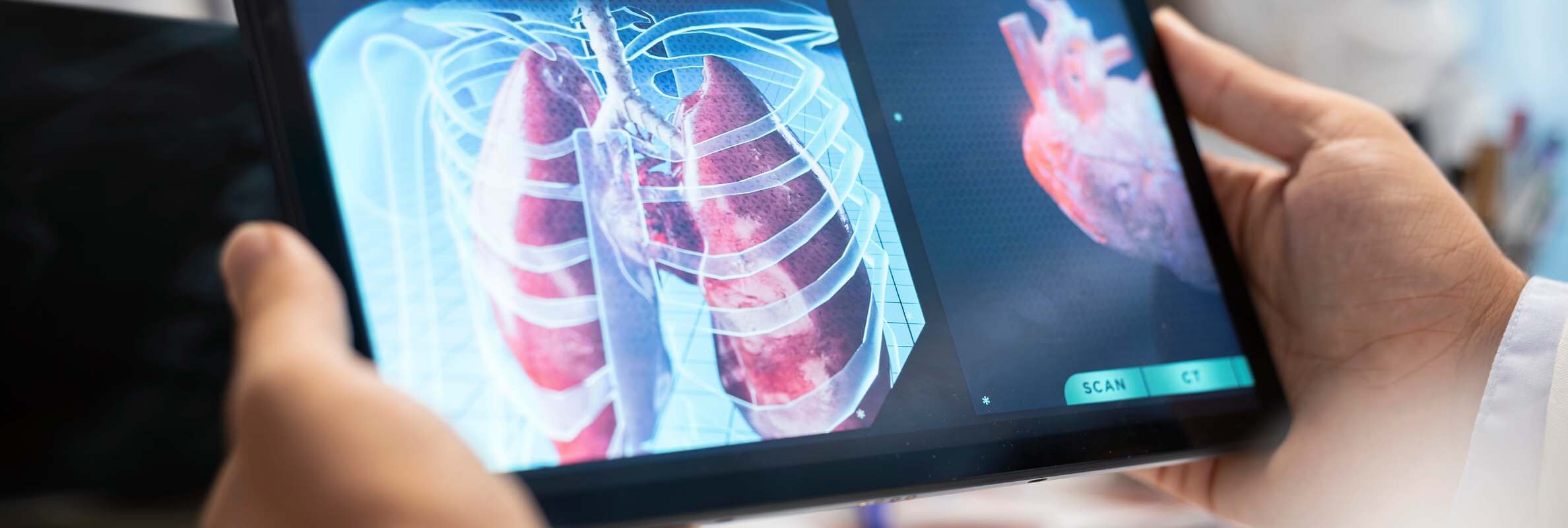
Pulmonary fibrosis is a progressive lung disease where healthy lung tissue is replaced by nonfunctional scars and this makes breathing increasingly difficult. The mechanism is self-reinforcing. Abnormal wound-repair signaling drives continuous collagen deposition at the alveolar level, creating a cycle of damage that compromises gas exchange and quality of life simultaneously [2]. Median survival sits at just 2–5 years from diagnosis, a figure that has remained largely unchanged across decades of research.
The disease primarily affects adults over 50, with idiopathic pulmonary fibrosis (IPF — the subtype in which no identifiable external cause can be established) representing the most clinically devastating form. Onset is deceptively gradual. What begins as a dry, persistent cough and mild shortness of breath can progress (within months!) to a level of impairment that transforms daily life.
The progressive impact on daily life includes:
- Simple activities like climbing stairs or walking become exhausting ordeals
- Conversation grows difficult — breathlessness interrupts speech, isolating patients socially and emotionally
- Supplemental oxygen dependence — continuous or exertional — often required within the first two years of diagnosis
- Loss of independence and the ability to perform routine tasks
- Anxiety and depression affecting patients and families
Lung transplantation is a definitive intervention. Yet organ scarcity means most patients are never listed. Add the economic weight — hospitalizations, oxygen infrastructure, and antifibrotic medications collectively exceeding $50,000 annually — and the picture becomes even harder. Pulmonary fibrosis currently affects 13–20 people per 100,000 globally [3], with prevalence rising as populations age. Genuinely curative approaches aren't just desirable. They're urgent.
Conventional Treatment Approaches for Pulmonary Fibrosis
Currently used methods applied widely are best understood as disease-modifying rather than curative. They slow, not stop. FDA-approved antifibrotic agents can reduce the rate of forced vital capacity (FVC) decline by approximately 50% in some patients [4], offering meaningful but clearly bounded benefit. No approved therapy reverses established scarring of lungs or restores lost lung architecture.
The fundamental limitation of current approaches lies in their mechanistic breadth — broad suppression of fibrotic activity rather than precision targeting of the cells driving it:
- Failure to address the root cause: overactivated fibroblasts that continuously deposit scar tissue
- Inability to eliminate cells already producing excessive collagen
- Repair pathway neglect — the lung's endogenous regenerative mechanisms remain unaddressed and unsupported
- Collateral impact — healthy tissue is affected alongside diseased tissue, limiting tolerable dosing
- Late-stage inadequacy
By the time most patients receive a diagnosis, significant and irreversible lung damage has occurred already. This diagnostic lag reflects the insidious onset of the disease. And current therapeutic paradigm, as we see, amounts to damage control rather than healing. This therapeutic gap has created demand for innovative approaches that can specifically target disease-causing cells and preserve healthy lung tissue.
The fundamental problems with conventional approaches include:
- Failure to address the root cause: overactivated fibroblasts that continuously deposit scar tissue
- Inability to eliminate cells already producing excessive collagen
- No restoration of the lung's natural repair mechanisms
- Broad effects on both diseased and healthy tissue
- No solution for patients with advanced disease
By the time most patients receive the diagnosis, significant lung damage has already occurred. The current therapeutic paradigm essentially amounts to damage control rather than true healing, leaving patients and physicians with limited options as the disease progresses. This therapeutic gap has created urgent demand for innovative approaches that can specifically target disease-causing cells while preserving healthy lung tissue.
Dendritic Cell Therapy for Pulmonary Fibrosis
The method moves from anti-inflammatory approaches with systemic action to immunotherapy that specifically targets the cells driving disease progression. The Nobel Committee acknowledged the role of dendritic cells in immunity functioning and awarded the 2011 Nobel Prize in Medicine to their discoverer — American immunologist Ralph Steinman [5].
Dendritic cell therapy works by training the immune system to recognize and attack specific disease-causing cells — unlike conventional medications that broadly suppress fibrotic processes. This targeted approach addresses the fundamental problem in pulmonary fibrosis: the persistence of cells that continuously deposit collagen and other scar tissue components.
The Science Behind Dendritic Cell Treatment for Pulmonary Fibrosis
The scientific foundation of dendritic cell therapy lies in training the immune system to fight lung scarring. Dendritic cells act as the body's "immune teachers," showing T-cells which specific targets to attack. In this treatment of pulmonary fibrosis, dendritic cells are programmed to recognize diseased lung tissue, creating a personalized vaccine against each patient's fibrosis.
The therapeutic target was identified through a key discovery. Scientists found that certain proteins — most notably ADAM12 and GLI1 — appear almost exclusively in scarred lung tissue while remaining virtually absent in healthy lungs [6], functioning as molecular fingerprints that distinguish pathological cells from normal ones. This specificity is what makes precision targeting possible.
Researchers proved that vaccinating against these scar-specific proteins could dramatically reduce lung damage — that was a breakthrough information. Studies showed remarkable results: vaccination led to significant decreases in both the troublemaking cells and the amount of scar tissue in diseased lungs.
This pulmonary fibrosis latest treatment mechanism works through interconnected steps:
- Dendritic cells present fibrosis-associated antigens to the immune system
- Cytotoxic T-cells become specifically programmed to recognize diseased cells
- Activated T-cells migrate to the lungs and systematically eliminate overactivated fibroblasts
- Healthy tissue — protected and unharmed
- Natural lung repair mechanisms are restored to normal function
Crucially, this approach appears to not only halt disease progression but also promote tissue regeneration. Research has shown that by eliminating excess fibrotic tissue mechanical stiffness that impairs normal lung cell function is reduced. As the tissue environment normalizes, the lung's capacity for self-repair is restored — these lead to improved cellular profiles and better oxygen exchange.
The Treatment Process: What Patients With Pulmonary Fibrosis Expect
Dendritic cell therapy follows a carefully structured protocol. Comprehensive initial evaluation includes complete blood count, liver and kidney function assessments, and additional specialized testing as indicated by individual patient profile — establishing the baseline necessary to manufacture an accurately personalized vaccine.
The most crucial step involves blood sampling for manufacturing the personalized dendritic cell vaccine. Approximately 50-100 ml of blood is collected from which the patient's own dendritic cells will be isolated and programmed. In some cases, if available, small tissue samples may also be utilized to enhance the specificity of the immune response. This entire initial phase is conducted on an outpatient basis, allowing patients to return home the same day.
Following blood collection, the patient's dendritic cells undergo sophisticated laboratory processing over 7-14 days. During this manufacturing period, the cells are isolated, cultured, and exposed to specific antigens associated with pulmonary fibrosis. This process (known as "loading") gives dendritic cells the ability to recognize and present fibrosis-associated proteins to the immune system. Each vaccine is individually prepared for the specific patient.
Treatment administration involves a defined set of steps, each managed at a specialized medical center with professional nursing support throughout:
- Outpatient procedure — conducted at a specialized center with no overnight admission required
- Subcutaneous injection — the personalized dendritic cell vaccine is administered via injection beneath the skin
- Immediate monitoring — post-treatment observation is conducted to assess and manage any acute reactions
- Symptom management — professional care is available for any post-treatment discomfort or side effects
- Follow-up scheduling — subsequent appointments are arranged based on individual treatment response and clinical need
The entire administration is completed within a single day. Patients typically experience minimal discomfort and can return to normal activities within 24–48 hours — a recovery profile that contrasts sharply with the ongoing burden of daily antifibrotic medication regimens.
Clinical Evidence and Results
Clinical findings suggest that dendritic cell vaccination can produce outcomes that conventional pulmonary fibrosis therapies have been unable to achieve. The results are specific. Research models targeting ADAM12 and GLI1 proteins demonstrated reductions in lung scarring of 60–80%, alongside measurable restoration of the immune system's capacity to eliminate disease-causing cells without affecting healthy tissue. These figures represent a meaningful departure from the modest FVC preservation offered by currently approved antifibrotic therapy.
Patients enrolled in studies experienced improvements across multiple dimensions of disease burden, each reflecting a different aspect of restored lung and immune function. Key outcomes point toward a pattern of functional recovery rather than stabilization alone.
Key improvements patients experienced include:
- Substantial improvements in breathing capacity
- Reduced cough severity and frequency
- Daily activity tolerance — enhanced ability to perform routine physical tasks without the breathlessness that previously made them prohibitive
- Exercise capacity — improved tolerance for exertion, indicating systemic oxygen exchange recovery beyond resting lung function
- Better overall quality of life scores
- Reduced need for oxygen supplementation
The safety profile further supports the therapeutic case. No significant organ damage was observed, and minimal impact on normal healing processes was recorded — an important distinction from broad immunosuppressants that compromise systemic immune function. IPF treatment appears most effective when initiated before extensive scarring has developed, which indicates that early intervention is clinically critical rather than merely preferable. For patients who previously faced only managed decline, these findings suggest a path toward measurable functional improvement — not simply a slower deterioration.
Integrated Pulmonary Fibrosis Treatment Strategies
Dendritic cell therapy in combination with anti-fibrotic drugs allows the creation of powerful personalized PF treatment plans. Conventional medications slow down lung scarring, immunotherapy targets and eliminates the specific cells the damage is caused by. As obvious, such a strategy addresses the symptoms and the root cause of the disease.
Some patients benefit from both therapies together, others do better with treatments given in sequence. A medical team creates the most effective plan for the specific situation:
- Disease severity, progression rate
- Patient age and overall health status (additional examinations may be required)
- As follows, comorbid conditions that affect treatment choices
- Patient preferences and lifestyle factors — options provided by specialized clinics
- Previous treatment responses and tolerability
The approach guarantees attention to health and emotional well-being. To address every aspect, pulmonologists, specialists in the field of immunotherapy, respiratory therapists, and even support groups work together.
| Characteristic | Standard Treatment | Standard Treatment + Dendritic Cell Vaccine |
|---|---|---|
| Treatment Mechanism | Broad anti-fibrotic suppression | Targeted elimination of disease-causing cells |
| Treatment Approach | One-size-fits-all protocol | Personalized immunotherapy |
| Disease Progression | Slows progression moderately | Halts progression and promotes tissue repair |
| Treatment Duration | Continuous daily medication | Single outpatient procedure + follow-up |
| Side Effects | Significant GI, liver, and skin reactions | Minimal, temporary immune responses |
| Oxygen Dependency | Often increases over time | May reduce or eliminate the need |
| Life expectancy | Extends life by several months | Potential for significant life extension |
*Data from Booking Health clinical analysis. Treatment outcomes may vary based on individual patient factors, disease severity, and timing of intervention. Consult with our lung specialists for personalized treatment planning and comprehensive care coordination.
Pulmonary Fibrosis Patient Success Story: Francis's Journey
Francis Bekele's case illustrates what becomes possible when precision immunotherapy is applied where conventional approaches have already been exhausted. At 43, this mining company worker from Accra, Ghana, faced a condition that threatened not only his livelihood but his capacity to perform the most basic physical tasks. The disease had not arrived without cause. Living and working near active mining operations, Francis developed pulmonary fibrosis complicated by pneumothorax in 2018 — a combination in which occupational dust exposure accelerated a fibrotic process that standard medical intervention in Ghana was unable to slow.
Despite treatment with corticosteroids and antibiotics over a two-year period, Francis continued experiencing severe breathlessness, chronic cough, chest pain, and fatigue that made short walks impossible. He was hospitalized at Agogo Presbyterian Hospital on five or six separate occasions, with no measurable improvement in functional capacity between admissions. The turning point came through an indirect route. A friend based in the UK, familiar with the international latest treatment for pulmonary fibrosis, connected Francis with a specialized center in Germany — where he received dendritic cell therapy targeting the underlying immune dysfunction driving his fibrosis.
The reported transformation has been substantial. Francis describes his current condition as approximately 80–90% recovered — able to walk distances without significant breathlessness, perform daily tasks independently, and return to work. Before treatment, supplemental oxygen had been required for even minimal exertion. Thus, dendritic cell therapy can offer functional recovery in patients for whom conventional medicine had effectively reached its ceiling.
Looking Forward: Hope and Realistic Expectations in Pulmonary Fibrosis
End-stage pulmonary fibrosis has historically carried an implicit message: options are running out. That message, understandable given the disease's progression patterns, is increasingly outdated. Dendritic cell immunotherapy, stem cells in medicine research, and personalized combination protocols are all advancing — often faster than the prognostic frameworks built a decade ago can accommodate.
Standard anti-fibrotic therapy continues to benefit a defined patient population. But resistance develops. Over time, conventional approaches lose efficacy in ways that precision immunotherapy is specifically engineered to overcome — targeting the immune dysfunction driving fibrosis rather than simply moderating its effects.
The practical profile reinforces the clinical case. No extended hospitalization. Outpatient visits only. A side-effect burden meaningfully lower than that of conventional anti-fibrotic regimens — which means effective idiopathic pulmonary fibrosis treatment need not come at the cost of systemic wellbeing. Francis Bekele's case documents one version of this potential. The broader clinical evidence points in the same direction.
At Booking Health, every patient's situation is treated as clinically distinct. Pulmonologist expertise is combined with immunotherapy consultation to build plans calibrated to individual disease profile, health status, and therapeutic history. Even in the most challenging cases — especially those — a path forward can be identified. The role of specialized coordination is simply to make that path navigable.
Your Trusted Partner: Every Step of the Way With Booking Health
Finding the best treatment strategy for your clinical situation is a challenging task. Being already exhausted from multiple treatment sessions, having consulted numerous specialists, and having tried various therapeutic interventions, you may be lost in all the information given by the doctors. In such a situation, it is easy to choose a first-hand option or to follow standardized therapeutic protocols with a long list of adverse effects instead of selecting highly specialized innovative treatment options.
To make an informed choice and get a personalized treatment plan, which will be tailored to your specific clinical situation, consult medical experts at Booking Health. Being at the forefront of offering the latest medical innovations for 12 years, Booking Health possesses solid expertise in creating complex therapeutic programs in each case. As a reputable company, Booking Health offers personalized pulmonary fibrosis treatment plans with direct clinic booking and full support at every stage, from organizational processes to assistance during treatment. We provide:
- Assessment and analysis of medical reports
- Development of the medical care program
- Selection of a suitable treatment location
- Preparation of medical documents and forwarding to a suitable clinic
- Preparatory consultations with clinicians for the development of medical care programs
- Expert advice during the hospital stay
- Follow-up care after the patient returns to their native country after completing the medical care program
- Taking care of formalities as part of the preparation for the medical care program
- Coordination and organization of the patient's stay in a foreign country
- Assistance with visas and tickets
- A personal coordinator and interpreter with 24/7 support
- Transparent budgeting with no hidden costs
Health is an invaluable aspect of our lives. Delegating management of something so fragile yet precious should be done only to experts with proven experience and a reputation. Booking Health is a trustworthy partner who assists you in pursuing stronger health and a better quality of life. Contact our medical consultant to learn more about the possibilities of personalized treatment with innovative methods for pulmonary fibrosis with leading specialists in this field.
Dendritic Cell Therapy: Patient Stories with Booking Health
FAQ About Pulmonary Fibrosis Answered
Send request for treatmentThis is a disease of the lungs in which healthy tissue is replaced by scar tissue. Causes are environmental toxins, medications, family history of genetic changes, etc. And in many patients, despite thorough testing, no clear trigger appears.
Symptoms worsen over time — as lung function declines. These are cough (persistent, dry), shortness of breath during activity, fatigue, chest discomfort, and gradual weight loss.
Although a cure is not that likely to happen, innovative treatment of idiopathic pulmonary fibrosis (dendritic cell therapy, stem cell treatments) can halt progression and improve lung function. They offer hope beyond conventional approaches.
Antifibrotic medications, oxygen concentrator therapy, pulmonary rehabilitation, and innovative approaches like dendritic cell immunotherapy are available options. Treatment for idiopathic pulmonary fibrosis is personalized: based on disease severity and patient needs.
The distinction comes down to cause. Idiopathic lung fibrosis is a form of interstitial lung disease with an unknown cause. And typically worse prognosis. Other types have identifiable causes — like occupational exposures, medications, autoimmune conditions.
Lung transplant is considered for patients under 65 with advanced disease who remain healthy enough for surgery. Limited organ availability means most patients never receive transplants and that is why new treatment for pulmonary fibrosis is crucial.
Yes. Oxygen therapy helps maintain adequate oxygen saturation levels. It reduces strain on the heart and improves QoL. Many patients use portable oxygen during activities or continuous oxygen — as the disease progresses.
Progression varies significantly. Some patients experience rapid decline within months, others have slower progression over years. Regular monitoring helps track changes — and adjust treatment options for pulmonary fibrosis.
Life expectancy varies widely depending on disease type and severity. IPF typically has 2-5 year median survival from diagnosis. Some patients live far longer than early estimates suggest. Prognosis informs decisions — it doesn’t define destiny.
Traditional lung fibrosis treatment cannot achieve remission. But breakthrough therapies like dendritic cell immunotherapy have shown potential to halt progression and even restore lung function.
Yes, new pulmonary fibrosis treatment — including dendritic cell therapy and stem cells — is available. Booking Health can provide information about accessing these options.
Spirometry and pulmonary function tests are typically performed every 3-6 months, to monitor disease progression. HRCT scans may be done annually — or when symptoms change significantly — to assess lung tissue changes.
Fibrosis of lung is serious and progressive, but innovative pulmonary fibrosis treatment guidelines change outcomes. Pulmonary rehabilitation and respiratory therapy combined with newer immunotherapies offer hope for extended survival and improved quality of life.
In stage 4 pulmonary fibrosis, antifibrotic drugs, immunosuppressants and innovative methods 一 dendritic cell therapy, for example. It allows the immune system to destroy the cells that cause fibrosis, stopping the progression of the disease and stimulating the natural regeneration of lung tissue.
The cost of dendritic cell therapy for pulmonary fibrosis in Germany is on average €20,000–38,000 depending on the individual program and combination with other methods. In the UK and the USA prices are usually higher, while in Australia this method is currently only available in a few clinics, mainly within the framework of clinical trials.
Compared to standard treatment which only slows the progression of fibrosis dendritic cell therapy not only stops the progression but also promotes the regeneration of lung tissue. Patients show improved respiratory function, reduced cough and less dependence on oxygen support.
Clinical data show that patients who receive dendritic cell therapy in the early and middle stages have a significantly improved prognosis. While standard drugs prolong life by a few months innovative treatment can provide a significant increase in lifespan by reducing fibrotic lesions by up to 60–80%.
How does the mechanism of action of standard treatment differ from dendritic cell vaccine in stage 4 pulmonary fibrosis?
Standard therapy reduces inflammation in general but does not affect the cells that produce scar tissue. Dendritic cell vaccine works in a targeted manner — it activates T-cells that destroy pathological fibroblasts, preserving healthy tissue and promoting its self-repair.
Antifibrotic drugs often cause side effects in the gastrointestinal tract, liver and skin. In contrast, dendritic cell therapy is much better tolerated — only short-term immune reactions are possible, without organ damage or a long recovery period.
Yes, some patients experience a decrease in oxygen demand after therapy. Restoring natural breathing mechanisms and lung tissue elasticity allows for improved blood oxygen saturation and improved overall quality of life, even in stage 4 of the disease.
Germany is recognized for pulmonary fibrosis care (especially when advanced therapies like dendritic cell treatment are considered). Hospitals there combine close respiratory monitoring with specialized immunotherapy programs — ensuring patients receive personalized treatment.
Choose treatment abroad and you will for sure get the best results!
Authors:
This article was edited by medical experts, board-certified doctors Dr. Nadezhda Ivanisova, and Dr. Bohdan Mykhalniuk. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Our editorial policy, which details our commitment to accuracy and transparency, is available here. Click this link to review our policies.
Sources:
[1] American Lung Association. How Is Pulmonary Fibrosis Treated? https://www.lung.org/lung-health-diseases/lung-disease-lookup/pulmonary-fibrosis/patients/how-is-pulmonary-fibrosis-treated
[2] Pulmonary Fibrosis Foundation. What is Pulmonary Fibrosis? https://www.pulmonaryfibrosis.org/understanding-pff/about-pulmonary-fibrosis/what-is-pulmonary-fibrosis
[3] MedlinePlus. Idiopathic pulmonary fibrosis. https://medlineplus.gov/genetics/condition/idiopathic-pulmonary-fibrosis/
[4] Luca Richeldi, Huw Richard H R Davies, Paolo Spagnolo, Fabrizio Luppi. Corticosteroids for idiopathic pulmonary fibrosis. Cochrane Database Syst Rev. 2003 Jul 21;2003(3):CD002880. doi: 10.1002/14651858.CD002880 [DOI] [PMC free article]
[5] Roman Volchenkov, Florian Sprater, Petra Vogelsang, Silke Appel. The 2011 Nobel Prize in physiology or medicine. Scand J Immunol. 2012 Jan;75(1):1-4. doi: 10.1111/j.1365-3083.2011.02663.x. [DOI] [PubMed]
[6] Science Direct. Turning the tide: From fibrosis to regeneration following anti-fibrogenic cell vaccination. https://www.sciencedirect.com/science/article/pii/S1934590922003848
[7] Jing Yan, Song-Yu Wang2, Qi Su 1, Min-Wen Zou 1, Zi-Yue Zhou 1, Jian Shou 1 2, Yunlong Huo. Targeted immunotherapy rescues pulmonary fibrosis by reducing activated fibroblasts and regulating alveolar cell profile. Nat Commun. 2025 Apr 21;16(1):3748. doi: 10.1038/s41467-025-59093-7. [DOI] [PubMed]
Read:
Pulmonary sarcoidosis therapy: combining drugs with non-drug treatment options