Living with small intestine cancer can be difficult, but it leaves reason for optimism. Despite the rarity of this disease, more therapeutic options are available today than ever before. With timely and correct treatment, the five-year survival rate in the early stages can exceed 80%, which highlights the importance of specialized care.
Surgery, chemotherapy, and radiation therapy remain the basis of small intestine cancer treatment. At the same time, modern methods such as HIPEC, PIPAC, TACE, and immunotherapy significantly expand the possibilities of disease control and affect treatment results [1].
Do not limit yourself to the initial forecast. Consultation with specialists who apply innovative approaches to the treatment of small intestine cancer can improve the quality of life and increase the chances of longer survival.
The Hidden Difficulty: What You Should Know About Small Bowel Cancer?
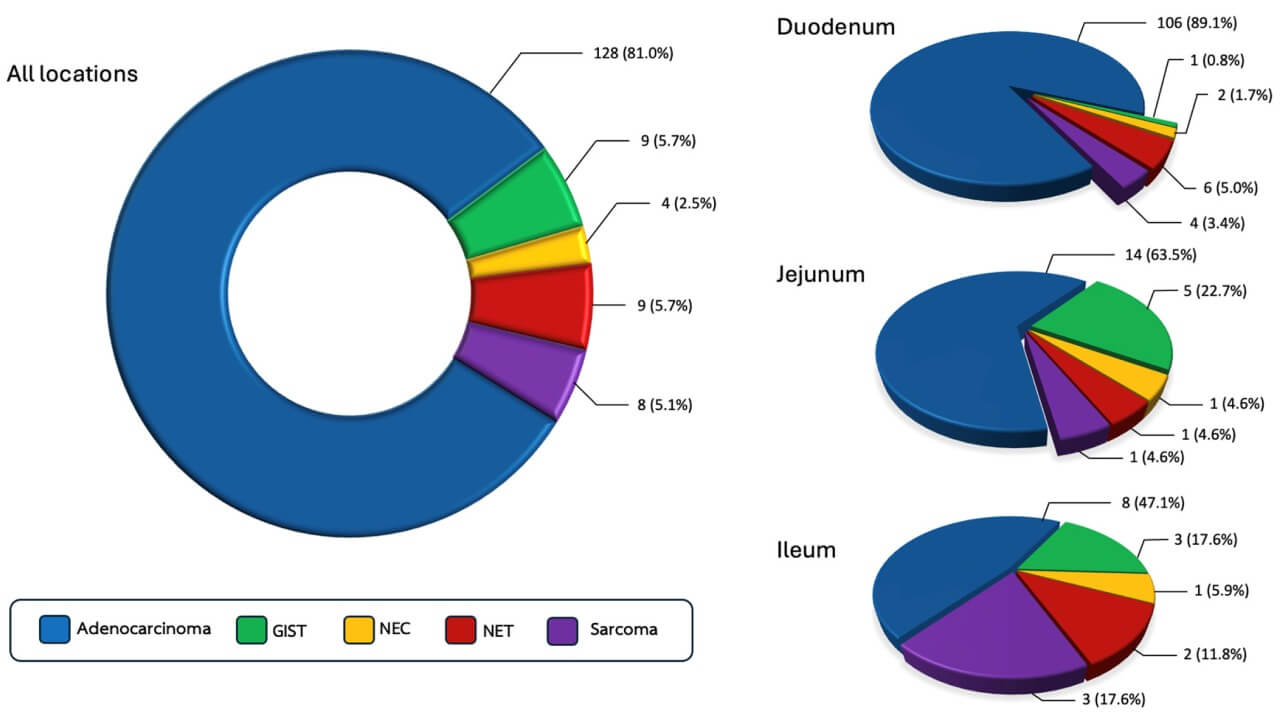
Small bowel cancer is a rare but clinically difficult disease that accounts for only 3-5% of all malignant tumors of the gastrointestinal tract, although the small intestine occupies about 90% of its area. Such a discrepancy makes it difficult to detect each tumor on time and choose the optimal treatment tactics.
The main types of small bowel cancer include:
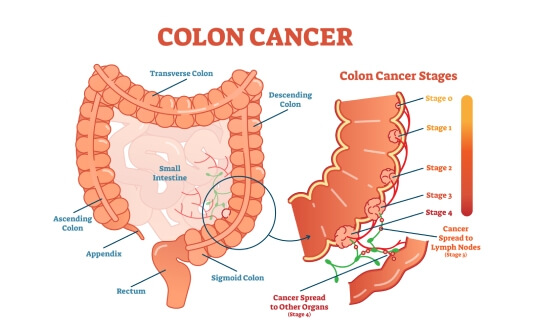
- Adenocarcinoma is one of the most common variants, usually localized in the duodenum and developing from glandular cells; biologically partially similar to colorectal cancer.
- Neuroendocrine tumors mainly arise in the ileum from hormone-producing cells.
- Lymphomas affect the lymphatic tissue of the small intestine.
- GIST (stromal tumors) are formed from Cajal interstitial cells.
- Sarcomas – rare tumors of muscle origin [2].
Diagnosis is often delayed due to non-specific symptoms: abdominal pain, weight loss, occult bleeding. The prognosis depends significantly on the stage: with early detection and timely small intestine cancer treatment, the five-year survival rate can exceed 80%, while with lymph node damage, it decreases to about 40%.
Basic Approaches to Treatment of Cancer of The Small Bowel: Surgery, Chemotherapy, and Radiation Therapy
Traditional treatments of small bowel cancer remain the basis of therapy, although they have certain limitations, especially in late stages of the disease.
Surgery
Surgery is the main treatment for a localized process.
- It involves segmental resection of the affected area together with the adjacent mesentery.
- For tumors of the proximal duodenum, Whipple surgery may be indicated.
- Limitations: complex anatomy of the digestive tract and the impossibility of surgery in cases of metastatic process, in particular with small bowel cancer stage 4.
Chemotherapy
Chemotherapy is used for small bowel cancer in two main situations:
- as palliative treatment in patients with inoperable tumours or distant metastases;
- as adjuvant therapy after radical surgery to reduce the risk of recurrence [3].
It may be accompanied by significant side effects that affect the quality of life of patients.
Radiation Therapy
- It is used less often due to the difficulty of safe irradiation of the abdominal organs.
- Can be used in certain localized cases.
- There is currently limited evidence base on its impact on survival.
Although these approaches are the standard treatment for cancer of the small bowel, their possibilities are limited in advanced stages of the disease or in the appearance of nonspecific symptoms in the later stages. That is why an important role is played by the consultation of an experienced specialist and the introduction of innovative methods of therapy that can expand the possibilities of treatment.
HIPEC in Cancer of the Small Intestine: Heated Chemotherapy in the Abdomen
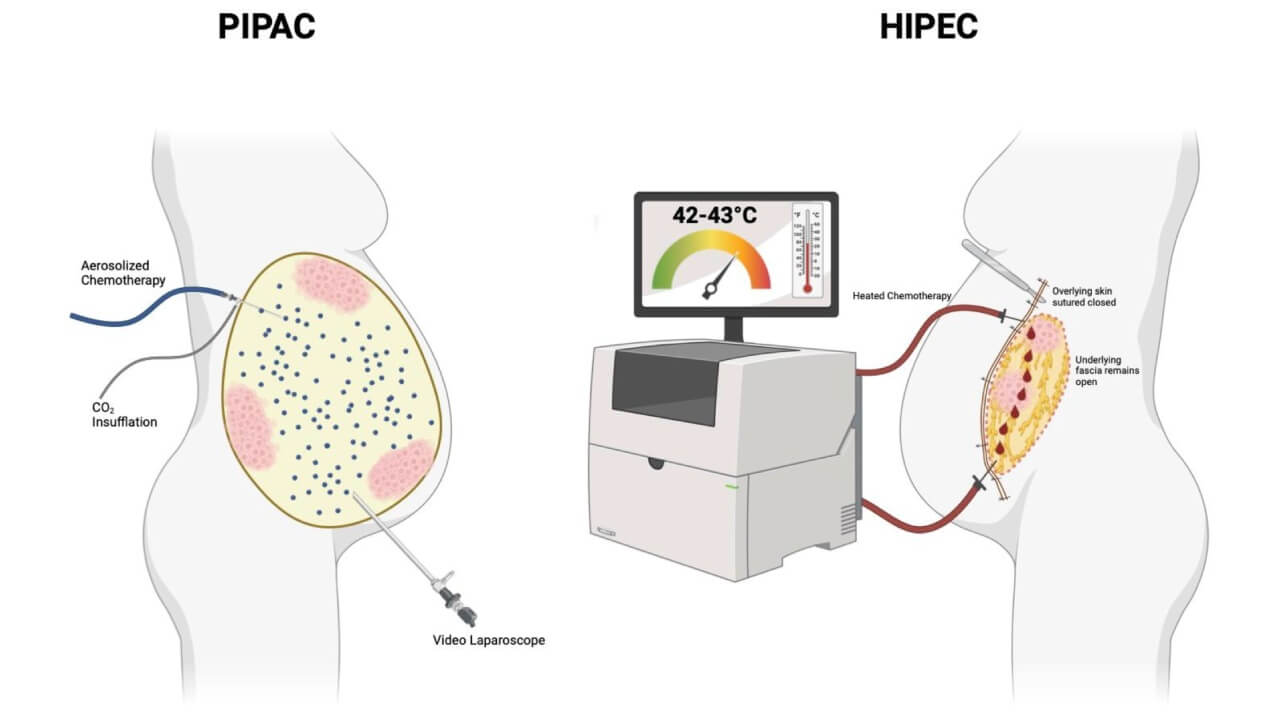
Hyperthermic intraperitoneal chemotherapy (HIPEC) is a modern method of small intestine cancer treatment, which is used for peritoneal metastases. Previously, this condition was considered almost incurable, but the combination of cytoreductive surgery with local heated chemotherapy changed the approaches to cancer of the small intestine treatment.
The Main Advantages of HIPEC
- creates a concentration of chemotherapy in the abdominal cavity up to 15 times higher than with systemic therapy;
- destroys microscopic cells of cancer in small intestine that cannot be removed during surgery;
- heat (40-43°C) enhances the penetration of drugs into tumor tissues;
- reduces systemic side effects;
- opens up additional treatment opportunities for patients with advanced cancer of the small intestine [4].
Stages of the Procedure
HIPEC begins with cytoreductive surgery (CRS), in which surgeons remove all visible tumor tissue in the abdomen. After that, special drains are installed, through which the heated chemotherapy solution circulates. The drug rinses the abdominal cavity evenly for 60-90 minutes, reaching even those areas of the bowel where microscopic tumor cells can remain. The entire procedure lasts about 5-10 hours, and postoperative recovery takes about 10-14 days.
Results and Clinical Data
Studies show that combining CRS and HIPEC can significantly improve treatment outcomes. In patients with peritoneal metastases, the median survival may be about 30-35 months, and in some cases – even longer. Similar approaches are also actively used in peritoneal metastases of colorectal cancer and other tumors, including adenocarcinoma of the digestive tract.
Prognosis largely depends on the extent of tumor spread, which is assessed by the Peritoneal Carcinomatosis Index (PCI). A lower volume of bowel lesions is associated with better treatment outcomes.
Usually, the path to such therapy begins with accurate diagnosis – endoscopy, imaging techniques and biopsy, especially if the patient develops symptoms such as abdominal pain or bleeding from the digestive tract.
HIPEC complements traditional surgery by allowing not only the removal of visible tumor, but also the impact of invisible cells of cancer in small intestine, making this method one of the most promising current treatment approaches [5].
Dr. Michael Lipp, a leading specialist and the head physician of the Department of Abdominal and Colorectal Surgery, explains what HIPEC is, what types of cancer this method is used for, and how the procedure itself goes. He also talks about the selection of patients, preparation for surgery, possible risks, duration of treatment, and features of recovery after the intervention.
"HIPEC Treatment: A Breakthrough in Advanced Abdominal Cancer Care" - Interview with Dr. Michael Lipp
PIPAC in Cancer of the Small Bowel: Local Chemotherapy Under Pressure
Patients with cancer of the small bowel, especially in advanced stages, can today access an innovative treatment approach – PIPAC (pressurized intraperitoneal aerosol chemotherapy). This technology belongs to modern small intestine cancer treatments and allows doctors to deliver chemotherapy directly into the abdominal cavity without large-scale surgery. During the procedure, the drug turns into a small aerosol under pressure, which helps it penetrate better into tumor tissues.
The procedure is performed laparoscopically. The surgeon makes two small incisions in the abdominal wall, through which special equipment is inserted. The chemotherapy is sprayed as an aerosol and circulated in the abdomen for approximately 30 minutes, after which it is removed. The entire procedure usually lasts 60-90 minutes, and the hospital stay is 2-3 days.
The Main Advantages of PIPAC
- Minimally invasive method with two small incisions
- Ability to repeat treatment every 6-8 weeks
- Can be combined with systemic chemotherapy
- Less physical damage than with HIPEC
- Shorter hospitalization
- Can be used as a transitional stage of treatment before other methods
PIPAC is particularly useful in patients with advanced peritoneal metastases, particularly in small bowel cancer stage 4, when radical surgery or HIPEC may not be possible. Due to the even distribution of chemotherapy on the peritoneum, the method influences the microscopic tumor cells and expands the possibilities of treatment in advanced cancer of the small bowel [6].
TACE for Cancer of the Small Intestine: Target Therapy for Metastasis in the Liver
For patients with small intestine cancer stage 4, when the tumor spreads to the liver, transarterial chemoembolization (TACE) may be an effective treatment for small intestine cancer. This method delivers chemotherapy directly to metastases, minimizing the effects on healthy tissues.
During the procedure, the interventional radiologist inserts a thin catheter into the large artery of the arm or leg and, under X-ray control, conducts it to the vessels that feed the tumor in the liver. A mixture of chemotherapy drugs and special embolization materials that block the blood supply to the tumor is injected through the catheter.
This approach has a dual mechanism of action:
- high local concentrations of chemotherapy (several times higher than with systemic treatment) directly affect tumor cells;
- blocking blood flow deprives the tumor of oxygen and nutrients and at the same time keeps the drug in the affected area longer.
Benefits of TACE for Patients
- smaller systemic side effects compared to traditional chemotherapy;
- targeted effect on liver metastases;
- minimally invasive procedure with recovery usually within 24-48 hours;
- possibility of usage in patients who cannot tolerate major operations;
- combination with other methods of treatment for small intestine cancer.
TACE is used in various small intestine cancer types, especially when the disease is metastatic and standard surgery is not possible. It helps control tumor growth and improve patients' quality of life [7].
Prof. Dr. Attila Kovács, chief physician of interventional radiology, talks about the possibilities of transarterial chemoembolization (TACE) and modern approaches of interventional oncology. In the conversation, he explains which types of TACE are used today (conventional TACE, DEB-TACE, TARE) and how they differ in clinical practice, for which tumors this method is considered as the standard of treatment and which has limitations. It is also discussed how physicians choose the optimal treatment option for each patient, what role imaging techniques (CT, MRI, DSA) play in treatment planning and control, and in which cases TACE is combined with other local or systemic therapies.
Prof. Kovács: Why TACE Doubled Cancer Survival – What Patients Need to Know
Use of the Immune System: Dendritic Cell Therapy for Small Bowel Cancer
Dendritic cell therapy is one of the modern areas of immunotherapy, which can be used for rare tumors of the digestive tract, in particular for small intestine cancer. This approach activates the patient's immune system to recognize and destroy tumor cells throughout the body, especially in cases where standard treatments have already been exhausted. This immunotherapeutic approach is actively being investigated in other tumors of the digestive system, in particular dendritic cell therapy for colon cancer, which demonstrates promising results in patients with tumors of the gastrointestinal tract. The role of dendritic cells in antitumor immunity is of fundamental importance for modern immunotherapy and was awarded the Nobel Prize in Physiology or Medicine in 2011 [11].
The essence of the method is to "train" immune cells to fight the tumor. Firstly, dendritic cells are obtained from the patient's blood by a procedure similar to blood donation. In the laboratory, they are programmed to recognize the proteins of a specific tumor, after which the cells are returned to the patient's blood. They activate T-lymphocytes, which search for and destroy tumor cells throughout the body [10].
The Main Advantages of the Method
- Personalized treatment adapted to each patient's tumor biology
- Fewer side effects compared to chemotherapy or radiotherapy
- Can be used together with other methods, including tumor resection or targeted therapy
- Potential assistance in controlling the metastatic process
- Better tolerability of treatment and faster recovery compared to aggressive methods
- The ability to reduce the risk of recurrence thanks to the formation of an antitumor immune response
DC vaccination is actively being investigated as part of immunotherapy for bowel cancer, including colon cancer treatment and rectal cancer treatment, as well as in some rare tumors, such as sarcoma.
Modern cancer centers are improving this technology for tumors of the gastrointestinal tract. Patients note stabilization of the disease, reduction of tumor burden and improvement of quality of life.
Prof. Gansauge, head of a clinic specializing in innovative dendritic cell therapy, talks about this method, the principle of its action and the possibilities of application in modern oncology. The conversation discusses how this therapy is combined with other treatments, what results it can produce, and its potential in the field of anti-aging medicine.
"Every Patient Deserves an Individual Approach": Interview with Renowned German Immunologist Prof. Gansauge
Minimally Invasive Methods of Treatment for Small Bowel Cancer
Modern cancer in small intestine treatment increasingly includes minimally invasive technologies that destroy malignant tumors without major operations. Such methods are particularly useful for patients with limited metastasis, such as in the liver, or with single tumors. They provide an accurate effect on the tumor, a lower risk of complications and faster recovery.
Thermal Destruction of Tumors: Radiofrequency and Microwave Ablation
Radiofrequency ablation (RFA) involves inserting a thin needle directly into the tumor under imaging control. A high-frequency current is supplied through it, which creates a heat of 60-100°C, which destroys cancer cells. The procedure usually lasts 10-15 minutes and allows doctors to treat tumors up to 5 cm, after which the patient can often return home the same day.
Microwave ablation (MWA) uses electromagnetic energy to heat and destroy tumor tissue. This technology is effective even in areas with high blood flow and allows multiple tumors to be treated simultaneously.
Advantages of these methods:
- short recovery period compared to surgery;
- preservation of healthy tissues around the tumor;
- lower risk of complications than after surgical resection;
- possibility of usage in patients with impaired liver function;
- the possibility of repeated treatment when new tumors appear.
Similar technologies are used for other tumors of the digestive tract, including lymphoma.
Cryoablation: Destruction of the Tumor by Cold
Cryoablation uses extremely low temperatures to destroy tumors in patients with cancer of small intestine. Under the control of imaging, special probes are inserted into the tumor, which quickly cool to a temperature below -75°C. An "icy ball" forms in the tissue, which destroys cell membranes and triggers the death of cancer cells.
Usually, the procedure involves a cycle of freezing, thawing and re-freezing to ensure complete destruction of the tumor.
Advantages of cryoablation:
- clear visualization of the treatment area during the procedure;
- precise boundaries between treated and healthy tissue;
- minimal pain after intervention;
- the possibility of treating tumors next to important structures, such as blood vessels;
- effectiveness for tumors up to 4 cm.
For patients with localized tumors or limited metastasis, these techniques can become an important part of treatment of cancer in small intestine, controlling disease with minimal impact on healthy tissues.
| Characteristic | Standard Treatment | Innovative Methods |
|---|---|---|
| 2-Year Survival Rate | ~25% for advanced cancer | ~60% for advanced cancer |
| Response Rate | Less than 10% | 45-65% |
| Treatment Duration | Several cycles over months | Up to 4 sessions |
| Side Effects | Severe (nausea, fatigue, hair loss, immunosuppression, skin irritation) | Mild (localized pain) |
| Cost in Germany | €80,000 - €150,000 full course | €25,000 - €60,000 full course |
| Cost in Great Britain | €90,000 - €165,000 full course | €70,000 - €120,000 full course |
| Cost in the USA | €100,000 - €180,000 full course | €100,000 - €150,000 full course |
*Booking Health data. Costs may vary based on case complexity, hospital stay duration, required follow-up care, and additional expenses such as diagnostics, travel, and accommodation.
From Diagnosis to Modern Treatment of Small Bowel Cancer: the Patientʼs Story
After the first operation and a course of chemotherapy, David received news that changed the course of his treatment: control examinations showed the development of peritoneal carcinomatosis. "My oncologist said that there are not many opportunities left for further therapy", – he recalls. "Then my wife started looking for specialized clinics abroad".
A few days after contacting the international coordinator Booking Health, David's medical documents were reviewed by German specialists. They proposed a combined PIPAC treatment program along with dendritic cell therapy, methods that were not available in his country.
"The first PIPAC procedure turned out to be much simpler than I expected", – says David. "After three procedures in combination with dendritic cell vaccination, control scans showed a noticeable reduction in the tumor, and the level of tumor markers returned to normal".
Later, David was able to return to his usual life. "What surprised us the most was that these innovative methods complemented standard treatment well and at the same time produced significantly fewer side effects. I got not only time, but also new hope".
Advanced Cancer Treatment: Patient Success Stories with Booking Health
Hope Thanks to Innovative Methods of Treating Small Bowel Cancer
The diagnosis of stage 4 small bowel cancer is often accompanied by the phrase that "treatment options are limited". However, modern medical technologies open up new opportunities where traditional approaches have limited effectiveness.
Today, specialized centers around the world offer stage 4 small intestine cancer patients modern techniques that can help to control the disease, improve the quality of life, and prolong survival beyond initial prognoses. Among such approaches:
- personalized dendritic cell therapy for colon or small intestine cancer that activates the immune system against tumor cells;
- PIPAC technology that delivers chemotherapy directly to peritoneal metastases;
- HIPEC procedure combining surgery with heated intra-abdominal chemotherapy;
- minimally invasive ablation methods for the treatment of single metastases;
- TACE for the precise treatment of liver metastases.
Unlike traditional methods, which are often accompanied by significant side effects and prolonged hospitalization, many innovative procedures require a short stay in the clinic and are associated with a lower risk of complications. While not seen as a complete cure, such approaches can provide better disease control and improve quality of life.
It is important to contact specialists who work with these modern methods of treatment. Even with stage 4 small bowel cancer, innovative approaches can significantly change the possibilities of therapy.
A Medical Journey: Every Step of the Way With Booking Health
Finding the best treatment strategy for your clinical situation is a challenging task. Being already exhausted from multiple treatment sessions, having consulted numerous specialists, and having tried various therapeutic interventions, you may be lost in all the information given by the doctors. In such a situation, it is easy to choose a first-hand option or to follow standardized therapeutic protocols with a long list of adverse effects instead of selecting highly specialized innovative treatment options.
To make an informed choice and get a personalized cancer management plan, which will be tailored to your specific clinical situation, consult medical experts at Booking Health. Being at the forefront of offering the latest medical innovations for already 12 years, Booking Health possesses solid expertise in creating complex cancer management programs in each case. As a reputable company, Booking Health offers personalized small bowel cancer treatment plans with direct clinic booking and full support at every stage, from organizational processes to assistance during treatment. We provide:
- Assessment and analysis of medical reports
- Development of the medical care program
- Selection of a suitable treatment location
- Preparation of medical documents and forwarding to a suitable clinic
- Preparatory consultations with clinicians for the development of medical care programs
- Expert advice during the hospital stay
- Follow-up care after the patient returns to their native country after completing the medical care program
- Taking care of formalities as part of the preparation for the medical care program
- Coordination and organization of the patient's stay in a foreign country
- Assistance with visas and tickets.
- A personal coordinator and interpreter with 24/7 support
- Transparent budgeting with no hidden costs
Health is an invaluable aspect of our lives. Delegating management of something so fragile yet precious should be done only to experts with proven experience and a reputation. Booking Health is a trustworthy partner who assists you on the way of pursuing stronger health and a better quality of life. Contact our medical consultant to learn more about the possibilities of personalized treatment with innovative methods for small bowel cancer with leading specialists in this field.
Frequently Asked Questions About Small Bowel Cancer Treatment
Send request for treatmentSmall bowel cancer is a malignant tumor that develops in the small intestine (duodenum, jejunum, and ileum). The five main types include adenocarcinoma, neuroendocrine tumors (including carcinoid), lymphoma, gastrointestinal stromal tumors, and sarcoma.
The exact etiological factor has not been established. Notable risk factors include genetic syndromes (FAP, Lynch syndrome), Crohn's disease, celiac disease, and excessive alcohol consumption. Prolonged inflammation of the mucous membrane can cause cellular changes that eventually lead to malignant transformation.
Small bowel cancer is much less common, although this organ occupies about 90% of the length of the gastrointestinal tract. It is not uncommon for it to be detected in later stages, and treatment approaches differ from protocols for colorectal cancer. In addition, small bowel cancer is characterized by a higher proportion of non-adenocarcinoma tumors.
The most common manifestations are abdominal pain, weight loss, weakness, hidden bleeding with the development of anemia, nausea and vomiting. In the later stages, the development of intestinal obstruction is possible, which is accompanied by intense pain, gas retention and the absence of bowel movements.
Examination usually involves endoscopic techniques, imaging (particularly CT-scans), and morphological confirmation by biopsy. If ileal tumors are suspected, colonoscopy with ileal intubation may be performed. In some cases, the tumor is detected during an operation performed for another pathology.
It is a rare cancer: in the USA, it accounts for about 0.6% of all new cancer cases. Despite the large surface area of the small intestine, malignant tumors occur here much less often than in the large intestine.
The main methods include surgical resection, chemotherapy and radiation therapy. In complex or common cases, modern approaches may be employed, including HIPEC, PIPAC, TACE, and immunotherapy.
Surgery is the main treatment for localized tumors. During the metastatic process, it is not always indicated. In case of intestinal obstruction, palliative surgery or stent placement may be necessary, even if radical removal of the tumor is not possible.
Yes. Chemotherapy is used both after surgery and during the metastatic process. In modern practice, it is sometimes combined with new methods, such as dendritic cell therapy, to increase the effectiveness of treatment and reduce side effects.
The prognosis is determined by the stage, histological type, and location of the tumor. In the early stages, the five-year survival rate may exceed 80%, while it decreases to about 40% when lymph nodes are affected. Carcinoid tumors usually have a better prognosis than adenocarcinomas.
Initially, the tumor usually spreads to regional lymph nodes and then to the liver through the portal venous system. Peritoneal metastasis detection is also possible. Current imaging techniques, particularly CT, allow these changes to be detected during staging.
The duration of recovery depends on the type of therapy. After major surgery, hospitalization usually lasts 10-14 days. The PIPAC procedure requires approximately 2-3 days in the hospital, and after endoscopic interventions, patients can often return home the same day.
The five-year survival rate is significantly stage-dependent: more than 80% in the early stages, about 40% in lymph node involvement, and 11-19% in the metastatic process. Rates are gradually improving thanks to early diagnosis and modern treatment methods.
Yes. Innovative approaches include HIPEC, PIPAC, dendritic cell immunotherapy and minimally invasive tumor ablation techniques.
With standard treatment, the two-year survival rate is about 25%. The use of modern techniques such as HIPEC, PIPAC, TACE or dendritic cell therapy can raise this to about 60%.
In the early stages, survival is significantly higher and often exceeds 80%. In common or metastatic forms, results may improve by combining standard therapy with modern treatments.
Traditional chemotherapy provides a response in less than 10% of cases. New approaches, including PIPAC or immunotherapy, can achieve a 45-65% response rate in eligible patients.
Standard therapy often involves multiple cycles over several months. Instead, minimally invasive or targeted methods, such as TACE or ablation, can be performed as several short procedures.
With traditional chemotherapy, fatigue, nausea and hair loss are often observed. Current techniques such as HIPEC or immunotherapy usually are associated with faster recovery.
Patients receiving innovative treatments tend to experience fewer side effects, spend less time in hospital, and return to their normal lives more quickly.
In Germany, innovative programs cost approximately 25,000-60,000€, while standard therapy can reach 150,000€. Prices are usually higher in the UK and US, and in Australia access to such methods is limited and often costs 3-4 times more.
Tactics depend on the location of the tumor, the degree of spread and biological features. For example, peritoneal metastases may be an indication for HIPEC or PIPAC, dominant liver metastases – to TACE, and dendritic cell therapy may be used as an additional method to activate the antitumor immune response.
The most complete approach is offered by specialized gastroenterological oncology centers with experience in the treatment of rare tumors. In particular, clinics in Germany that use modern technologies provide multidisciplinary treatment planning for each patient.
Countries with well-organized centralized oncology systems, particularly Germany, are considered among the best for treating rare gastrointestinal tumors. German multidisciplinary cancer centres provide access to modern therapies in accordance with international guidelines and offer individually tailored treatment strategies for patients with advanced or metastatic forms of the disease.
Choose treatment abroad and you will for sure get the best results!
Authors:
This article was edited by medical experts, board-certified doctors Dr. Nadezhda Ivanisova, and Dr. Bohdan Mykhalniuk. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Our editorial policy, which details our commitment to accuracy and transparency, is available here. Click this link to review our policies.
Sources:
[1] Alberto Puccini, Francesca Battaglin, Heinz-Josef Lenz. Management of Advanced Small Bowel Cancer. Curr Treat Options Oncol. 2018 Nov 5;19(12):69. doi: 10.1007/s11864-018-0592-3. [DOI] [PMC free article]
[2] Mirna H Farhat, Ali I Shamseddine, Kassem A Barada. Small Bowel Tumors: Clinical Presentation, Prognosis, and Outcome in 33 Patients in a Tertiary Care Center. J Oncol. 2008 Dec 2;2008:212067. doi: 10.1155/2008/212067. [DOI] [PMC free article]
[3] Tsunekazu Mizushima, Hiroshi Tamagawa, Hideyuki Mishima et al. The effects of chemotherapy on primary small bowel cancer: A retrospective multicenter observational study in Japan. Mol Clin Oncol. 2013 Jul 22;1(5):820–824. doi: 10.3892/mco.2013.150. [DOI] [PMC free article]
[4] John Spiliotis, Vasileios Kalles, Ioannis Kyriazanos et al. CRS and HIPEC in patients with peritoneal metastasis secondary to colorectal cancer: The small-bowel PCI score as a predictor of survival. Pleura Peritoneum. 2019 Oct 30;4(4):20190018. doi: 10.1515/pp-2019-0018. [DOI] [PMC free article]
[5] Yang Liu, Yutaka Yonemura, Edward A Levine et al. Cytoreductive Surgery Plus Hyperthermic Intraperitoneal Chemotherapy for Peritoneal Metastases From a Small Bowel Adenocarcinoma: Multi-Institutional Experience. Ann Surg Oncol. 2018 Feb 26;25(5):1184–1192. doi: 10.1245/s10434-018-6369-x. [DOI] [PMC free article]
[6] Sara K Daniel, Beatrice J Sun, Byrne Lee. PIPAC for Gastrointestinal Malignancies. J Clin Med. 2023 Oct 27;12(21):6799. doi: 10.3390/jcm12216799. [DOI] [PMC free article]
[7] Carolina Lanza, Velio Ascenti, Gaetano Valerio Amato et al. All You Need to Know About TACE: A Comprehensive Review of Indications, Techniques, Efficacy, Limits, and Technical Advancement. J Clin Med. 2025 Jan 7;14(2):314. doi: 10.3390/jcm14020314. [DOI] [PMC free article]
[8] Jirapat Wonglhow, Patrapim Sunpaweravong, Chirawadee Sathitruangsak et al. A 20-Year Real-World Study of Small Bowel Cancers: Histologic Subtypes, Clinical Features, and Survival Implications. J. Clin. Med. 2025, 14(19), 6962. doi: 10.3390/jcm14196962. [DOI]
[9] Sergiu Marian Cazacu, Dan Cârțu, Mihai Popescu et al. Small Bowel Tumors: A 7-Year Study in a Tertiary Care Hospital. Cancers 2025, 17(9), 1465, 6962. doi: 10.3390/cancers17091465. [DOI]
[10] Mikio Kajihara, Kazuki Takakura, Tomoya Kanai et al. Dendritic cell-based cancer immunotherapy for colorectal cancer. World J Gastroenterol. 2016 May 7;22(17):4275–4286. doi: 10.3748/wjg.v22.i17.4275. [DOI] [PMC free article]
[11] Roman Volchenkov, Florian Sprater, Petra Vogelsang, Silke Appel. The 2011 Nobel Prize in physiology or medicine. Scand J Immunol. 2012 Jan;75(1):1-4. doi: 10.1111/j.1365-3083.2011.02663.x. [DOI] [PubMed]
[12] Elbek Fozilov, Anthony Weng, Snigdha Kanadibhotla et al. State-of-the-Art Therapy in Peritoneal Carcinomatosis Management. Onco 2025, 5(2), 14. doi: 10.3390/onco5020014. [DOI]
Read:
New Effective Treatments for Stage 4 Cancer: Innovations in Oncology
Immunotherapy for Cancer Treatment
Dendritic cell therapy in cancer treatment in Germany - Vaccination against cancer