A benign brain tumor is a non-cancerous, slow-growing mass of cells in and around the brain tissue. It accounts for nearly 72% of all primary brain neoplasms, with an incidence of roughly 17.69 per 100,000 people [1]. Non-malignant primary central nervous system (CNS) tumors are more frequently diagnosed in females, with research indicating that they constitute approximately 64.4% of cases, in contrast to 35.6% observed in males [2]. The median age at diagnosis is approximately 61 years [3].
The attitudes of patients and healthcare professionals toward non-cancerous brain tumors are often contradictory. On the one hand, these tumors are not part of the oncological process – they grow slowly or even remain the same size, do not invade nearby tissues and organs, and stay at the site of origin without metastasizing. The usual 5-year relative survival rate is typically reported to be approximately 91.8%-95% for certain benign brain tumor types [4].
A benign neoplasm is the most favorable tumor type, which may cause no symptoms and require nothing more than active surveillance. On the other hand, even the tiniest tumors near vital centers of the brain can cause harm if they grow. Even a non-malignant neoplasm inside the skull is a potential cause of neurological problems.
In such a situation, healthcare professionals should make the decision that is most beneficial for the patient, as brain surgery always carries certain risks. Paying close attention to possible symptoms of non-cancerous brain tumors is very helpful for early diagnosis and successful treatment.
Comparison of Benign vs. Malignant Brain Tumors
| Characteristics | Benign Tumors | Malignant Tumors |
|---|---|---|
| Growth | Slow | Rapid and aggressive |
| Borders | Well-defined, localized | Irregular, jagged |
| WHO grade | I, II | III, IV |
| Invasiveness | Does not invade nearby tissue | Invades surrounding brain tissue |
| Reoccurrence | Rare | High |
| Impact on function | Can cause symptoms due to pressure | Causes progressive neurological damage |
| Prognosis | Often favorable | Differs, but can be lethal |
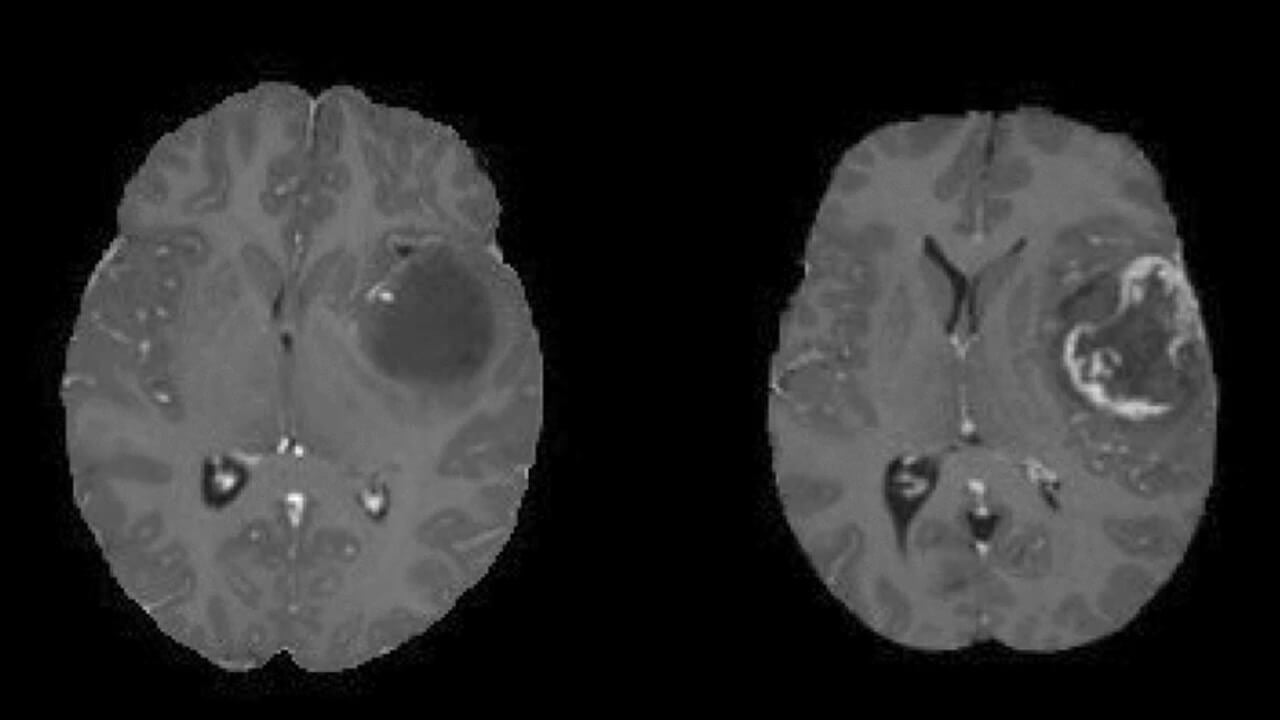
Symptoms of a benign brain tumor
Benign brain tumor symptoms can include general (which occur in many other diseases) and specific symptoms. This mainly depends on the tumor's localization and size.
Benign tumors can be considered when such signs are present [7].
- Severe recurrent headaches that worsen in the morning and do not respond to usual painkillers. Headaches can also occur during nighttime sleep and become more intense during physical exercise, coughing, or sneezing.
- Vomiting without objective causes (e.g., poisoning, intoxications, gastrointestinal problems, pregnancy). Vomiting may be preceded by nausea, but not always. It is unrelated to diet or food intake and can occur even on an empty stomach.
- A gradual, partial loss of hearing can be a sign of a schwannoma, as this tumor involves the hearing nerve. Compression of the nerve fibers can disrupt their function, leading to total deafness.
- Poor coordination is another sign of schwannoma. Unsteadiness and loss of balance arise from involvement of the balance nerve, a part of the vestibulocochlear nerve. Naturally, balance disturbances in non-cancerous brain tumors can`t be treated with usual drugs.
- A gradual, partial loss of vision occurs in tumors of the occipital lobe, where the visual center is located. In such cases, the eyes and optic nerves may perfectly perceive all the information, but the brain is unable to process it.
- Changes in smell perception arise in olfactory (smell) brain affection. Smell perception can be distorted or totally absent in advanced tumors.
- Weakness in the legs and arms, along with numbness, especially when it involves only one part of the body. These symptoms arise when large tumors compress the motor or sensory centers of the brain or alter cerebrospinal fluid flow, thereby affecting the spinal cord.
- Seizures and loss of consciousness are consequences of changes in the brain's electrical activity. High cortical excitability causes seizures and syncope.
- Changes in mental functions, e.g., memory (namely, short-term memory), speech, comprehension, and attentiveness. Such changes are usually gradual and stable and don`t depend on the previous level of intellectual activity.
- Stable changes in personality – mood (depression and loss of energy), behavior, and personal preferences. Undoubtedly, people can acquire new features over time, but sudden and unexplained changes should draw attention.
Naturally, it is much better to detect and remove a benign mass on brain while it is "silent" (asymptomatic) and causing no harm to delicate brain tissue. Another important point is precise diagnosis after symptoms appear.

What causes benign brain tumors?
Although benign tumors are more prevalent than malignant tumors, their etiology remains unclear. Based on clinical practice data and research, we can identify the following causes of brain tumor cancer:
- Age. The older you are, the higher the risk of developing a benign tumor is.
- Race. In general, brain tumors are more widespread among Caucasians compared to Europeans.
- Pathology and traumas during pregnancy (inherited non-cancerous brain tumors).
- Family history of brain tumors. Some types of tumors are connected with genetic conditions – for example, Turcot syndrome, neurofibromatosis, and tuberous sclerosis.
- Radiation exposure. This involves both treatments with ionizing radiation and accidental exposure during work or emergencies.
- Exposure to certain chemicals (e.g., vinyl chloride, formaldehyde). In case you work with dangerous substances, you should always use personal protective equipment.
Another widely discussed topic is whether there is a link between brain tumor development and mobile phone use. Indeed, cell phones emit radiofrequency energy (radio waves), a form of non-ionizing radiation. This energy easily penetrates the skin and reaches nearby tissues and organs. During a phone call, the brain is the organ closest to the source of radiofrequency energy. If a person spends a long time on the phone, the strength of this exposure increases.
Several studies and reviews have been conducted to investigate this issue in greater detail, given the ubiquity of mobile phones today. As a result, National Institute of Health (NIH) studies have found no association between cell phone use and the incidence of non-cancerous brain tumors. This finding has been further confirmed by other healthcare organizations and institutions. The U.S. Food and Drug Administration (FDA) has also issued a statement on the safety of cell phone use for public health [8].
Types of Benign Brain Tumors
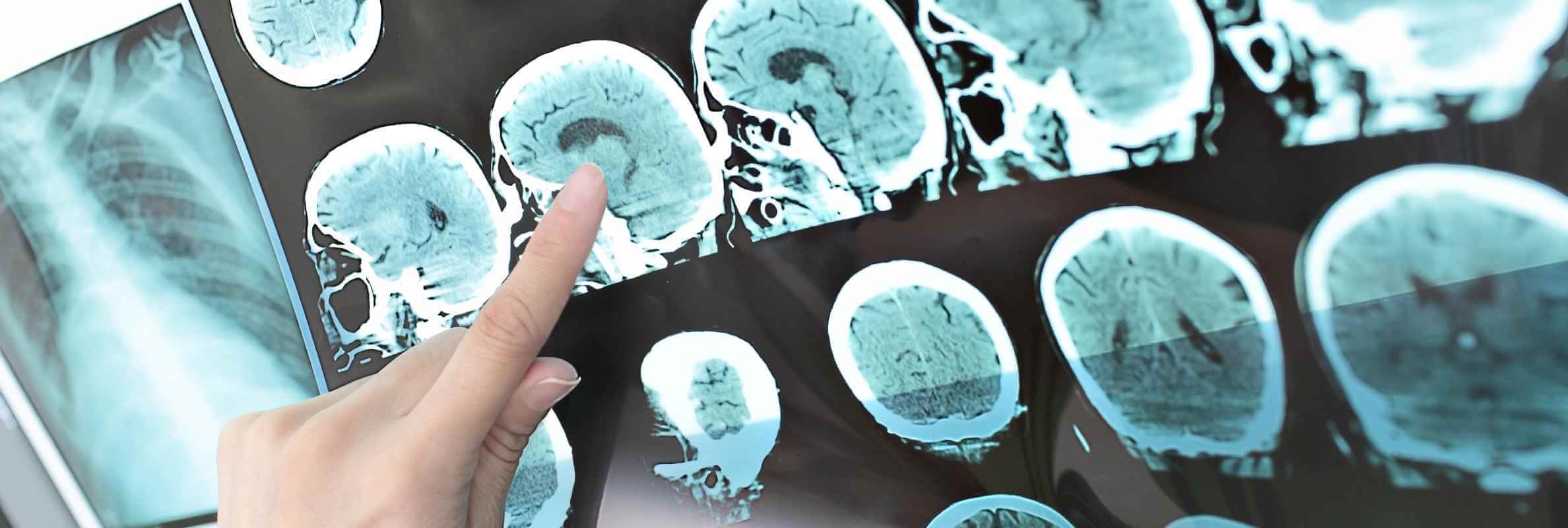
Virtually every cell in the brain can be the origin of a tumor. Nevertheless, some cells, such as neurons, are less likely to form a tumor because they don`t divide. Other cells, such as those of blood vessels or the pituitary gland, are more physiologically active and thus can be the structural basis of a tumor. The cell type determines the tumor's location, the rate of its growth, and its ability to produce excessive amounts of hormones. The diagnosis often relies on an MRI for a benign brain tumor.
The most important benign brain tumor types are described below.
Meningioma
Meningioma benign brain tumor, is rather widespread and accounts for almost 20% of all brain tumors. It arises not from the nervous tissue directly but from the meninges – the three membranes (namely, the dura mater, the arachnoid mater, and the pia mater) that cover the brain and spinal cord to feed them and protect them from injuries. Thus, meningioma disease usually grows on the surface of the brain without invading deeper tissues. This type of tumor can potentially become quite large and reach 2-5 cm in size. Symptoms of meningioma include headaches that are often worse in the morning, seizures, vision changes, hearing loss, memory loss, and weakness in limbs.
We have already mentioned genetic risk factors, and meningioma brain tumors are exactly from the group of such neoplasms – they are associated with neurofibromatosis type 2. Meningioma prognosis for the five-year survival rate is around 88.2% after diagnosis [9].
Schwannoma
Schwannoma, and its subtype acoustic neuroma, ranks second in incidence and accounts for about 9% of all brain tumors. This tumor originates from the cranial nerves, particularly the 8th (the vestibulocochlear nerve, which includes the balance and hearing nerves), specifically from its Schwann cells. Schwann cells form the outer layer of the nerve, produce myelin, and support and insulate nerve tissue. Schwannomas usually don`t change location and don`t spread along the nerve. Acoustic neuroma clinical features include hearing and balance; larger tumors can influence facial sensation and movement. The good news is that schwannomas grow slowly or even remain stable in size. This tumor is also associated with neurofibromatosis type 2 and shows a correlation with age – it mainly affects people between the ages of 30 and 60.
Pituitary adenoma
A pituitary adenoma arises in the pituitary gland. The incidence of this tumor is similar to that of schwannomas and accounts for about 8% of brain tumors. Nevertheless, pituitary adenoma is the most frequently encountered tumor because it can be hormone-producing and cause a wide variety of complaints and clinical signs. Pituitary adenoma symptoms often include disruptive cycle and fertility problems, acromegaly, weight gain, and muscle weakness. There are two main types of pituitary adenomas – pituitary microadenomas, which are less than 10 mm in size, and pituitary macroadenomas, which are greater than 10 mm in size. About 65% of all pituitary adenomas produce hormones; these are usually microadenomas [10]. The most common hormone produced by microadenomas is prolactin. Other possible hormones include growth hormone (GH), adrenocorticotropin (ACTH), and thyrotropin (TSH). Macroadenomas are hormonally inactive but can affect nearby tissues due to their greater size. Tumors with mixed hormone secretion can occur as well.
Hemangioblastoma
Hemangioblastomas originate in the blood vessels of the brain. As a vital organ, the brain requires a rich supply of oxygen and nutrients, so its blood flow is extensive. Nevertheless, brain vessels are usually protected by internal mechanisms, and the incidence of this tumor type is only 2% of all brain tumors. Hemangioblastomas can also grow outside brain tissue, but they can press on the brain once they are large enough. Sometimes the tumor is not solid but rather forms a cyst or a closed sac. The development of hemangioblastomas is associated with von Hippel-Lindau (VHL) syndrome, an inherited condition. However, they can also arise sporadically in otherwise healthy people.
Craniopharyngioma
Craniopharyngioma is more often found in children but can also affect adults. The incidence of this tumor accounts for about 1%-3% of all brain tumors. It arises from remnants of Rathke's pouch (nasopharynx) and is associated with abnormal fetal development during pregnancy. Craniopharyngioma is usually a cystic tumor. It is called "a tumor with benign cellular structure and malignant behavior" because it tends to invade surrounding structures and recur after resection. Craniopharyngiomas are usually located near two important endocrine glands – the pituitary gland and the hypothalamus – and can directly influence hormone levels when they are large enough. Craniopharyngioma treatment can be performed at any age, depending on the patient's general condition and clinical indications.
Choroid plexus papilloma
Choroid plexus papilloma is more common in children and accounts for less than 1% of CNS tumors. The choroid plexus is a network of blood vessels that surrounds the ventricles and produces cerebrospinal fluid (CSF). Active cell proliferation in this region leads to the formation of a solid, vascular tumor and, consequently, to interruption of cerebrospinal fluid flow. Choroid plexus papilloma grows slowly, as all non-cancerous brain tumors do, but in the most complicated cases, it can completely block the flow of CSF. This tumor type also has a genetic basis – in certain cases, it is associated with a mutation in the TP53 gene.
Dermoid cysts
Epidermoid and dermoid cysts (tumors) are uncommon lesions. These "tumors" are not solid structures but hollow cysts (sometimes filled with fluid). Most healthcare professionals consider them benign tumors due to their intracranial (inside the skull) location and possible influence on brain tissue.
Explore advanced brain tumor treatment options in Germany
Are benign brain tumors dangerous?
Non-cancerous brain tumors are not dangerous in themselves, as they do not invade surrounding tissues or metastasize, deprive healthy tissues of nutrients, produce toxic degradation products, harm blood vessels, or cause bleeding. Small benign tumors are often asymptomatic and may be discovered only by chance.
Nevertheless, in certain circumstances, living with a benign brain tumor can affect a person's overall health, cause symptoms, and even be life-threatening.
The main mechanisms of harmful influence are the following:
- Pressure on surrounding tissues, including vital centers. As already mentioned, benign tumors are clearly separated from surrounding tissues and sometimes even have an additional capsule. At the same time, each neoplasm puts pressure on nearby structures. Even a slight force can be significant when it affects vital centers, such as the respiratory or motor centers, because brain tissue is highly specialized.
- Increased overall brain volume. The bones of the human skull are tightly connected, so the skull has a strictly limited volume. The size of a healthy brain, with its meninges and blood vessels, fits this volume perfectly. Each benign tumor occupies a certain volume, which is added to the overall volume. Initially, compensatory mechanisms smooth this difference, but this becomes impossible as the tumor grows. Compression of the brain leads to swelling and additional damage. In such cases, neurological symptoms, including seizures, arise almost immediately.
- Blocking cerebrospinal fluid flow. This mechanism is specific to choroid plexus papilloma, especially in young patients. The tumor can produce excessive cerebrospinal fluid, increasing pressure within the system. Another possible problem is the direct obstruction of fluid flow when a tumor grows into the lumen of the spinal canal. In such cases, the process can also disturb the state and functions of the spinal cord.
In many cases, surgery is recommended, and benign brain tumor surgery recovery is a steady process with positive results. It is important to choose among the best hospitals for benign brain tumor treatment to have access to multidisciplinary teams, advanced technologies, and the best possible care.
Treatment Options for Benign Brain Tumors
Treatment options depend on different factors like tumor size and location within the brain tissue, growth rate, and the symptoms that the patient experiences. Even if tumors are non-cancerous, they still pose a great danger by pressing on nearby brain structures. That's why there are different treatment approaches to control growth and relieve symptoms.
Neurosurgical Removal of Benign Brain Tumors
Surgery is one of the main treatment approaches that is aimed at removing the tumor completely. Modern procedures have improved safety guidelines and guarantee better results, including clearer resection margins and more precise tumor localization. The main modern neurosurgical procedures are:
- Minimally invasive (keyhole) surgery. It is performed from the small strategically placed incisions with specialised, precise instruments. This allows for reduced postoperative trauma and faster recovery compared to traditional open surgery.
- Awake brain surgery (awake craniotomy). During the procedure, the patient remains awake to provide real-time speech, movement, and cognitive monitoring. It helps prevent damage to important brain areas.
- Endoscopic brain surgery. The special tube with a camera is inserted through the small opening with all the necessary instruments. It is an excellent option for tumors located deep within the brain.
- Neuronavigation systems. It is a modern, important part of any neurological procedure that integrates preoperative MRI or CT scans to create a 3D map of the brain. It helps surgeons precisely plan the surgical path, avoid critical structures, and improve the accuracy of neoplasm removal.
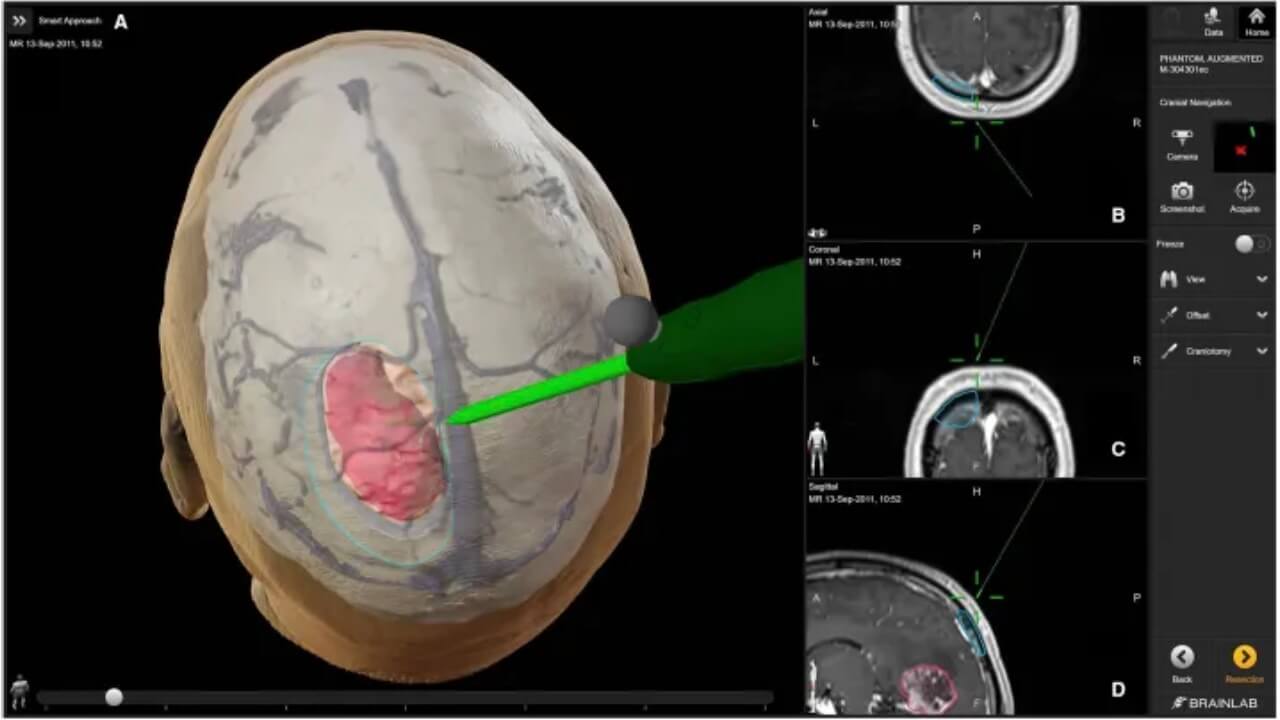
Radiotherapy Treatment for Benign Brain Tumors
Radiotherapy is a treatment that uses high-energy radiation to destroy tumor cells. It is a main option for inoperable tumors where surgery carries a high risk due to the tumor’s location. Modern radiotherapy approaches include intensity-modulated radiation therapy (IMRT) and stereotactic radiosurgery (SRS), which aim to deliver radiation precisely to the neoplasm.
Proton Therapy for Benign Brain Tumors
It is a type of therapy that uses proton beams to deliver radiation to the location of a neoplasm. It is made for benign brain tumors located near critical structures such as the optic nerves, brainstem, or spinal cord. Proton therapy offers the wonderful benefit of its high precision. Protons release most of their energy directly at the tumor site (the Bragg peak). This approach minimizes radiation exposure to surrounding healthy brain tissue. It is particularly important for younger patients.
Dendritic Cell Therapy for Benign Brain Tumors
Dendritic cell vaccination (DCV) is a personalised treatment approach that aims to train your own immune system to find and destroy tumors more effectively. Dendritic cells are a specialized type of immune cell that can modulate the immune response to a specific antigen. Even if the neoplasm is non-cancerous, it still can be targeted by DCV. The process starts with collecting blood from the patient, followed by the extraction of dendritic cells and their activation in laboratory settings. When the vaccine is administered to the patient, it starts working immediately and helps achieve a long-lasting antitumor response.
Hospital Selection for Benign Brain Tumor Treatment
Choosing the right hospital is an important step towards successful treatment of a brain neoplasm. It can directly influence the outcomes and mostly depends on the level of the medical facility. There are some of the main key factors that you, as a patient, need to consider before choosing a treatment center:
- Neurosurgical expertise. As the surgery is one of the main steps of the treatment process, the experience of the medical team matters. Neurosurgeons who specialise in complex and delicate cases tend to achieve better outcomes with lower complication rates. Particular attention should be given to centers with expertise in skull base surgery, as these tumors are often located near vital structures.
- High-quality imaging and navigation technologies. It is an essential diagnostic tool for successful treatment planning. Imaging provides improved surgical precision, which can help preserve vital functions such as speaking, walking, or seeing.
- Multidisciplinary team. The best centers bring together a team of neurosurgeons, neurologists, oncologists, radiologists, and radiation specialists to evaluate each case and create a personalized treatment plan to help the patient achieve the most favorable result possible and bring the disease under control.
- Radiosurgery and advanced radiation techniques. They are important procedures for patients whose tumors cannot be removed surgically due to various reasons or those who require additional therapies after surgery.
A Medical Journey: Every Step of the Way With Booking Health
Finding the best treatment strategy for your clinical situation is a challenging task. Being already exhausted from multiple treatment sessions, having consulted numerous specialists, and having tried various therapeutic interventions, you may be lost in all the information given by the doctors. In such a situation, it is easy to choose a first-hand option or to follow standardized therapeutic protocols with a long list of adverse effects instead of selecting highly specialized innovative treatment options.
To make an informed choice and get a personalized cancer management plan, which will be tailored to your specific clinical situation, consult medical experts at Booking Health. Being at the forefront of offering the latest medical innovations for already 12 years, Booking Health possesses solid expertise in creating complex cancer management programs in each case. As a reputable company, Booking Health offers personalized bening brain tumor treatment plans with direct clinic booking and full support at every stage, from organizational processes to assistance during treatment. We provide:
- Assessment and analysis of medical reports
- Development of the medical care program
- Selection of a suitable treatment location
- Preparation of medical documents and forwarding to a suitable clinic
- Preparatory consultations with clinicians for the development of medical care programs
- Expert advice during the hospital stay
- Follow-up care after the patient returns to their native country after completing the medical care program
- Taking care of formalities as part of the preparation for the medical care program
- Coordination and organization of the patient's stay in a foreign country
- Assistance with visas and tickets.
- A personal coordinator and interpreter with 24/7 support
- Transparent budgeting with no hidden costs
Health is an invaluable aspect of our lives. Delegating management of something so fragile yet precious should be done only to experts with proven experience and a reputation. Booking Health is a trustworthy partner who assists you on the way of pursuing stronger health and a better quality of life. Contact our medical consultant to learn more about the possibilities of personalized treatment with innovative methods for brain tumors with leading specialists in this field.
Real Stories, Real Results: Meet Booking Health International Patients
Frequently Asked Questions About Benign Brain Tumors
Send request for treatmentA benign brain tumor is a non-cancerous cell growth in the brain that tends to grow slowly and not invade surrounding tissues.
Yes, the benign brain tumor complications can include a stroke if the growth compresses blood vessels or interferes with normal cerebral blood flow.
One of the primary approaches is benign tumor surgery, which involves the removal of the growth and alleviates pressure on the surrounding brain tissue.
Benign brain tumor treatment without surgery can include close monitoring of the tumor via imaging, as well as medications to manage symptoms and radiotherapy.
Most tumors do not disappear spontaneously; however, due to their slow growth, they can remain stable for years without causing complications.
Currently, there is no established method to prevent brain tumors; however, minimizing risk factors, early detection, and regular medical check-ups may contribute to risk reduction.
With precise and individualized management, individuals with non-cancerous brain tumors often achieve normal life expectancies and can sustain a good quality of life.
The benign brain tumor survival rate is generally very high, ranging from 85% to 95%, especially when the tumor is removed surgically or monitored effectively.
Recovery varies by tumor size and location, but most patients return to normal activities within a few months following benign brain tumor removal.
Although these lesions are benign, they may cause neurological complications and symptoms due to compression of vital brain tissue, nerves, or blood vessels. Typically, management involves surgical intervention, radiation therapy, or, at the very least, lifelong surveillance.
Treatment for non-cancerous brain tumors involves surgical procedures aimed at the physical removal of the neoplasm to provide immediate relief. Non-surgical treatments of benign brain tumor—such as radiation therapy, monitoring, or pharmacological therapy—are used for small, deep-seated, or high-risk tumors to control growth, manage symptoms, or address cases that are inoperable.
Choose treatment abroad, and you will get the best results for sure!
Authors:
This article was edited by medical experts, board-certified doctors Dr. Nadezhda Ivanisova, and Dr. Yana Dmytryshyn. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Our editorial policy, which details our commitment to accuracy and transparency, is available here. Click this link to review our policies.
Source:
[1] Quinn T Ostrom, Mackenzie Price, Corey Neff et al. CBTRUS Statistical Report: Primary Brain and Other Central Nervous System Tumors Diagnosed in the United States in 2015–2019. Neuro Oncol. 2022 Oct 5;24(Suppl 5):v1–v95. doi: 10.1093/neuonc/noac202. [DOI] [PMC free article]
[2] Quinn T Ostrom, Mackenzie Price, Corey Neff et al. CBTRUS Statistical Report: Primary Brain and Other Central Nervous System Tumors Diagnosed in the United States in 2015-2019. Neuro Oncol. 2022 Oct 5;24(Suppl 5):v1-v95. doi: 10.1093/neuonc/noac202. [DOI] [PubMed]
[3] Kyung Moo Kim, Rachel Jane Lew, Tate Justin Higashihara et al. Differences in tumor size, clinical, demographic, and socioeconomic profiles of central nervous system tumors among a racially diverse cohort: A retrospective case–control study. Surg Neurol Int. 2024 Dec 13;15:459. doi: 10.25259/SNI_190_2024. [PMC free article]
[4] A Woehrer, M Hackl, T Waldhör et al. Relative survival of patients with non-malignant central nervous system tumours: a descriptive study by the Austrian Brain Tumour Registry. Br J Cancer. 2013 Nov 19;110(2):286–296. doi: 10.1038/bjc.2013.714. [DOI] [PMC free article]
[5] Hari Mohan Rai, Joon Yoo & Serhii Dashkevych. Two-headed UNetEfficientNets for parallel execution of segmentation and classification of brain tumors: incorporating postprocessing techniques with connected component labelling. J Cancer Res Clin Oncol 150, 220 (2024). doi: 10.1007/s00432-024-05718-1. [DOI]
[6] Soumick Chatterjee, Faraz Ahmed Nizamani, Andreas Nürnberger & Oliver Speck. Classification of brain tumours in MR images using deep spatiospatial models. Sci Rep 12, 1505. 2022. doi: 10.1038/s41598-022-05572-6. [DOI]
[7] Mia Schmidt-Hansen, Sabine Berendse, William Hamilton. Symptomatic diagnosis of cancer of the brain and central nervous system in primary care: a systematic review. Fam Pract. 2015 Oct 14;32(6):618–623. doi: 10.1093/fampra/cmv075. [DOI] [PMC free article]
[8] FDA. Cell Phones.
[9] Yu-Chi Wang, Chi-Cheng Chuang, Kuo-Chen Wei et al. Long Term Surgical Outcome and Prognostic Factors of Atypical and Malignant Meningiomas. Sci Rep 6, 35743 (2016). doi: 10.1038/srep35743. [DOI]
[10] Mark E Molitch. Diagnosis and Treatment of Pituitary Adenomas: A Review. JAMA. 2017 Feb 7;317(5):516-524. doi: 10.1001/jama.2016.19699. [DOI] [PubMed]
[11] Albert Joseph Sulangi, Adam Husain, Haoyi Lei, Jessica Okun. Neuronavigation in glioma resection: current applications, challenges, and clinical outcomes. Front. Surg. 11:1430567. doi: 10.3389/fsurg.2024.1430567. [DOI]
Read:
Comprehensive Guide to Brain Cancer Treatment: New and Standard Treatment Options