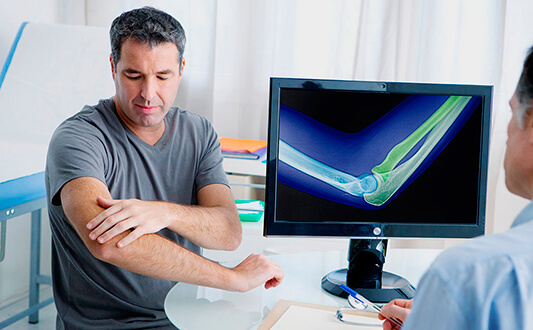
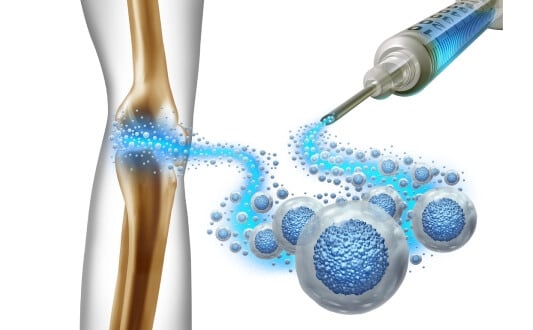
Arthrosis (osteoarthritis) is a non-inflammatory joint disease that causes cartilage degeneration and joint surface defects. This is the most common connective tissue disease. Its incidence among joint diseases accounts for 70%. It is believed that 20% of the world's population is diagnosed with arthrosis of varying severity.
The prevalence of the disease among people over the age of 50 reaches 50%. In people after the age of 70, the occurrence of arthrosis exceeds 80%.
Content
- Causes of arthrosis
- Symptoms of arthrosis
- Diagnosis of arthrosis
- Treatment of arthrosis abroad
- Prognosis
- Hospitals and cost of treatment
- Treatment of arthrosis in foreign hospitals with Booking Health
Causes of arthrosis
There are two causes of the development of arthrosis. The first is an excessive functional load on the joint, while the second one is a reduction of resistance to a normal load on the joint, as a result of which it becomes conditionally excessive. Consequently, a degeneration of articular cartilage develops.
Risk factors for arthrosis:
- Obesity
- Heredity
- Age of over 50 years old
- Strenuous physical labour
- Sports
- Accompanying joint pathologies
Depending on the cause of the disease, arthrosis can be primary (idiopathic) or secondary.
- Primary arthrosis occurs in the most clinical cases of this pathology. It is characterised by the lack of a causal link between the degeneration of the articular cartilage and external or internal factors that have caused the pathological process.
- Secondary arthrosis is diagnosed in case of such an obvious link. It can be a systemic disease of the connective tissue, trauma, the outcome of an acute inflammatory process, endocrine diseases.
Symptoms of arthrosis
Arthrosis usually begins with the lesion of a single joint. The main clinical symptom is pain. Arthrosis is characterised by several types of pain syndrome. Most patients experience mechanical pain. It occurs upon the carrying of loads and disappears or subsides at rest. Pain also often intensifies during the day and subsides after rest.
Other symptoms:
- Swelling of the joint
- Joint stiffness
- Development of muscle contractures
- Cracking in the joint while walking
- Occurrence of subluxations
- Crawling and burning sensations
- Deformation of joints
- Atrophy of the adjacent muscles
The disease has the following clinical signs, which depend on the location of the pathological process:
- Hip osteoarthritis (coxarthrosis). The condition accounts for 25% of all its cases. The most severe form of arthrosis often develops against arthritis. Menopause can be a trigger factor in females. The pain is initially mild but eventually progresses. Movement disorders develop quite quickly. As a result, a person develops a waddling gait.
- Knee osteoarthritis (gonarthrosis). It has a more favourable clinical course than coxarthrosis. The main symptom is pain, which is usually felt on the inside of the joint. Over time, the patient develops reduced mobility. Initially only bending is limited and later knee straightening becomes restricted as well. In 40% of patients the joint is deformed and increased in volume. An atrophy of the muscles of the thigh and lower leg can develop.
- Osteoarthritis of distal interphalangeal joints. It accounts for about 20% of cases of arthrosis. This condition has another name - Heberden's nodes. It usually develops in postmenopausal women. In the course of this form of disease, deformity of the joints often occurs earlier, before the pain manifests itself. The passive movements show lateral hypermobility of the distal interphalangeal joints.
- Osteoarthritis of proximal interphalangeal joints. Another name of the condition is Bouchard's nodes. In 50% of the cases it is combined with Heberden's nodes. The pain syndrome is usually absent or mild. The fingers become spindle-shaped, which is associated with the formation of nodules on the lateral surfaces of the proximal interphalangeal joints.
- Elbow osteoarthritis. The condition is rare. The joint mobility is severely limited due to the bone growth around the joint surface of the ulna.
- Shoulder osteoarthritis. It is a rare disease. It develops after a fracture of the head of the humerus or as a result of chondrocalcinosis. The main symptom is painful shoulder abduction. There is no deformity of the shoulder joint. The condition is characterised by the muscle atrophy of the shoulder girdle in the pathological process. As the disease progresses, the shoulder abduction becomes limited.
- Ankle Arthritis. The condition develops due to the trauma. The primary form of arthrosis of this location practically does not occur. The disease progresses rapidly, causing a sudden disorder of joint mobility and disability of the patient.
- Osteoarthritis of intervertebral joints. The condition is also called facet syndrome. It is manifested by pain and a slowly progressing limitation of the mobility of the spine. While performing either active or passive movements, one can hear crunching in the affected joints. In the mornings a person can feel stiffness but during the day it subsides.

Diagnosis of arthrosis
The diagnosis is based on x-ray. Criteria for osteoarthritis diagnosis:
- Osteophytes (marginal bone growths)
- Narrowing of the joint space
- Increased bone density (subchondral sclerosis)
The subsidiary criteria of diagnosis include subluxations, erosion and cysts in the areas of the greatest mechanical loads.
Based on radiographic findings, arthrosis can have the following stages:
- Stage 1 - doubtful signs
- Stage 2 – very few osteophytes, minimal narrowing of the joint space
- Stage 3 - multiple osteophytes, a pronounced narrowing of the joint space
- Stage 4 - multiple coarse osteophytes and there is almost no joint space
Such diagnostic methods as MRI, CT, bone scan and arthroscopy are more accurate but not always available in poorly equipped hospitals. German medical institutions carry out all these diagnostic measures, if necessary, and therefore it is possible to accurately determine the stage of arthrosis and to choose an effective treatment.
Treatment of arthrosis abroad
A patient with osteoarthritis needs comprehensive and continuous treatment. It includes not only therapeutic measures carried out within the medical institution, but also a drastic improvement in lifestyle.
The main goals of the treatment:
- Delayed development of arthrosis
- Elimination or reduction of symptoms
- Restoration or maintenance of working ability
- Restoration of the joint surface using surgical techniques
Treatment methods:
- Physical therapy
- Unloading joints
- Compliance with orthopaedic treatment
- Physiotherapeutic procedures (the best analgesic effect is achieved through the ultrasound action on the joint)
- Spa treatment
The following drugs are used to relieve symptoms and improve a functional state of the joint:
- Analgesics
- Chondroprotectors
- Glucocorticoids
- Hyaluronic acid for intra-articular administration
European hospitals widely use various procedures and medical manipulations that makes its possible to achieve a long-term improvement in the patient's condition and delayed progression of the disease.
These include:
- Laser therapy
- Intraosseous blockades
- Decompression of the epiphyseal cartilage
- Multichannel electrostimulation
The further development of arthrosis may require surgery. Most patients undergo joint replacement. The surgery involves the replacement of patient’s own joint with an artificial prosthesis.
Prognosis
A natural course of the disease has an unfavourable prognosis. Despite the progressive radiographic signs of arthrosis, some patients have a stable joint for many years. Nevertheless, the condition eventually causes a complete destruction of the articular cartilage, which is accompanied with the development of ankylosis (complete immobility of the joint) or neoarthrosis (unnatural mobility).
German hospitals offer highly effective and timeous treatment of osteoarthritis, which can significantly improve the outcome of the disease. The use of conservative and surgical treatments can restore a patient’s working ability at any stage of the pathological process.
Hospitals and cost of treatment
Patients with arthrosis undergo treatment in the Departments of Orthopedics and Traumatology, with the participation of specialists in the field of conservative and surgical treatment, as well as physiotherapists and rehabilitation therapists. Leading hospitals that treat patients with arthrosis of large and small joints are as follows:
- Academic Hospital DRK Berlin Westend, Department of Orthopedics, Traumatology and Endoprosthetics
- Catholic Clinic Koblenz-Montabaur, Department of Adult and Pediatric Orthopedics, Traumatology, Endoprosthetics
- Academic Hospital Brothers of Mercy Munich, Department of Orthopedics and Traumatology
- Academic Municipal Hospital Karlsruhe, Department of Adult and Pediatric Traumatology, Hand and Orthopedic Surgery
- Vitos Orthopedic Clinic Kassel, Department of Adult and Pediatric General Orthopedics, Trauma Surgery
The cost of treatment depends on the affected joint and the type of medical program. For example, the average cost of treating arthrosis of the hip joint is as follows:
- Diagnostics and conservative treatment of hip arthrosis – €8,430
- Treatment of hip arthrosis with arthroscopic surgery – €14,600
- Treatment of hip arthrosis with autologous conditioned plasma – €7,885
- Hip replacement – €27,525
- Bilateral hip replacement – €34,620
- Hip replacement with rehabilitation – €36,350
- Orthopedic rehabilitation after completion of the main treatment course – €970 per day
Treatment of arthrosis in foreign hospitals with Booking Health
Germany has many reputable hospitals specialising in the treatment of arthrosis. To choose the most suitable one, feel free to use the international online-platform Booking Health.
Booking Health offers help in such important aspects:
- Choosing the right clinic based on the annual qualification profile
- Establishing communication directly with your doctor
- Preparing medical program in advance, without repeating previous examinations
- Providing favorable costs, without overpricing and additional coefficients for foreign patients (saving up to 50% from the initial cost estimation)
- Booking the appointment on the necessary date
- Monitoring medical program at all stages
- Help in buying and forwarding of medicines
- Communication with the clinic after treatment completion
- Control of invoices and return of unspent funds
- Organization of additional examinations, rehabilitation, follow-up
- Offering service of the highest level: booking hotels and plane tickets, transfer organization
- Services of interpreter and personal medical coordinator
If you cannot book the necessary medical program on your own, you can leave a request on the website. Our medical advisor will clarify the details of your health condition, select a suitable hospital and a treatment program.
Choose treatment abroad and you will for sure get the best results!
Authors:
The article was edited by medical experts, board certified doctors Dr. Nadezhda Ivanisova and Dr. Vadim Zhiliuk. For the treatment of the conditions referred to in the article, you must consult a doctor; the information in the article is not intended for self-medication!
Sources:
Centers for Disease Control and Prevention
Articles for Orthopaedic Practice - Orthogate
Read:
How are dendritic cells changing rheumatoid arthritis treatment strategies?